Health systems and hospitals need strategies to prepare for the increased demand for clinical and non-clinical staff as generations age, chronic conditions become more prevalent, and the industry shifts towards innovative employment and care models that require advanced technology and expert partners to manage operational costs and varying patient volumes.
 Download
Download

Editor’s Note: This article is based on a webinar entitled “Healthcare Labor Challenge – Why Is It Happening and What Can You Do About It?” featuring Dan Unger, Senior Vice President and General Manager of the Improvement Applications Business Unit.
Healthcare cost management and workforce improvement complexities are the biggest, most pressing challenges of our time. Rising labor costs and workforce shortages create turmoil for healthcare budgets, finances, and clinical priorities. Ultimately, compromised workforce stability results in unwarranted care variation, limited outcomes improvement, employee burnout, and reduced patient access to critical treatment services.
As we look ahead to 2024, healthcare staffing challenges will only intensify. These issues are not isolated to clinical positions. Indeed, hospitals are struggling with staffing shortages and wage increases in support staff and non-clinical roles equally as much. Health systems urgently need strategies to confront these hurdles head-on to maintain adequate staffing levels and support their infrastructure as employees exit the profession at record rates.
To address the matter, hospitals and other medical institutions must focus on preserving funds for clinical staff as much as possible, and this can be accomplished by leveraging partnerships to guarantee savings in non-clinical areas.
As discussed in the recent Health Catalyst webinar, Healthcare’s Labor Challenge-Why Is it Happening and What Can You Do About It? capitalizing on opportunities to reverse the economic impact of today’s workforce improvement challenges is essential for two reasons:
Labor analysts predict rapid growth for the healthcare industry, making it the fastest-growing sector. This projection comes as no surprise as the demand for healthcare services continues to rise due to an aging population and advances in medical technology. In addition, recent events like the COVID-19 pandemic further emphasized the critical importance of having a well-equipped healthcare system.
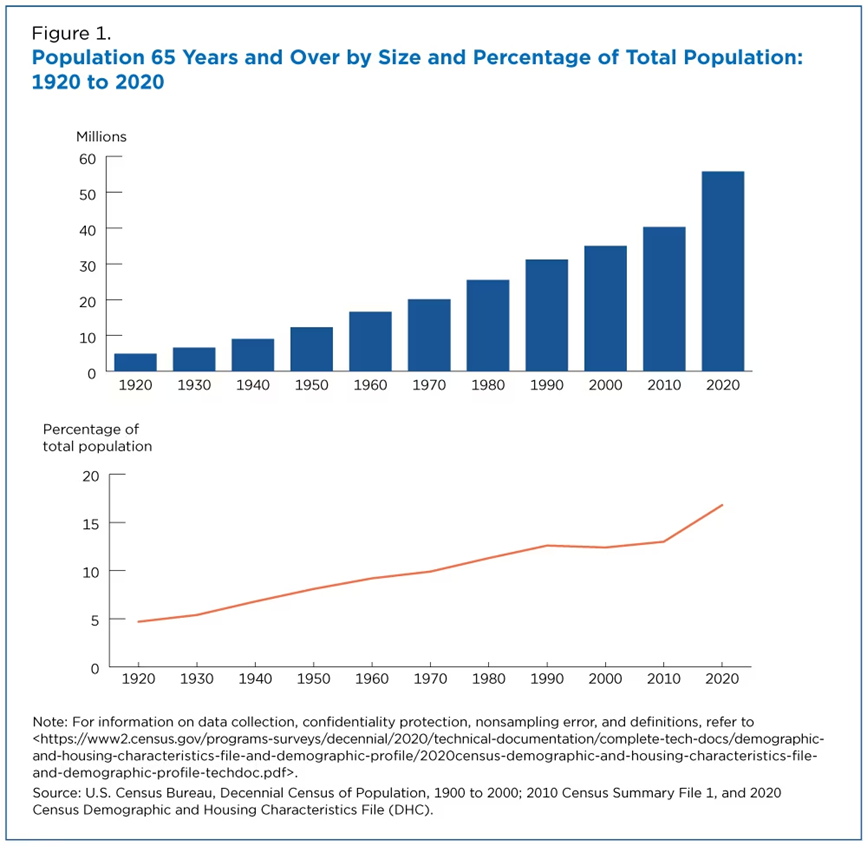
The U.S. Bureau of Labor and Statistics (BLS) projects that approximately 45 percent of all the anticipated job gains from 2022 to 2032 will come from healthcare, translating to an estimated 2.1 million jobs.
With the anticipated surge in vacant positions, there will be substantial demand for clinicians, nurse practitioners, occupational therapists, home health and personal care aides, and health services managers.
Another aspect of this growth can be seen through technological advancements within the industry. The integration of digital health solutions, telemedicine platforms, and augmented intelligence technologies is transforming how healthcare services are delivered.
As a result, job opportunities within IT departments or roles specializing in data analysis and data science are expected to surge alongside traditional clinical positions.
The healthcare industry's workforce improvement interference can be attributed to three notable setbacks: a global workforce crisis, employee burnout, and unbalanced labor supply and demand, which are affecting various areas within organizations, including workplace culture and long-term financial viability.
Research shows a greater need for registered nurses (RNs) and clinicians in the next decade to staff quality initiatives, invest in clinical programs that improve disease management, and meet seasonal fluctuations in patient volume.
Indeed, startling projections from the BLS estimate that American healthcare organizations must fill more than 203,000 open nursing positions annually until 2031.
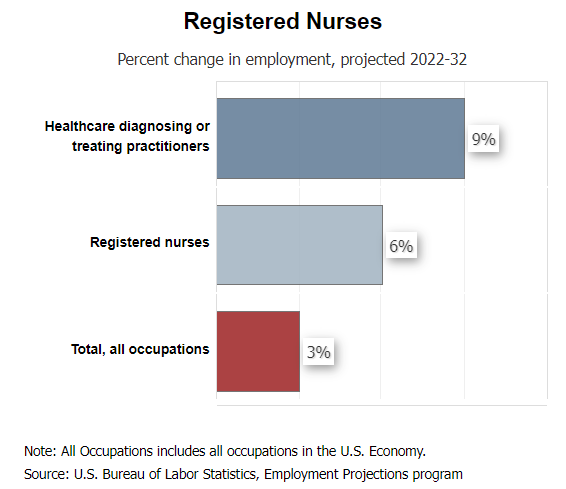
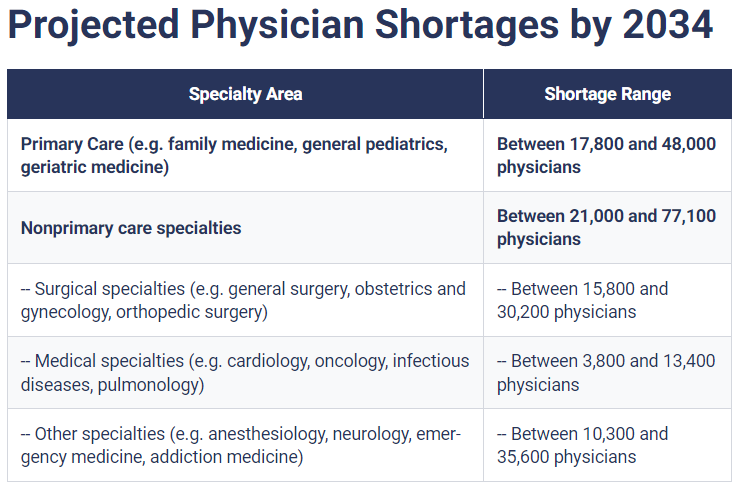
In addition to RNs, there are significant projected shortages of physicians in primary and specialty care along with allied health and behavioral healthcare providers. This predicted shortfall will likely adversely impact marginalized communities, including rural and urban regions.
Within the next decade, over 40 percent of currently practicing physicians in the U.S. will reach the age of 65 years or older, according to a report by the AAMC (Association of American Medical Colleges).
With a sizable portion of doctors approaching retirement, there is an imminent risk of losing their valuable expertise and leaving a void that may be challenging to fill. What’s more, these workforce gaps and retention concerns represent immediate concerns for health systems, as employees could incur substantial costs associated with employee turnover.
Health systems can effectively adapt to changing labor market conditions and patient volumes by making short-term enhancements to their labor and workforce strategies, including leveraging data for workforce planning and resource allocation, which can lead to long-term success.
Longer-term improvements in healthcare are essential for addressing the systemic issues underpinning today’s workforce improvement issues. It is a complex and ongoing effort that requires collaboration from healthcare providers, policymakers, the community, and other partners.
Meanwhile, instituting policies in the near term for increasing training and education for medical professionals, as well as investment in the infrastructure to support this essential group, could attract people to the healthcare industry and help fill clinical vacancies in the future.
Healthcare practitioners and support staff are also evaluating factors such as compensation, benefits, predictable work hours, healthy work-life balance, and access to innovative technological tools for patient care or productivity to influence their employment decisions.
Health systems can also migrate to a more reliable data and analytics platform for evidence-based decision-making. With the unpredictable nature of patient volumes, it is essential to have access to data-driven insights that can accurately predict trends.
By investing in culture, technology, and operational changes, healthcare organizations can emerge as a destination workplace for practitioners.
Veteran employees within an organization bring a wealth of knowledge and competence, including an existing rapport with patients. These experienced professionals can help new recruits. Therefore, providing an environment that values and supports their contributions is important.
There are numerous ways hospitals can maximize seasoned team members for outcomes improvement.
Healthcare system finances are undoubtedly facing a devastating blow, in part due to staffing shortages. Many hospitals and healthcare facilities need help meeting the demand for skilled nurses, doctors, and technicians, leading to increased patient-to-staff ratios and compromised quality of care.
The consequences of these challenges are detrimental on multiple levels:
Addressing these obstacles requires innovative solutions beyond traditional retention and recruitment strategies to achieve long-term financial success. Adopting more robust data and analytics solutions along with labor and cost management systems while prioritizing employee well-being holds immense potential for transforming hospitals into premier workplaces and earning them a reputation for world-class patient care.
Would you like to learn more about this topic? We suggest these three articles:
A Healthcare Labor Shortage Action Plan
Labor Shortage: Why You Need the Right Labor Management Partner Now
A Healthcare Worker Shortage Action Plan: Short-Term and Long-Term Strategy