Each year, around 700,000 hospitalizations for Chronic Obstructive Pulmonary Disease (COPD) occur in the U.S., with 20 percent of patients readmitted within 30 days. To address higher-than-expected readmission rates, MultiCare Health System implemented a NOREADMITS bundle, utilizing its analytics platform to enhance patient outcomes and reduce the rates of COPD readmissions.
Nationally, approximately 700,000 hospitalizations occur each year with the principle diagnosis of Chronic Obstructive Pulmonary Disease (COPD), with one in five patients being readmitted within 30 days. Even with a national cost for each COPD readmission costing between $9,000 and $12,000, evidence-based measures that improve patient outcomes and decrease COPD readmissions are largely lacking.
When reviewing organizational performance for 30-day all cause readmission, MultiCare Health System identified COPD as one of the top two readmission diagnoses, along with a rate higher than expected. This prompted the organization to take action. MultiCare implemented a NOREADMITS bundle, using the Health Catalyst Analytics Platform and integrating performance measures for each element of the bundle.
Chronic Obstructive Pulmonary Disease (COPD), a common preventable and treatable disease characterized by persistent respiratory symptoms and airflow limitation caused by significant exposure to particles or gases, is responsible for approximately 135,000 deaths annually, making it the third leading cause of death in the United States.1
Even though an estimated 700,000 hospitalizations occur nationally each year with the principle diagnosis of COPD and one in five of these COPD patients are readmitted within 30 days of discharge, evidence-based measures specifically for COPD readmission avoidance are lacking. The national cost for such readmissions is between $9,000 and $12,000 each.2,3,4
MultiCare Health System is a not-for-profit healthcare organization with more than 10,000 employees and a comprehensive network of services throughout Washington state’s Pierce, South King, Thurston, and Kitsap counties. It has long been committed to standardizing patient care to improve the overall quality of care and outcomes for its patients. One priority focus for MultiCare is 30 day-all-cause-readmissions. Through the implementation of standardized workflows, evidence-based guidelines, and analytics, MultiCare has demonstrated success in reducing the readmission rate for patients with heart failure (HF).
When reviewing organizational performance for 30 day-all-cause-readmissions, MultiCare identified that COPD was one of the top two readmission diagnosis, and that rate was higher than expected according to risk-adjusted benchmarks. Additionally, many of the patients being readmitted for HF, the number one readmission diagnosis, also had COPD. This presented a clear opportunity to improve readmission rates for patients with COPD.
Unlike HF, few evidence-based measures specific to COPD are available. Many patients with COPD are managed by primary care providers (PCPs) rather than specialists, substantially widening the number of providers who must have an adequate understanding of the most recent COPD care guidelines. It also makes effective handoff to the outpatient setting a priority, as a PCP could be managing up to 2,000 patients at any given point in time.
MultiCare needed an organizational strategy that would improve patient care processes and readmission rate for patients with COPD.
At MultiCare, Clinical Collaboratives, permanent, interdisciplinary teams of clinicians, support staff, data analysts, and operational leaders, are responsible for improving patient care and outcomes by eliminating variation. To improve the quality of care and outcomes for patients with COPD, MultiCare leadership turned to the Medicine Collaborative, which went to work immediately, developing and implementing a comprehensive strategy for improving care of patients with COPD.
The Medicine Collaborative developed care guidelines, outlining standard, evidence-based practices for the management of COPD. These guidelines standardize and improve the appropriate delivery of pharmacologic treatment and non-pharmacologic treatment, including smoking cessation counseling, vaccinations, medications, oxygen, patient education materials and action plans, and pulmonary rehabilitation.
The care guidelines are then integrated into the standard order sets for both admission and discharge, improving the consistency and reliability of care. To improve utilization of the orders sets, members of the Medicine Collaborative proactively sought feedback from ordering providers, asking how the order sets could be improved, and inquiring what changes could be made to increase usage.
While the development and availability of evidence-based order sets is an incredibly important piece of the improvement plan, the Medicine Collaborative recognized that availability alone would not lead to improvement.
The team needed to hardwire utilization of the order sets, and needed to redesign the workflow of the interdisciplinary team to implement best practices that would reduce the rate of readmission for patients with COPD.
To ensure improvement goals were achieved, the Medicine Collaborative applied learnings from the Heart Failure (HF) improvement team at MultiCare. The HF improvement team had successfully developed and implemented the NOREADMITS bundle, improving the readmission rate for patients with HF. The Medicine Collaborative elected to follow the HF improvement team’s lead, implementing the NOREADMITS bundle for patients with COPD. The NOREADMITS bundle includes key interventions to improve transitions of care and safe discharge from the hospital.
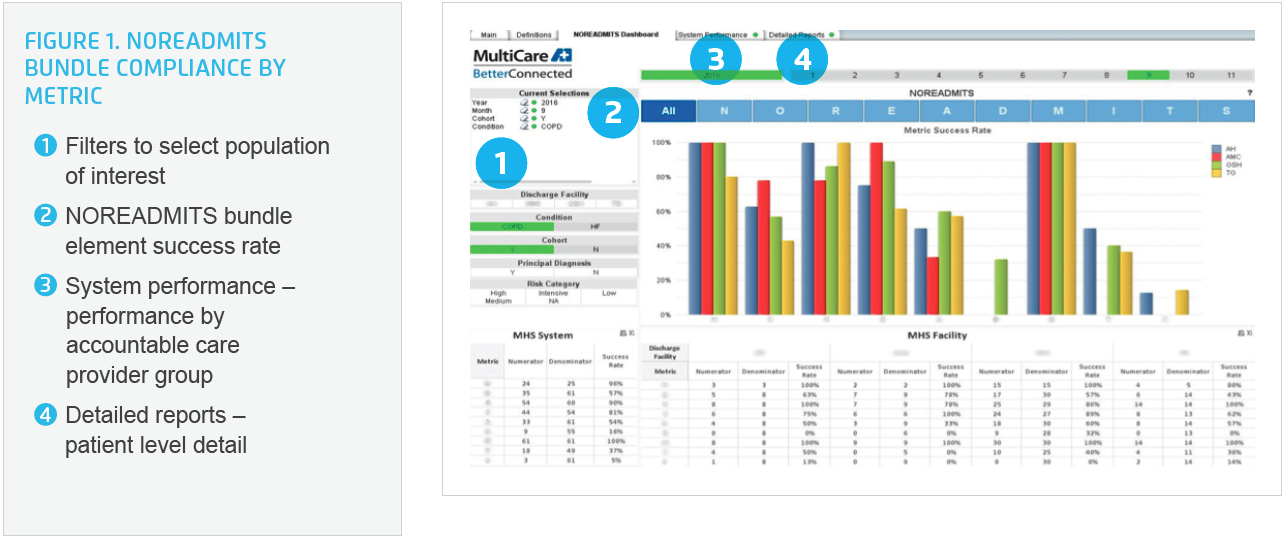
Promoting adoption of the elements of the NOREADMITS bundle, the Medicine Collaborative used the Health Catalyst Analytics Platform, including the Late-Binding™ Data Warehouse and broad suite of analytics applications, integrating performance measures for each element of the bundle into a NOREADMITS analytic application (see Figure 1).
The NOREADMITS bundle elements and associated performance metrics include:
Integrating the NOREADMITS bundle elements into the analytics application supports the Medicine Collaborative, and departmental owners, in monitoring and improving performance. The analytics application supports visualization of bundle element compliance by discharging facility and by the accountable department. Multiple views support quick, easy visualization of trends, and encourage a review of performance during monthly Medicine Collaborative team meetings. Additionally, the detailed reports tab enables users to quickly drill down into patient level detail (see Figure 1).
The analytics application eliminates the need to perform burdensome chart reviews, as patient level detail is easily accessible in the application. Users can simply open the application, access the detailed reports, quickly visualize if the patient was eligible for the bundle element, and confirm if it was provided.
The Medicine Collaborative and departmental leaders can quickly identify when performance could be improved. For example, when the analytics application revealed low order set utilization, leaders shared ordering provider performance data, allowing ordering providers to see their order set utilization and readmission rates, in comparison to their peers. When ordering providers with a lower order set utilization rate received the performance data, they subsequently increased their order set utilization rate.
Within ten months of implementing the NOREADMITS bundle, MultiCare has achieved the following results:
While already achieving impressive results, and demonstrating the effectiveness of the NOREADMITS bundle, the Medicine Collaborative is focused on increasing the number of patients who receive all elements of the bundle. It is clear these interventions make a positive impact on patient outcomes, avoiding costly readmissions.
MultiCare is actively expanding the NOREADMITS bundle to patients with pneumonia.
“I am very proud of this team. The way we have come together as a group to help these patients has been phenomenal. We’ve focused on the desired outcome, and then worked together as a cohesive team to achieve that goal.”
– Dr. Madiha Khan, Medical Director, Chief Hospitalist Sound Physicians