Emergency departments (ED) provide care for 145 million patients a year. Improving throughput times is a top priority for hospitals to reduce overcrowding, long wait times, and safety concerns. To improve ED throughput, Orlando Regional Medical Center assembled an improvement team to analyze the problem, utilizing data analytics to help identify workflow changes designed to improve ED throughput and care delivery.
Emergency departments (ED) provide care for a staggering 145 million patients a year, resulting in hospital admissions for 8.9 percent of patients. Because of the high cost associated with ED visits, improving throughput times remains a top priority for hospitals. Overcrowding and long wait times in an emergency department occur as visit volume rises, leading to potential safety events and dissatisfaction with care.
In its emergency department, Orlando Regional Medical Center (ORMC) experienced increasing patient volumes that did not align with the resources it had available to provide quality care. As a result, patients were waiting in the ED longer than desired, and throughput times were not meeting internal goals or industry standards. After assembling an improvement team to analyze the problem, data analytics and staff feedback identified a series of workflow changes—including improved staffing throughout the entire hospital—that were designed to improve ED throughput and improve care delivery.
In the U.S., EDs provide care for over 145 million people annually, with 8.9 percent of ED visits resulting in hospital admission.1 As a result, overcrowding and long wait times often occur with increases in ED visit volume, leading to potential safety events and dissatisfaction with care.2
Like many high population areas, Orlando Health experiences a high volume of ED visits. Orlando Health is one of Florida’s most comprehensive private, not-for-profit healthcare networks, and is a healthcare leader for nearly two million Central Florida residents and 10,000 international visitors annually.
ORMC is Orlando Health’s flagship hospital and Central Florida’s only Level One Trauma Center; it is also a designated Stroke and Cardiac Center. ORMC provides care to over 100,000 patient visits annually and is equipped to handle any major or minor emergency. Improved patient experience and throughput time in the ED is a major priority for ORMC, because of the opportunity improvements present for better outcomes and cost savings.
As with many EDs across the nation, ORMC experienced increasing patient volumes while having a finite amount of resources to provide care. Subsequently, patients were waiting in the ED longer than desired, throughput times were not meeting internal goals or industry standards, and a number of patients were leaving without being seen.
Orlando Health has consistently sought to use data to support its improvement efforts, leveraging lean concepts to improve outcomes and reduce cost, yet limited access to actionable data hindered targeted improvement efforts. ORMC was aware of the impact of inefficiencies in internal processes for patient flow within the ED from the time of arrival until seen by a qualified provider. However, without insight into patient volume, arrival times, and throughput metrics, improvement efforts were often ineffective.
Leadership recognized that factors outside of the ED impacted throughput, including diagnostic testing turnaround times, room turnaround, patient transportation, and inpatient bed availability. A lack of actionable data negatively impacted collaboration with other departments, limiting the ability to develop improvement plans. ORMC understood that to impact ED throughput, it needed a data-driven collaborative culture and hospital-wide engagement.
ORMC convened an interdisciplinary improvement team charged with developing a hospital-wide solution for improving ED throughput. The improvement team includes physicians and nurses from the ED, lean concept improvement specialists, data analysts, and representatives from radiology, laboratory, and environmental services.
Orlando Health leverages the Health Catalyst® Data Operating System (DOS™) and a robust suite of analytics applications, including the Department Explorer: Emergency Services analytics accelerator, to provide sophisticated analytics, gaining insight into ED throughput data. The analytics accelerator provides near realtime visibility into performance. The visualizations include ED data, LWBS rates, time from arrival to provider, time from admission order to arrival to an inpatient bed, and time from discharge order to departure from the ED. Patient volume and arrival trends can be reviewed and compared by day, week, month, or year (see Figure 1).
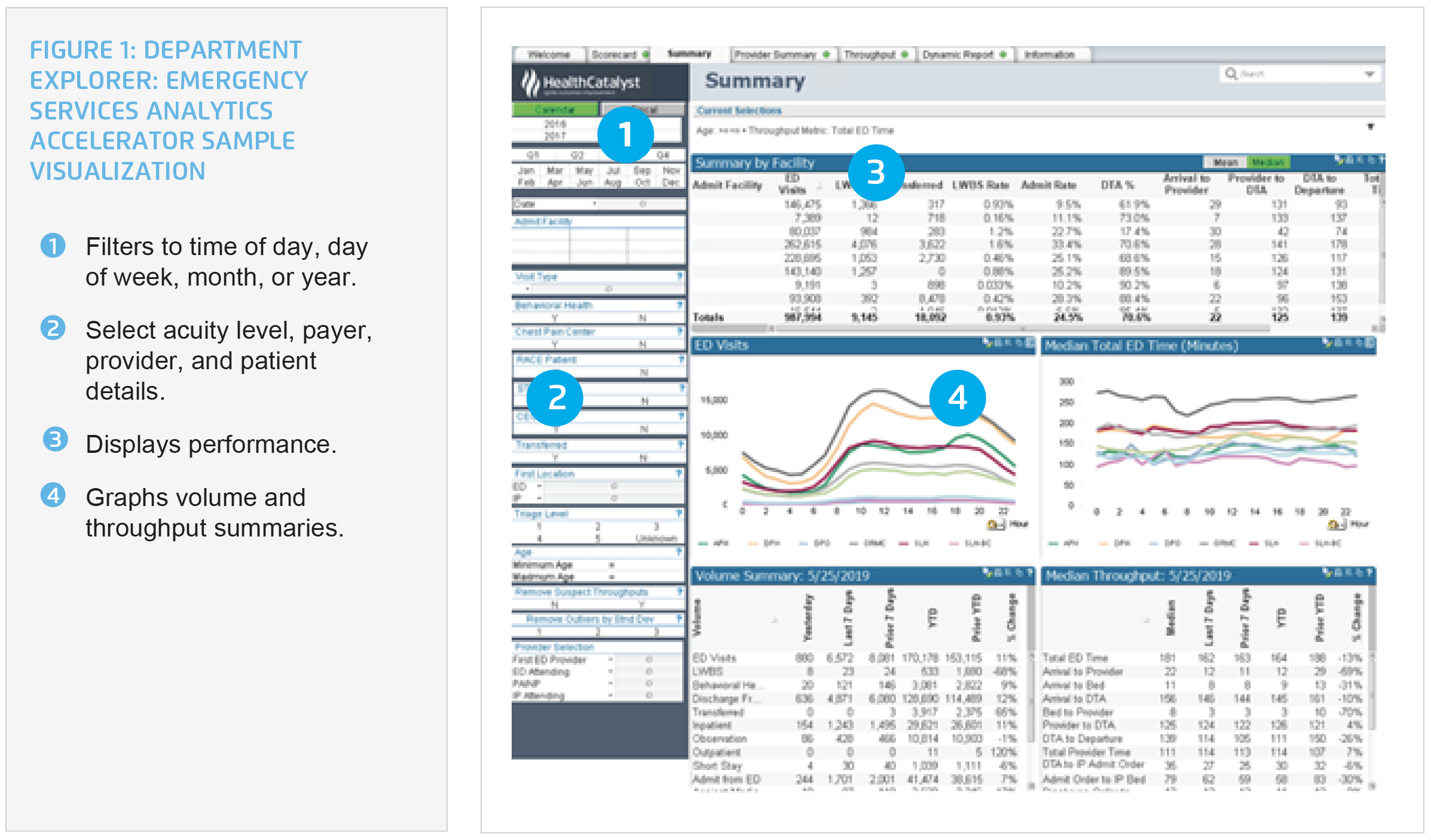
ORMC used its new insights from the analytics accelerator to implement strategies across the continuum of care to improve ED throughput. In an effort to positively impact throughput time, ORMC implemented several changes.
ORMC turned to its ED to identify opportunities for improvement from the source. Looking to its data for evidence and factoring in staff feedback, the following changes were made:
ORMC implemented a series of improvement changes throughout the hospital that were determined to have an effect on ED throughput and operations, such as:
ORMC understands the importance of team member engagement for an initiative to succeed and the use of data to monitor performance. Leadership uses the analytics accelerator as a daily scorecard, fostering ownership of key performance indicators (see Figure 2). The vice president of operations leads a weekly operations huddle with stakeholders to review key performance metrics impacting ED throughput, including:
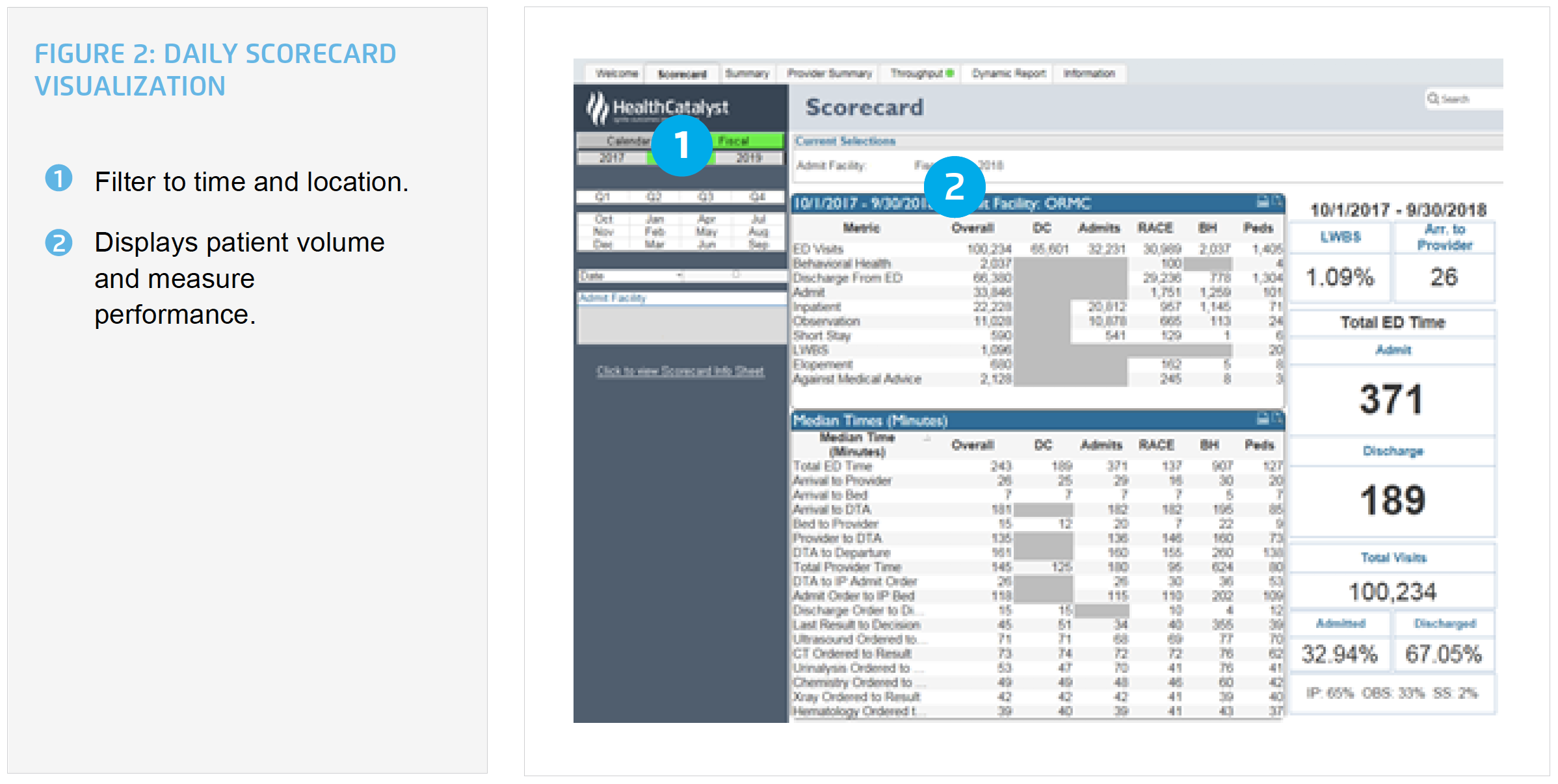
Using this collaborative, data-driven approach ORMC has achieved substantial improvements in ED throughput, including:
“We knew that we needed to engage hospital leaders to impact ED throughput to achieve our goal of providing the right care in the right place to improve the overall patient experience and quality of care.”
– Louise Philp, MSHA, BSN, RN, CCRN-K, NEA-BC Administrator Patient Care Trauma, Neuroscience, and Emergency Services Orlando Regional Medical Center
ORMC has established a culture of shared ownership for ED throughput. ORMC plans to further improve throughput by refining multidisciplinary rounds and improving case management for its complex patients.




