Blood Conservation Program Yields Millions of Dollars in Savings

- $3.2M decrease in annual blood product acquisition costs since 2011
- 30,283 units saved annually
- 111 units of red cells saved per 1000 inpatient admissions
Every three seconds, someone in the United States will need a blood transfusion, which adds up to nearly 17 million blood components transfused annually. Yet, evidence shows that up to 60 percent of red cell transfusions may not be necessary. In 2011, Allina Health, a healthcare delivery system that serves Minnesota and western Wisconsin, had a wide variation in transfusion practices throughout the system and a transfusion rate that was 25 percent above national benchmarks. In an effort to improve outcomes of high-risk transfusions, Allina Health turned to its data to develop an evidence-based blood conservation program aimed at reducing costs and saving valuable blood resources.
A CASE FOR POLICING BLOOD USAGE
Blood transfusions are a common medical intervention, with nearly 17 million blood components transfused in the U.S. annually—but, they are not without risk.1 Recent evidence indicates that a blood transfusion places patients at risk for immediate and long-term adverse outcomes, including myocardial infarction, stroke, renal failure, infection, and malignancy. Receiving a blood transfusion also increases a patient’s risk of death. Further, patients who receive blood transfusions during cardiac procedures or orthopedic surgeries may be at greater risk for adverse outcomes.2,3
Allina Health, an integrated healthcare delivery system, is dedicated to the prevention and treatment of illness and enhancing the greater health of individuals, families, and communities throughout Minnesota and western Wisconsin. Despite the availability evidence- based guidelines for blood conservation, physicians have been slow to embrace them.
Blood transfusions are considered a high-risk procedure with substantial associated costs, with red cells alone costing an estimated $7 billion annually. However, evidence indicates that up to 60 percent of red cell transfusions may not be necessary. Additionally, there is wide variation in transfusion practices nationwide, unexplained by patient characteristics.4 Allina Health looked to the development of a blood conservation program as a means to improve outcomes and reduce costs associated with the use of blood products.
HIGH DEMAND FOR BLOOD PRODUCTS FUELS CONSERVATION
With 12 hospitals, more than 100,000 inpatient hospital admissions annually, 1.5 million hospital outpatient admissions, 343,000 emergency care visits, and more than 90,000 inpatient and outpatient surgical procedures performed annually, Allina Health uses a lot of blood products, Aware of this, senior clinical leaders at Allina Health began discussions in 2010 on how to determine necessity for, and reduce the unwarranted use of, blood products across the system.
Wanting to better understand the opportunity for improvement, Allina Health obtained a blood product utilization review by an external consult. As a result of the review, Allina Health discovered its transfusion rate was higher than supported by the evidence and there was wide variation in transfusion practices across the system. In total, blood transfusion rates at Allina Health were coming in 25 percent higher than national benchmarks.
The external benchmarking was useful in highlighting opportunities for improvement in utilization. However, the monthly reports Allina Health received did not have enough detail to be useful in targeting meaningful outcomes improvement. Allina Health needed a strategic work plan that would increase adherence to evidence-based guidelines, thus making better use of limited, costly blood resources in an effort to ensure patients were receiving the best possible care.
BLOOD CONSERVATION PROGRAM ENACTED SYSTEMWIDE
Due to Allina Health’s systemwide EHR with shared electronic transfusion order sets, the decision was made to implement changes systemwide, rather than hospital by hospital. To ensure appropriate utilization of limited, costly blood resources, and ensure it was providing patients with the best possible care, Allina Health launched a blood conservation program, establishing a transfusion care council to provide governance over the improvement process.
With the understanding that clinical expertise was needed to make lasting improvements, Allina Health identified key stakeholders for the transfusion care council, including physician representatives from pathology, cardiovascular surgery, and anesthesia. Representatives from nursing were also identified to champion the improvement efforts and promote buy-in.
Allina Health relies on the Health Catalyst® Analytics Platform, including the Late-Binding™ Data Warehouse and broad suite of analytics applications, for its data and analytics. To make meaningful outcomes improvements, Allina Health needed detailed data regarding blood product utilization, beyond what the initial benchmarking could provide. Allina Health leveraged its analytics platform to create a comprehensive, interactive transfusion application with more robust metrics and details to support ongoing outcomes improvement. The interactive transfusion application enabled Allina Health to conduct comprehensive evaluation and monitoring of blood product utilization (see Figure 1).
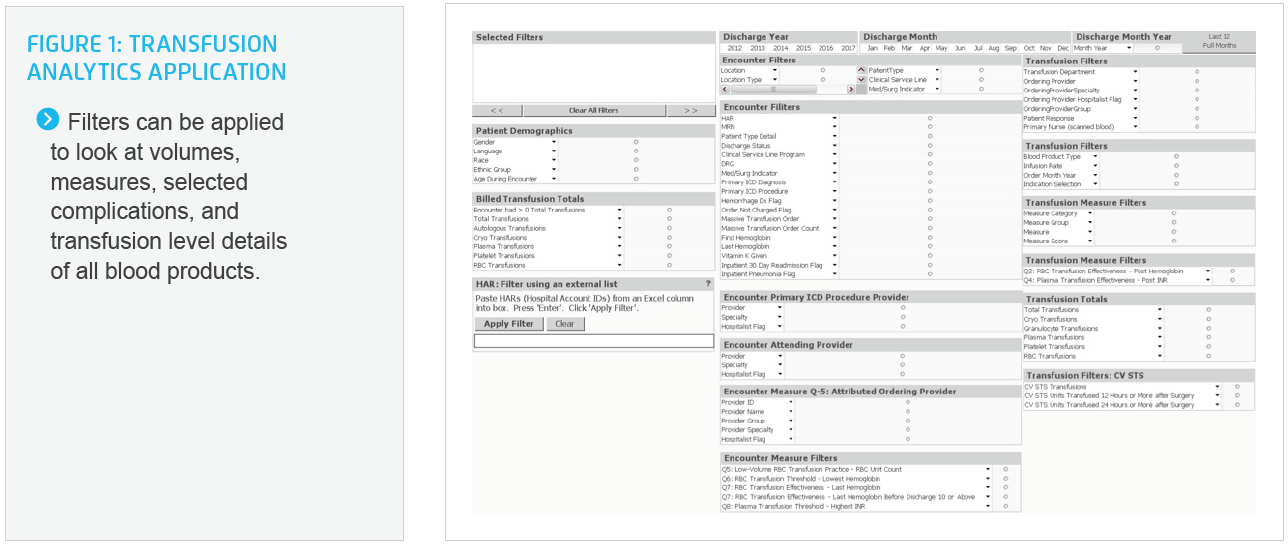
The interactive transfusion application provides visualization into blood product utilization, including transfused products, ordering provider, indications for transfusion—which includes frequency and timing of transfusions, number units transfused, effectiveness of transfusion, and more. The data is viewable by hospital, unit, or patient, and is inclusive of the patient age, diagnosis, and any complications. Additionally, the application provides insight into compliance with regulatory requirements for blood product administration.
Through the use of the analytics application, Allina Health was able to complete a detailed review of blood product utilization. Armed with meaningful, actionable data, the transfusion care council better understood the opportunity for improvement, and began work to ensure complete adoption of The Society of Thoracic Surgeons blood conservation guidelines. Several high-impact improvements were implemented systemwide:
- Reduced the systemwide transfusion order set default unit from two units to one.
- Included tools and information in the EHR order sets, such as recent lab values and patient vital signs, that can be used to enhance decision making during order entry.
- Added requirement for an in-person evaluation of the patient’s condition, basing the decision to transfuse on patient symptoms in addition to lab results.
- Updated cardiac bypass protocols to use the patient’s blood to prime the heart-lung machine, as opposed to using donated blood.
- Implemented auto-transfusion, a process where patients receive their own blood which is collected from surgical sites is filtered for re-infusion, for surgical cardiac and orthopedic patients.
- Added a device to invasive monitoring lines to reduce the volume of blood obtained for lab draws.
The new blood transfusion guidelines are vastly different from what many medical and nursing professionals learn during training. As such, Allina Health understood that education would be a key driver for success. Comprehensive workshops were developed for medical and nursing staff. Learning videos were created to support the transfusion improvements and to provide ongoing education across the integrated system. Additionally, quality scorecards support ongoing systemwide evaluation of performance in comparison to internal and national benchmarks (see Figures 2 and 3).
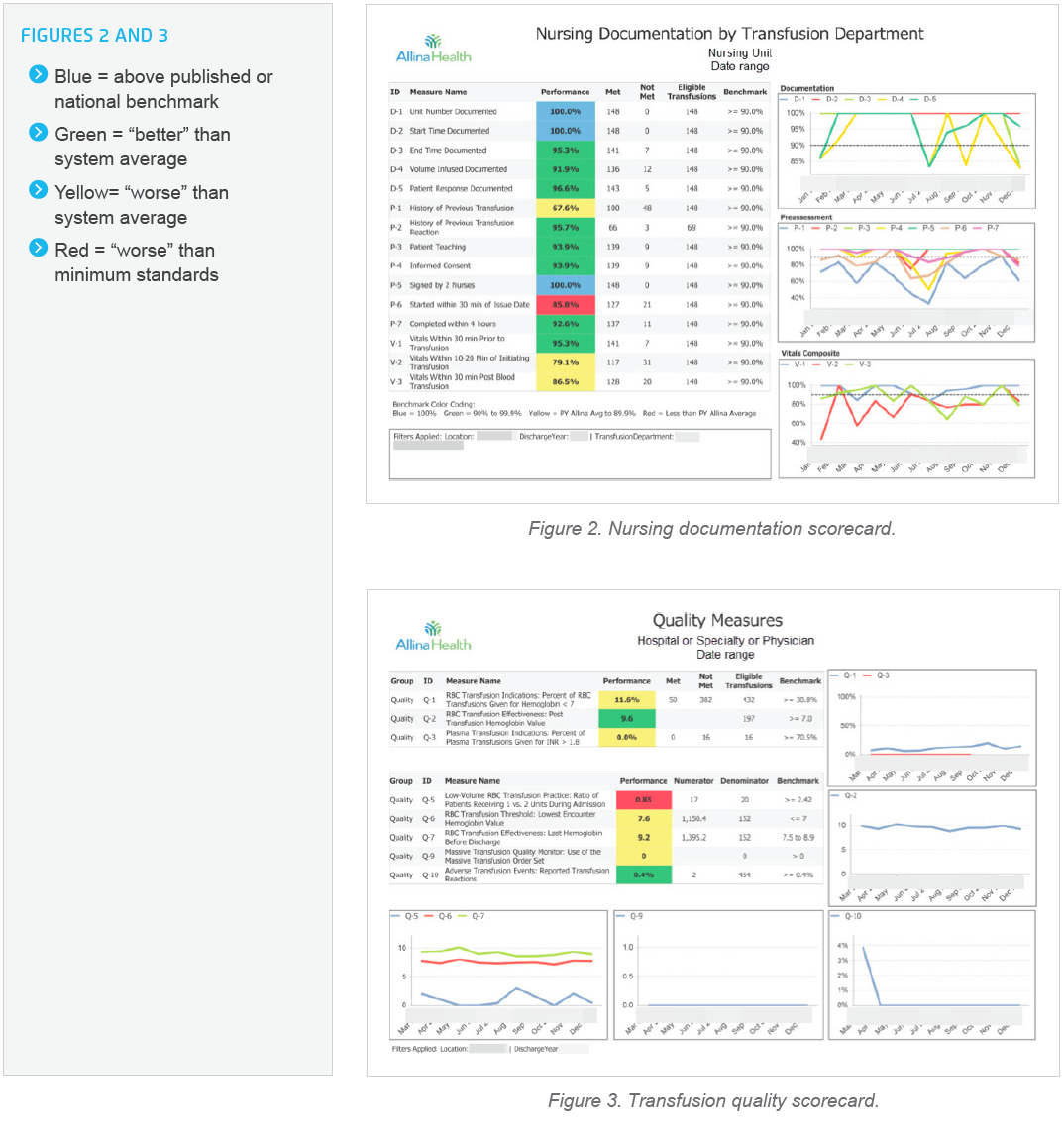
Allina Health uses its analytic platform to facilitate continuous outcomes improvement. The transfusion care council can easily review key parameters extracted for each admission to identify cases for additional review, supporting effective identification of potential care improvements.
RESULTS
After reducing the yearly cost of blood products by $3.2M, Allina Health has continued to improve its blood conservation program, achieving:
- Four-fold increase in the ratio of single vs. double unit red cell transfusions. (0.48 to 2.24).
- 32 percent decrease in plasma transfusion.
Additionally, the use of donated blood products in cardiac surgery has been further improved through a:
- Four-fold reduction in net prime volume of cardiopulmonary bypass circuit per case.
- 33 percent relative reduction percentage of blood transfusion for patients with a post-operative chest tube.
“The goal of patient blood management isn’t to transfuse less and less blood. We wouldn’t need analytics for that. The goal is to avoid transfusions that don’t benefit patients, and that’s where we need analytics. We need to link transfusions to value. With our dashboard, we can make the link between transfusion and outcomes like length of stay and readmissions.”
– Lauren Anthony, M.D
System Medical Director
Allina Health Laboratory
WHAT’S NEXT
Allina Health has begun work to correlate transfusions to outcomes, such as length of stay, readmission rates, and hospital-acquired infection rates. The goal of this work is to establish transfusion guidelines that optimize patient outcomes. Additionally, Allina Health plans to implement a system-level peer review process for transfusion practice, as well as include transfusion metrics as part of ongoing physician practice evaluations.
REFERENCES
- American Red Cross. (2017). Blood facts and statistics.
- Brown, J. D. (2008). The silent risks of blood transfusion. ResearchGate.
- Sheehan, E., & Parvizi, J. (2010). Blood transfusions can increase the risk of infection in orthopedic patients. Orthopedics today.
- Thomas, J. (2016). Blood transfusion best practices. Elite Learning.
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.