Orlando Health recognized the importance of effective data integration for strategic decision-making as its business needs evolved. The organization opted for a late-binding data warehouse to improve flexibility and access to critical data, enabling quicker acquisition and linking of disparate healthcare data for better clinical and business insights.
Effective data integration enables high value through more strategic, data-driven decision-making, while faster data acquisition feeds and speeds up the process. Orlando Health, one of Florida’s most comprehensive private, not-for-profit healthcare networks, recognized the need for effective data integration to successfully manage to the organization’s changing business needs. The health system needed the ability to rapidly acquire and link disparate healthcare data sources in various ways in order to answer clinical and business questions.
Leaders at Orlando Health needed a data warehouse that better met their needs. They determined that switching from an early binding data process to a late-binding process would provide greater flexibility and expand their access to critical data, with shorter data acquisition times.
Data integration enables business value when it provides information that is as close to real-time as possible, improves data quality, and is easily linked and correlated across disparate systems.1 With effective data integration, organizations can complete high-value business activities such as risk modeling, benchmarking, and event correlation, which lead to better, more data-driven decisions.
This can be a key differentiator among healthcare systems. Those that can make strategic, data-driven decisions are more likely to be successful in identifying shifting trends that will affect their organization, as well as to quickly respond to changing regulations, measure definitions, and treatment options.
Orlando Health is one of Florida’s most comprehensive private, not-for-profit healthcare networks consisting of eight hospitals and 50 clinics. This award-winning health system recognized the need for more strategic, data-based decision-making, and realized that this would require rapid data acquisition and nimble data integration.
With effective data integration, healthcare organizations can rapidly acquire and link multiple data sources in various ways, depending on the clinical or business questions being posed. The health system’s existing EDW had two restrictions that made it difficult to access and combine data sources quickly in a way that could be applied to different situations and business use cases.
First, the data acquisition process of adding new data elements and data sources was too cumbersome and labor intensive. Every time new data sources were required because of changing regulations, treatment protocols, or quality metric definitions, the data needed to be re-mapped. In fact, mapping and integrating new data sources could take several months or over a year. This lengthy process meant that leaders at Orlando Health often couldn’t access the data when they need it to support business decisions or quality improvement efforts. Second, the old EDW had rigid data-mapping requirements. These requirements meant that leaders at Orlando Health had to try to model the perfect database from the outset, determining in advance every possible business rule and vocabulary set that would be needed for years to come. This practice, called early binding, is a time-consuming and expensive undertaking for any business, but even more so in healthcare—an industry where business rules and vocabularies change rapidly, as do the use cases for linking data across source systems to solve problems. With early binding EDWs, mappings must be redone again and again as data models shift. In addition to those major constraints, they were limited by a less than optimal master data management process. Master data management is the process of linking identity and reference data across multiple IT systems into a single, consistent point of reference that facilitates the accurate identification and linking of related data.
Orlando Health decided to transition from their current EDW to Health Catalyst’s Analytics Platform built using the Late-Binding™ Data Warehouse architecture. Their reasons for choosing the late-binding technology were to:
While the old EDW’s data model was the classic extract-transform-load process, the new system’s late-binding model moves transformation of data to the end, which dramatically alters and improves the healthcare data acquisition process. With the new technology, team members could acquire, access, and relate data elements for multiple purposes without constantly rebuilding data tables or reacquiring source data (see Figure 1). That flexibility also makes it easier to adapt to changing and variable reporting requirements.
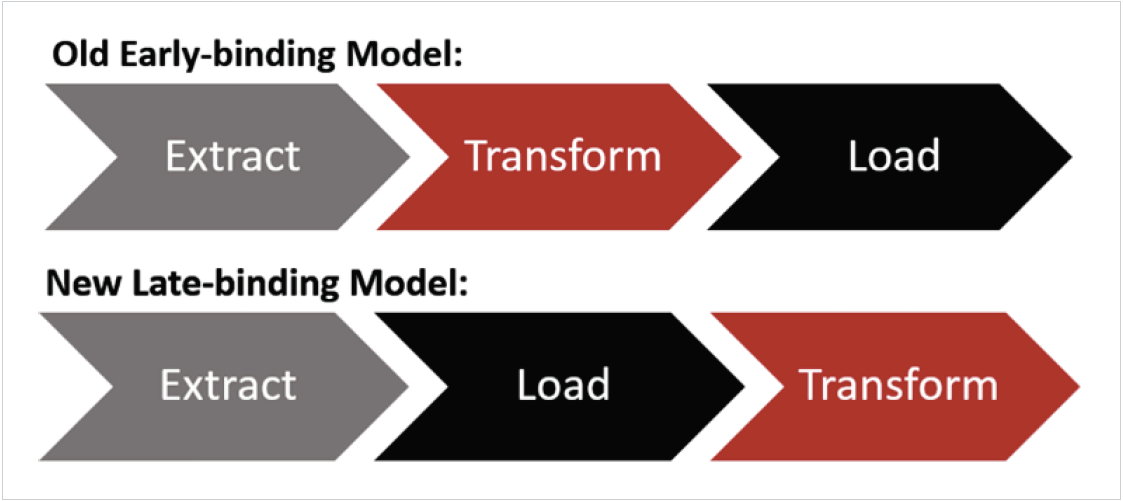
Moving the “transform” step to the end has multiple advantages for healthcare organizations. First, eliminating data mapping (the “transform” phase) as a pre-requisite to data acquisition significantly shortens the time needed for data acquisition (the time to complete the “load” phase). Next, there is an almost unlimited increase in the amount of data that can be loaded and made available in the EDW. The new architecture accepts all data elements from a source without having to build a specifically mapped place for each element. This capability simplifies the addition of new data sources and the expansion of available data elements within previous sources. This approach allows healthcare providers to perform timely, relevant advanced analytics and leverage the analysis to quickly answer questions or apply it to new use cases. These processes, which were previously impossible to perform, are an integral part of data acquisition and key to simplifying data mapping.
While leaders at Orlando Health understood the clear benefits of the new EDW, they expected the process of transitioning data sources to the new platform to be a long, uphill battle. They were pleasantly surprised to discover that the addition of the expertise provided by the new source mart team, coupled with the improved efficiency of the overall process, allowed new data sources to be entered quickly with fewer FTEs and a higher degree of data integrity. Having a team member on the source mart team with in-depth knowledge of both the legacy system and the new system was also helpful in ensuring a smooth transition. Leaders and team members were pleased to achieve a much shorter time to value than they had anticipated.
Since Orlando Health leaders pride themselves on being good stewards of resources, they wanted to keep track of both improvements and degradation in time and efficiency for each step of the transition to the new EDW. The organization is currently in the extract and load phase for multiple sources. There were two source systems, infection control and the encounter billing summary system, for which there was performance data to provide a good comparison of data acquisition times between the old and new EDWs, and which also offered an opportunity to see the potential impact of improved data access on internal processes.
Data acquisition and more information for Infection Control
During the implementation of the old EDW, only limited data from the organization’s infection control system had been loaded into the platform. Even with that smaller data set, it took almost 25 work weeks and one FTE to complete. In contrast, loading all the data from the infection control system into the new EDW took less than 14 work weeks, with only a portion of an FTE.
Effectively managing infection prevention (IP) programs in a hospital system is a complex process which requires access to multiple streams of data, and the ability to respond to multiple different reporting and clinical needs for infection information. Orlando Health’s capability to manage infection prevention data was greatly enhanced by the larger data set pulled from the infection control system and the greater flexibility provided by the new EDW. For example, the CDC’s National Healthcare Safety Network (NHSN) defines standard surveillance methods and metrics for monitoring infection that must be strictly adhered to and publicly reported. Changes in surveillance models and metric definitions occur fairly often. With the greater flexibility provided by the new EDW for adding new data elements and modifying analysis, Orlando Health will be able to rapidly adapt to the changing definitions and requirements for surveillance and reporting of infections.
With the full data set from the source system in the new EDW, team members will now be able to track patient location. Knowing the location of patients that acquire infections is essential to managing regulatory reporting requirements, and recognizing, responding, and intervening when there are patterns of infection. In the old platform, with the limited data available, it was impossible to track patient location, which severely limited the utility of the information that was available, especially when it came to intervening with patients to improve clinical outcomes.
Data acquisition and improvement for the Encounter Billing Summary System
Incomplete data and strict mapping requirements in the old EDW created challenges for Orlando Health’s finance and revenue cycle departments, which meant that they were not using the EDW for reporting. Loading limited data from the organization’s encounter billing summary system into the old EDW took almost 60 work weeks and more than one FTE. In contrast, it took fewer than 10 work weeks with a portion of an FTE to load all the data elements from its encounter billing summary system into the new EDW. In addition to this more comprehensive data, the new EDW offers the flexible data-mapping requirements that they need to support data-driven decision making.
Orlando Health’s billing system is architected around a hospital model that tracks all charges for a specific timeframe to a single visit or account number. A visit can be a clinic appointment or a hospital stay. It can vary in length and in the number and type of charges that are accumulated for that visit type. This structure, combined with the old EDW’s rigid data-mapping requirements, made it difficult, if not impossible, to differentiate among multiple physicians seeing the same patient during a single visit. For example, leaders at Orlando Health wanted to track heart failure patients. However, the billing system, which includes all the diagnosis and medical procedure codes commonly used to identify these patients, could only track patients to billing areas, which provided limited clinical utility. The new platform will make it possible to look at billing data along with clinical data from multiple systems. With the additional advantages provided by standardized master data management, access to the desired information will be much easier, and will open the way to greater clinical insight and potential intervention.
Although only at the second step in a three-step process to set up the new EDW, leaders at Orlando Health have seen efficiencies in data acquisition that they believe are a precursor to even greater improvements as they move into data transformation.
For data acquisition times for source data, Orlando Health achieved the following efficiencies:
Orlando Health also achieved efficiencies in adding new data elements or making other enhancements such as adding columns or changing data source pulls for reports:
“In the old system, we were unable to track patient location, which is a very important data point for us. We can easily track it in the new system—and that’s just one example of a huge win for the team. We expect many more wins to come.”
– Debbie Sherwin, Project Manager
Team members at Orlando Health are initially loading 10 systems that they identified as priorities. They were not successful in loading all 10 of these priority systems into the old EDW but will be able to do so in the new platform. In fact, there are more than 200 information systems in the hospital that potentially could be integrated into the late-binding data warehouse in the future. The transformation of the data, coupled with the improved data access and visualization that is slated to occur later in the year, will be a great advantage to the organization. They have already generated excitement among the stakeholders simply by sharing the new data model and the improvements in data acquisition. Users see the potential for more flexible and complete access to data, and are looking forward to getting the expanded information to guide decisions and monitor progress.




