ACOs: Four Ways Technology Contributes to Success
This report is based on a 2018 Healthcare Analytics Summit presentation given by Joan E. Valentine, RN, MSA, Executive Vice President Visiting Physician Association, US Medical Management, and David C. Vezina, MBA, Chief Information Officer, US Medical Management.
Accountable Care Organizations (ACOs) are an important business model of today’s value-based care environment as they strive to provide quality, efficiency, and improved healthcare outcomes for patients. In an ACO, healthcare providers and hospitals come together with the shared goals of reducing costs and increasing patient satisfaction by providing high-quality coordinated healthcare to Medicare patients. The goal, according to CMS, is to ensure that “patients get the right care at the right time while avoiding unnecessary duplication of services and preventing medical errors.”
The idea behind an ACO is that if providers are incentivized to improve the health of their patients over providing a large volume of services, the cost of care will decrease. When an ACO succeeds at delivering high-quality care and reducing healthcare spending, the ACO shares in the savings achieved for the Medicare program.
What anyone who has participated in an ACO knows is that it is not always easy to get started. These organizations often lack direction, and it can be difficult to understand how to use data toward actionable interventions in improving care. Integrating real-time data and analytics into provider workflows can ensure patients receive the appropriate primary and preventative care, improve ACO Measure performance, and save Medicare money.
Accountable Care Organizations: Requirements for Success
Participants in both the ACO program or Medicare Shared Savings Program (MSSP) are subject to a number of Medicare quality reporting requirements and performance initiatives, such as the Merit-based Incentive Payment System (MIPS). An ACO’s quality composite score is based on the performance of MIPS Group Practice Reporting Option (GPRO) best practice preventative care and primary care measures. ACO participants may receive as high as a four percent upward or downward payment adjustment based on their quality composite performance. ACOs are successful when the organization improves patient satisfaction, improves care coordination, and reduces cost.
ACOs are required to demonstrate quality through four domains:
- Patient experience of care: Patients are given the Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey to assess quality of experience.
- Care coordination and patient safety: ACOs are assessed based on outcomes measures including ED use, ambulatory sensitive admissions, and readmissions. They also measure an organization’s use of electronic health data to ensure coordination between providers, and reduction of potential transcription errors for prescribing or ordering services.
- Preventive health: Standard assessments and screenings to increase early detection of various conditions, such as colorectal and breast cancer.
- At-risk populations: ACOs must meet nationally recognized standards for patients with chronic diseases, such as diabetes, heart failure, and chronic obstructive pulmonary disease.
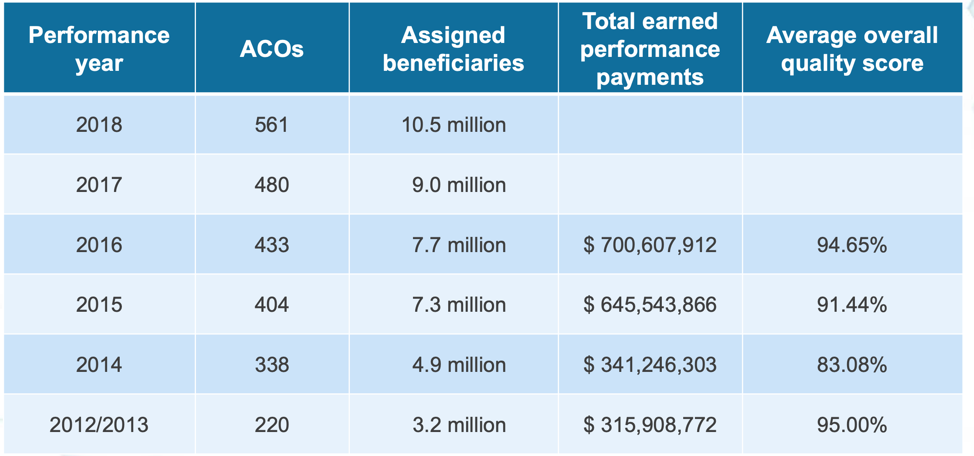
Participation in ACOs has been steadily growing since 2012. As shown in Figure 1, more healthcare providers and hospitals are participating in ACOs each year and their average overall quality scores, as well as performance payments are also rising.
Challenges for ACOs
Even though the accountable care organization model continues to grow, implementing such a model is no easy task. Below are just some of the common challenges to successful implementation:
- Available technology is not set up to meet the needs of an ACO. Investment in technology does not automatically mean success. An ACO needs to monitor EMR data, clinical and claims data, and more. A sophisticated analytics system is necessary to meet the analytic needs of an ACO’s quality reporting initiatives.
- Providers spend too much time on care coordination. Time spent by providers to review previous interventions is time-consuming. The manual processes may not provide the information needed at the point of care and may even detract from providers’ ability to focus on the patient. Physicians can experience lowered job satisfaction as a result.
- The organization’s financial viability is dependent upon shared savings. An ACO’s success leads to fewer hospital inpatient admissions, fewer procedures, and less fee-for-service reimbursement. There is often a dichotomy of trying to keep a head out of a bed versus the hospital’s need to keep heads in beds for their financial performance.
- Widespread understanding about the impact of documentation on measure performance is lacking. Few providers understand which documentation sources contribute to measure compliance, and the complex patient may qualify for as many as 12 measures annually.
- Lack of patient engagement. Healthcare providers can’t force patients to invest in their own care. It is up to them to make and keep appointments, adhere to a medication regimen, and monitor symptoms–all of which can contribute to medical costs.
Technology Enables Understanding of Performance
Transforming from a transaction-based system to a pay-for-performance based systems is a difficult process. Having the right technology and investing in that technology can help smooth the path forward for ACOs.
Steps to effectively implementing that technology might include the following:
- Build the data repository with an analytics platform. ACOs need something to bring all siloed systems into one place so they have access to they need once they have aggregated data. This requires a robust analytics platform to bring together all clinical, claims, and financial data into one place. Oftentimes, organizations have not had or utilized claims data before implementing an ACO, which can bring a wealth of knowledge into an analytics platform.
- Bring data to the point of care. Providers need to have a clear understanding of requirements in order to make decisions for patients that allow ACOs to meet quality requirements.
- Analyze claims data, identify outliers, including successes and failures. A robust analytics system allows ACOs powerful insights into data that help them meet quality metrics, such as the ability to drill down to the provider, department, or patient level, display the overall composite score performance, or display individual measure performance.
- Combine clinical claims, and quality data to identify opportunities for improvement. ACOs need to be able to prioritize opportunities based on identifying high risk patients and high-volume areas of inappropriate variation that significantly drive costs in order to effectively focus their resources. They also need to develop meaningful metrics for individual patient conditions (especially for chronic diseases) and for population health and wellbeing. This requires a highly sophisticated and flexible analytic system.
More Tips for Success for ACOs
Successful participation in the ACO program involves a lot of factors, beyond just technology. Other insights from successful ACO models include the following tips for success:
- Conduct deep dives into each measure to ensure data accuracy, including reaching out to CMS to clarify measure requirements.
- Conduct beta testing with providers and practice managers to validate accuracy and usability.
- Engage practice managers in active panel management.
- Clearly identify inclusion criteria, exclusion criteria, and denominator for each measure.
- Standardize provider workflow, including documentation in the EMR.
- Make sure providers have the information they need to understand the measure, documentation required to meet the measure, and location of that documentations in the EMR.
- Use an iterative process to identify and build measures within the analytics applications.
Healthcare organizations and providers increasingly need to focus on the health of patient populations, requiring care coordination and teamwork across specialties and organizations. A successful ACO model means the elimination of siloed views in favor of a more expansive and collaborative model of care delivery. In order to be successful, an ACO must address these challenges by leveraging a robust analytics system to automate the process of data gathering and analysis and aligning data with ACO quality reporting measures.
PowerPoint Slides
Would you like to use these concepts or share with a colleague? Download this presentation highlighting the key main points.
Click Here to Download the Slides
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.

