Population health management has emerged as a top priority due to increasing demands for flexible technology that can produce high-quality data, such as data from Health Information Exchanges (HIEs).
Healthcare industry stakeholders, including providers, payers, and public health agencies, look to prove that their collaborative efforts to align data exchange standards will scale cost, quality, and outcomes improvement measures. In turn, communities such as rural citizens and their providers will have greater access to high-quality data for better care.
HIEs represent cornerstones of data exchange if their technology, analytics, and service capabilities are modernized for today’s population health and value-based care needs. Read on to learn how HIEs can further support national connectivity efforts, local and regional value-based care initiatives, and other payment reform models.
 Download
Download

As healthcare models continue to evolve, there is growing recognition of the importance of population health management in reducing costs and promoting value-based care. To that end, Health Information Exchanges (HIEs) will play an active role in standardizing health information exchange, improving data quality, and ensuring interoperability to improve the delivery of healthcare services and patient outcomes.
HIEs must offer versatile services and flexible technical capabilities to meet the shifting demands of the industry. Accordingly, any HIE that fails to provide comprehensive data insights to assess and pinpoint improvements for patient populations or meet emerging data standards may be rendered obsolete.
However, HIEs can remain cornerstones of data exchange by modernizing their technology, analytics, and service capabilities for today’s population health and value-based care needs. Subsequently, stakeholders can utilize robust data for new use cases. Moreover, HIEs can leverage funding and resources to support national connectivity, local and regional value-based care initiatives, and payment reform models.
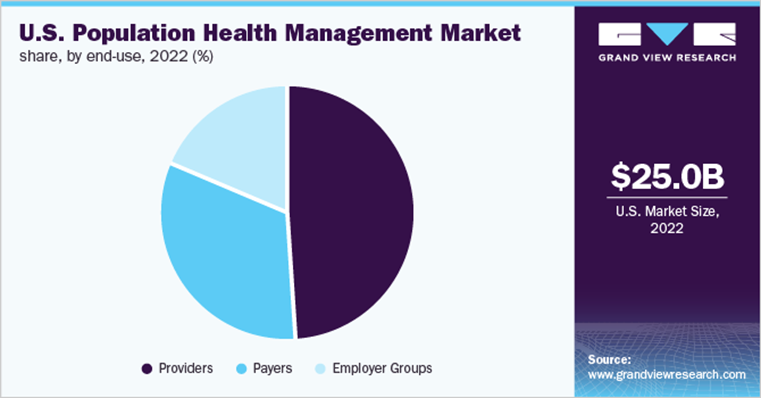
Experts valued the U.S. population health management market at $25 billion in 2022 and anticipate this figure will reach nearly $104 billion in 2030. Market share participants consist of payers, providers, and employer groups.
HIEs support the population health market and enable population health management in three ways:
Meanwhile, HIEs are grappling with numerous issues that threaten their sustainability. Sustainability approaches for HIEs should center around technology, data quality, and new partnerships. Technology modernization is crucial for ensuring HIEs can operate effectively in the long term. Prioritizing efforts to enhance data quality is equally crucial as it ensures that end users can confidently trust the shared information’s value.
HIEs are also battling financial challenges, including shifting business models and scarce revenue sources, which impact their operations and ability to provide valuable services. They also encounter issues securing funding from sources such as government grants or find that initial investments may not sufficiently cover ongoing operational costs.
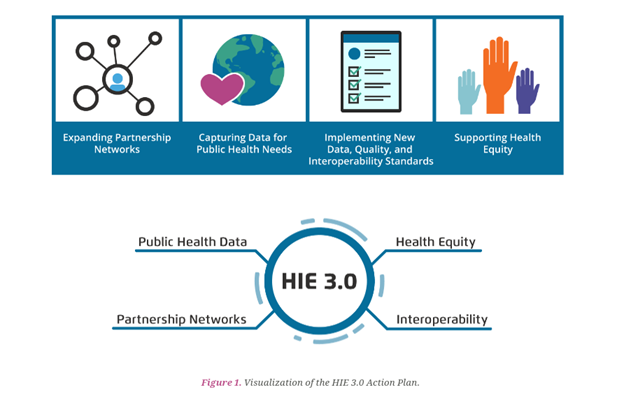
Therefore, four strategies that may improve HIE’s financial stability include:
HIEs have historically facilitated transactional data exchanges from connected sources. However, today’s healthcare landscape demands more than simple transactions. Healthcare providers and systems require more than basic information; they need sophisticated analytics to gain accurate, comprehensive, and actionable insights.
The demand for these advanced analytics is fueled by the growing focus on managing chronic diseases among various patient populations, understanding population health needs, and delivering equitable healthcare. This deeper understanding of patient demographics, social determinants of health, and risk factors allows providers to shape interventions and deliver proactive care tailored to specific groups or communities.
What’s more, by analyzing data at a granular level, organizations can uncover patterns related to access barriers, health outcomes variations among different demographics, or gaps in services. To be sure, new insights generate opportunities for targeted interventions to close these gaps and ensure everyone has equal access to high-value healthcare.
To achieve these expectations and new standards in health information exchange, many leading HIEs have selected KPI Ninja by Health Catalyst™ as their technology and services expertise partner. KPI Ninja is a cloud-native platform that aggregates, normalizes, enriches, and optimizes real-time multi-source, multi-format healthcare data. The platform encompasses the entire data lifecycle, enabling HIEs to ensure their end users receive validated and relevant data for unique use cases.
WISHIN, for example, was among the first HIEs in the U.S. to earn NCQA DAV status after adopting KPI Ninja. The partnership improved the value of the data provided to WISHIN’s healthcare participants. Their health plan participants anticipate that leveraging the validated, automated data will result in a greater than 10 percent increase in performance measures, including blood pressure and hemoglobin A1c control. Participants can also use the validated data to improve their NCQA star rating due, in part, to their alignment with a Certified Data Partner that meets certain DAV standards and supports aggregators’ data validation.
Our partnership with KPI Ninja enables us to provide more value to our clients. We’ve successfully reduced the manual chart review burden, a relief for both payers and providers.
- Joe Kachelski, CEO, WISHIN
The global healthcare data interoperability market is growing exponentially – from $2.83 billion in 2020 to $5.8 billion by 2028. The leading drivers behind this growth include an increasing emphasis on integrated patient care, a need for high-quality population health and disease management data, and national efforts to reduce healthcare expenditures. Indeed, an expanded network of partnerships fosters innovation, such as interoperable systems that seamlessly share data across organizations and provide access to larger data sets.
Therefore, health records benefit when an HIE secures an extensive network of data exchange participants. By incorporating a wider array of data, health data is more complete, empowering evidence-based practices. More comprehensive records, in turn, have more value and usability.
For instance, payer partners can help sustain HIE operations as they gain subscription-based access to broader health information. This access to validated clinical data streams can facilitate immediate enhancements to payer workflows like claims processing and Healthcare Data and Information Set (HEDIS®) reporting.
The call for better interoperability is also motivating HIEs and health information networks to actively embrace new technology frameworks and data standards such as the United States Core Data for Interoperability (USCDI) and Trusted Exchange Framework and Common Agreement (TEFCA). Participation in these networks requires customizable interoperability tools, however.
To effectively align with industry frameworks, HIEs can offer novel platform features like advanced alerting functionality, agnostic data exchange capabilities, and cutting-edge analytics, which KPI Ninja supports. As a result, HIEs that invest in a modernized cloud-agnostic solution that supports these standards are more reliable and attractive to partners and end users.
In addition to promoting health equity, leveraging HIE data has proven valuable in addressing other healthcare challenges, including supporting pandemic responses. Sharing and analyzing health data is vital to effectively address gaps in care during a public health crisis. Government payers like Medicaid also leverage HIE data for program enrollment and population health analytics, improved cost-cutting measures, care management, and quality improvement outcomes initiatives.
With the right technological backbone, HIEs can offer public health departments and federal and state agencies secure access to current and relevant medical population health data to effectively track disease surveillance, trend analysis, public health reporting, and disparities.
With a robust platform, HIEs can seamlessly shift their role from transactional data intermediaries to facilitators of population health enablement, securing their long-term sustainability.
To initiate this process, HIEs must engage a certified data partner and adopt a scalable infrastructure. By establishing these fundamentals, HIEs can consistently deliver value to various stakeholders and establish themselves as preferred data interoperability, health information exchange, and data quality partners.
Would you like to learn more about this topic? Here are three articles we suggest:
HIE 3.0: A Turning Point for HIE Business Models - Health Catalyst
HIE Adopt Data Quality Standards for Long-Term Success
NCQA Data Aggregator Validation (DAV): An ROI Analytics for HIEs