Four Effective Opioid Interventions for Healthcare Leaders
At one time, pain was undertreated, even among patients dying from cancer, and opioids were reserved to treat only the most severe pain. This gradually changed and assessing and treating pain became so important, it was named the fifth vital sign. Pharmaceutical companies began aggressively developing and selling different configurations of opioids (long acting, different routes, etc.), deeming them safe for patients.
Regulatory boards and professional organizations, such as the American Pain Society, began pushing against the undertreatment of pain. Social attitudes toward opioids changed, as did clinician prescribing patterns, as they attempted to relieve their patients’ pain.
Now, the U.S. is facing an opioid epidemic. The increase in prescribing patterns has led to the increased availability of opioids and the potential to overuse them by the patient it was prescribed for, as well as misuse by others who beg, borrow, or steal the opioids from the intended patient, the so-called “non-medical use of opioids”. The facts from the CDC about this public health problem are sobering:
- Since 1999, overdose deaths involving opioids have quadrupled, and sales of opioids have almost quadrupled.
- More than six out of every ten drug overdose deaths involve an opioid.
- On an average day, 3,900 people initiate nonmedical use of prescription opioids and 78 people die from an opioid-related overdose.
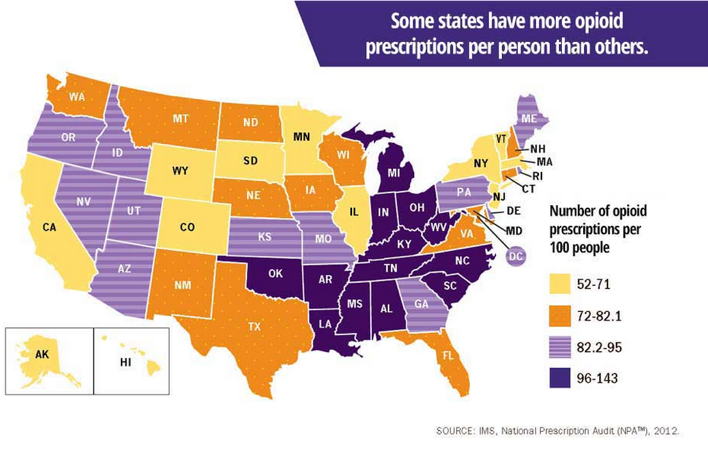
Because misuse is a multifactorial problem, multiple opioid interventions are required to combat the epidemic. But there are steps healthcare organizations and prescribers can take—both process and data driven—to decrease the risk of harm from opioids.
The Risk Patients Face When Prescribed Opioids
When I first started practicing as a registered nurse, appropriate relief of pain was a high priority. Like many others, I was trained that pain was the fifth vital sign. The minimum frequency for assessment of pain was every four hours, and we established pain goals with each patient. Pain was a frequent problem for the patients under my care because all had experienced a recent trauma. Broken bones and major wounds were common, so it was appropriate to assess the patients’ pain and appropriately attempt to relieve that pain so they could participate in their care.
It has been nearly 20 years since I provided care to her, but I still remember one patient because I was taken aback by the number of opioids prescribed and the amount I needed to administer to relieve her pain. Her opioid tolerance, and significant abuse, had started with a traumatic injury. For the initial treatment of her acute pain she received intravenous opioids. Then she was prescribed oxycontin (a medication that releases the opioid over 12 hours) for the pain and oxycodone (an immediate release opioid) for breakthrough pain. These were prescribed for her to continue at discharge, as it was anticipated that her injuries would result in continued pain.
More than a year later, when she was admitted to the hospital again, she was still taking both opioids, and had added a fentanyl patch. When the provider—who had been prescribing her 220mg of oxycontin three times daily, 60mg of oxycodone every three hours, and 100mcg fentanyl patch daily—moved out of the area, she had difficulty obtaining the number of prescriptions required for her to avoid the severe discomfort and symptoms of withdrawal she experienced without the opioids. Facing discomfort and withdrawal, she began using heroin because it was cheaper than oxycodone or fentanyl, and easier to get.
Her heroin abuse led to an infection of her hip joint and prosthesis, requiring multiple revisions. I still remember this patient, because her opioid misuse, which started with a prescription from a prescriber with good intent who was appropriately working to alleviate her severe pain, ultimately contributed to her demise. Because of her heroin use, she ended up with necrotizing fasciitis. I provided care to her over five years as she underwent numerous surgeries, painful wound debridement, numerous infections, and two above-the-knee amputations. I administered many opioids, including methadone, oxycontin, oxycodone, hydromorphone, and fentanyl. I also administered ketamine, a dissociative anesthetic that results in a trance-like state, reducing pain, and numerous medications to help ease the negative side effects of the opioids she was receiving.
Through all of this, she was aware of the risk she faced taking heroin. She had a central venous catheter, but never used that line for her heroin, telling me that it was too close to her heart and she didn’t want to die. Sadly, that is what finally happened. After years of opioid misuse and heroin abuse, she overdosed and died.
The Call for Opioid Intervention
While we healthcare providers absolutely need to do our best to alleviate pain and suffering, there is evidence that suggests non-medical opioid use is associated with heroin abuse, and that even appropriate medical use increases the risk of chronic opioid use.
A recent publication from the CDC evaluated the impact of early opioid prescribing patterns on opioid-naïve patients. The findings reveal the risks: a second opioid prescription doubles the risk for opioid use one year later; risk increases with each additional day of opioids supplied—starting with the third day— and the sharpest increase after the fifth and 31st day of therapy, a second prescription refill, 700 morphine equivalent cumulative dose, and an initial 10- or 30-day supply.
With these risks in mind, it is important that healthcare systems find a balanced approach to relieving pain and suffering, while also combating opioid misuse and overdose. While prescribers and the public await improved abuse-deterrent medications and improved non-opioid, pain-relieving treatment options, there are data-informed interventions that healthcare systems, payers, states, and individual prescribers can start today to help combat the epidemic.
Four Approaches to Confront the Opioid Epidemic
Data, analytics, and best practices can be used to identify opportunities for improvement and drive the prevention of opioid misuse and overdose.
1. Use Data and Analytics to Inform Strategies that Reduce Opioid Availability
Healthcare systems, payers, and prescribers can use data and evidence to change practices and reduce the opioid availability within the community.
Payers have access to rich data they can use for improvement. This data can be evaluated and provider-specific data shared with individual prescribers. For example, Aetna actively analyzes its claims database and intervenes if there is evidence of abuse. It notifies physicians if patients are taking more than three opioids, or if they have multiple prescriptions. This opioid oversight program reduced opioid prescriptions by 14 percent between 2010 and 2012 among 4.3 million members. In 2016, Aetna evaluated prescribing patterns and the CMO sent personal letters to nearly 1,000 prescribers—the top one percent—who refill prescriptions at a much higher rate than their peers.
There are situations in which higher amounts of opioids are clinically appropriate and should be prescribed. Sharing data creates the opportunity for prescribers to evaluate their prescribing patterns relative to their peers and adjust where appropriate.
How Allina Health Reduced Opioid Prescriptions by One Million Pills in One Year
Using data from the enterprise data warehouse, Allina Health obtained data on prescribing patterns, shared it with providers, and identified several opportunities to reduce the number of opioids prescribed.
The Allina Health team evaluated prescribing patterns in relation to national guidelines and evidence, and instituted guidelines for primary care providers, including:
- Avoiding long-acting opioids.
- Prescribing less than 20 opioid pills per prescription.
- Limiting the duration to less than five days, unless it is assessed that the injury or medical condition will last longer.
Allina Health’s efforts are already producing results, with nearly one million fewer opioid pills prescribed in the outpatient setting in just one year.
2. Adopt Prescription Drug Monitoring Programs to Prevent Misuse
States can increase the availability of Prescription Drug Monitoring Programs (PDMPs) and availability of data from other state PDMPs. Vendors need to integrate all available state data into EHRs, improving the workflow and ease of use for prescribers. State regulatory boards can help communicate evidence-based dosing guidelines, increase education opportunities and ongoing education requirements for prescribers, and should consider requiring additional prescriber education requirements beyond a specific morphine milliequivalent dose.
PDMPs help providers identify patients who might be misusing their prescription drugs. Following the implementation of statewide PDMP programs and requiring prescribers to check the PDMP prior to prescribing, New York saw a 75 percent decrease, and Tennessee a 36 percent decrease, in patients who were seeing multiple prescribers to obtain the same drugs.
3. Adopt Evidence-Based Guidelines
Washington state implemented evidence-based dosing guidelines, including a dosing threshold trigger for consultation with pain specialists, criteria to be considered a pain specialist, elements for patient evaluation, periodic review of the patient’s treatment plan, exemptions for special circumstances, and continuing education requirements. The state also obtained additional funding for the PDMP. These changes are believed to have contributed to a 27 percent reduction in opioid deaths between 2008 and 2012.
Primary care providers account for approximately 50 percent of all dispensed prescription opioids. Individual prescribers, particularly those within primary care, should be familiar with, and use, the most recent evidence when making decisions regarding the treatment of chronic pain. The CDC Guideline for Prescribing Opioids for Chronic Pain can help providers make informed decisions about pain treatment for patients 18 and older in the primary care setting.
The ED is the largest ambulatory source for opioids. Prescribers within the ED can make use of the opioid prescribing resources made available by the American College of Emergency Physicians, and should limit prescribing opioids for chronic pain to only the immediate treatment of an acute exacerbation of uncontrolled pain.
When prescribing opioids, prescribers need to check the PDMP, use the lowest possible effective dose, and start with immediate release opioids rather than long-acting opioids. The quantity prescribed should align with the expected duration of the pain.
Dosages at or above 50 morphine milliequivalent doses are associated with an increased risk for overdose. Prescribers should consider offering a prescription for naloxone (the medication used to reverse opioid overdose) and provide education to the patient and their support system about how naloxone works.
4. Consider Promising State Strategies for Dealing with Prescription Opioid Overdose
States can use data from PDMPs, Medicaid, workers’ compensation programs, and state-run health plans to identify pain clinics that may be prescribing opioids in ways that are risky to patients, so they can address inappropriate prescribing. Many states also need to increase access to substance abuse treatment services and medication-assisted treatment services.
Healthcare providers and states can support layperson administration of naloxone and can encourage bystanders to be good Samaritans and summon emergency response for someone who has overdosed. These good Samaritans should be encouraged to contact emergency response without fear of arrest or other negative consequences. As of June 2016, all but three states had passed legislation to increase layperson access to naloxone. Good Samaritan laws are not yet widespread.
Increases in the availability of naloxone, Good Samaritan laws, and education for the public regarding the safety and utility of naloxone can reduce the number of overdoses. Between 1996, when naloxone was first made available to laypersons, and June of 2014, more than 150,000 naloxone kits were distributed, and 26,463 overdoses were reversed.
The Opioid Epidemic is a Public Health Problem with a Treatment
It is critical that healthcare providers continue to work to alleviate pain and suffering. At the same time, it is increasingly important that each of us involved in the delivery of healthcare—healthcare systems, payers, and prescribers—use data, analytics, and evidence-based practices to inform prescribing patterns, identify potential misuse, and change practices to minimize opioid misuse and overdose. Patients, like the woman I still think about from so many years ago, are relying on us to relieve their pain without inadvertently increasing the risk that they will be harmed.
Additional Reading
Would you like to learn more about this topic? Here are some articles we suggest:
- Combatting Opioid Abuse with Data-Driven Prescription Reduction (Success Story)
- How to Use Data to Improve Patient Safety
PowerPoint Slides
Would you like to use or share these concepts? Download this presentation highlighting the key main points.
Click Here to Download the Slides
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.


