The U.S. healthcare market projects that by 2022 90 million Americans will be in an ACO. The upward trend in population health management (PHM) makes the move towards risk-based contracts increasingly urgent for health systems. The industry has been largely unprepared for the shift, as it hasn’t established a clear definition of population health or solid guidelines on transitioning from volume to value. Organizations can, however, prepare for the demands of PHM by adopting a solution that manages comprehensive population health data, provides advanced analytics from new and complex challenges, and connects them with the deep expertise to thrive in a value-based landscape.


The landscape of reimbursement in U.S. healthcare is changing and evolving, spurring increasing urgency for health systems to enter into risk-based contracts. But, despite this momentum, healthcare has lacked a clear definition of population health and well-defined guidelines on how to proceed towards value. To succeed in value-based care (VBC), organizations need comprehensive population health data, a platform that integrates and harmonizes data from multiple sources, and insights from expert partners.
This report discusses current trends in population health, the corresponding market response, and challenges to success and considers the requirements for a capable population health solution—both the technological and service components.
ACOs are continuing their upward trend nationally, both in terms of the number of lives covered and the number of models. According to Health Affairs, as of 2018, there were over 1,000 ACO models in the United States, covering 32 million lives. The market projects that, by the end of 2022, ACOs will manage 90 million lives, meaning an estimated one in three Americans will be in an ACO model.
There’s growth across the ACO market overall, but more significantly, there’s growth across contract types. While commercial ACOs lead in terms of numbers, trends show commercial organizations slowing down, while Medicare ACOs are steadily rising. Medicaid ACOs are also growing nationally.
Several notable events and trends are driving the trend towards risk bearing:
In making changes to the MSSP model that nudge health systems to take on more risk more quickly, CMS differentiates between high- and low-revenue ACOs, asking high-revenue ACOs to take on risk more quickly than low-revenue ACOs. Attribution is also shifting, allowing ACOs to elect prospective beneficiary assignments, and some retrospective reconciliation, as well as expanded use of regional factors and benchmarking.
Medicare Advantage is experiencing ongoing growth. In 2019, more than 20 million Medicare beneficiaries (i.e., one in three Medicare patients) are enrolled in a Medicare Advantage plan. Between 2017 and 2018, enrollment in Medicare Advantage grew by about 8 percent, an identical growth rate compared to prior years and a significant and ongoing yearly increase.
To encourage organizations to take on more risk, in April 2019, CMS announced its Primary Cares Initiative, which aims to accelerate the movement from volume to value. CMS announced five sub-models within the Primary Cares Initiative; overall, these models recognize that primary care is the medical home base for the patient and ties payment to what’s taking place in the primary care practice.
The Primary Cares Initiative comprises topics encompassing two types of models and a total of five sub-models:
The Direct Contracting payment models have a similar theme of transforming primary care but aim at a different audience than the Primary Care First programs. These three models aim to draw in entities such as ACOs, Medicare Advantage plans, Medicaid, and managed care organizations (MCOs) with experience in taking on financial risk and serving much larger patient populations. And, similar to the Primary Care First models, participation in these models would involve fixed monthly payments and, ultimately, payment tied to outcomes.
Health and Human Services (HHS) anticipates that about a quarter of traditional Medicare beneficiaries may be opted into some of these initiatives.
Much of the shift to taking on risk for populations is taking place among self-insured employers, who are exploring innovative approaches to better managing their employee populations. Haven—the joint venture between Amazon, JPMorgan Chase, and Berkshire Hathaway—is one intriguing example. Though not much is known about Haven, its stated focus areas include easing healthcare system navigation and access to affordable treatment and prescription medication.
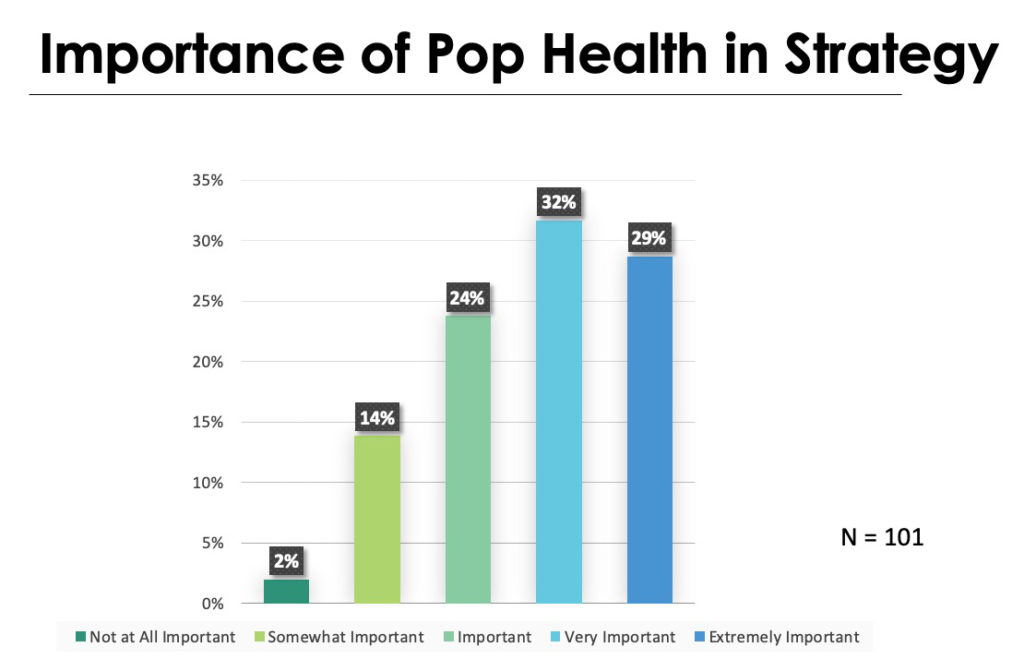
As VBC continues to grow, driving innovations and new risk arrangements, population health remains a high priority. In a 2019 Health Catalyst poll of 101 healthcare leaders from across the U.S., over 60 percent responded that population health was either very important or extremely important (Figure 1). Only 16 percent said it was somewhat important or not at all important. So, very clearly, and despite its changes and dynamics, population health remains a high national priority.
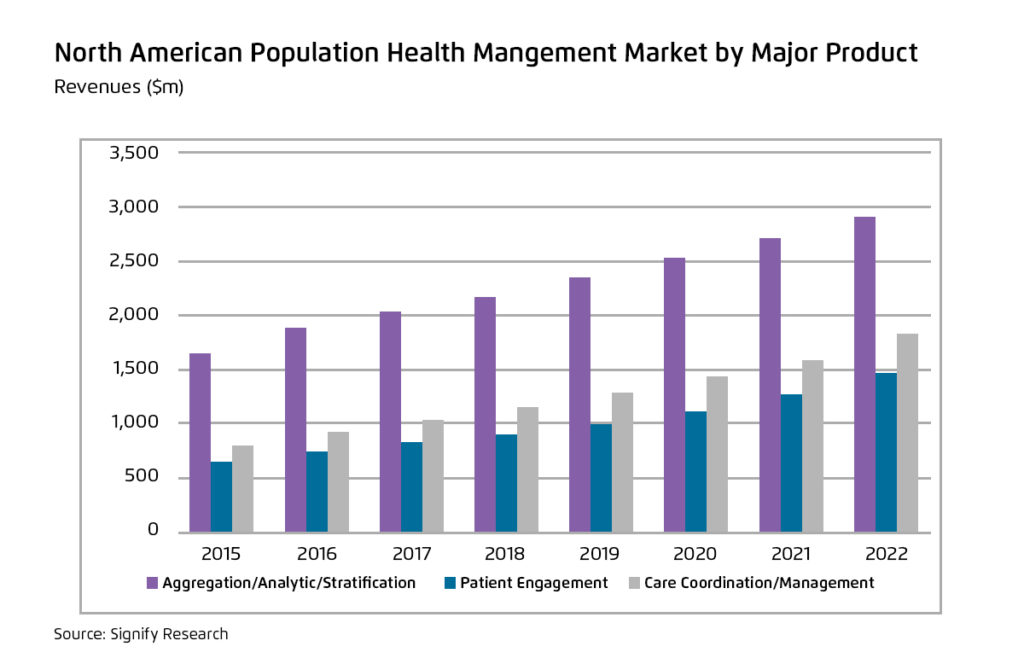
Signify Research, a market research company specializing in population health, has also tracked definite trends upwards in population health (Figure 2). They’ve broken the market into three product areas:
The purple bars in Figure 2 represent the aggregation, analytics, and stratification components of the market.
On the other side of the ACO growth story, a number of ACOs are dropping out. Entry and exit trends over time show that while there were 232 new ACOs in 2017, during that same time, 35 ACOs exited the program. Many ACOs are still struggling to succeed in improving performance while lowering trends. With a likely net increase in ACO growth, there will also be an ongoing flow of organizations leaving the ACO model.
Healthcare organizations can’t simply ride the momentum towards population health; they must understand and address its key challenges. Common barriers to VBC success include the following:
As population health trends upwards, organizations need specialized resources and capabilities in place to meet these critical needs:
With the above challenges, plus the lack of a standard industry definition of population health, organizations may benefit from a key-step framework (e.g., the Health Catalyst® Population Health Management Transformation Framework, Figure 3) as they transition from fee for service to fee for value. The right solution for risk management today requires a data- and analytics-first approach, a platform that aggregates data across multiple sources, and partners with deep expertise in PHM.

Health systems can embark on the following foundational steps to transform to population health organizations:
As health systems and ACOs build population health capabilities, they’re rightly interested in cost-effective, rapid time-to-value solutions. Point solutions can appeal but don’t have the robust data capabilities for the long haul, as most typically operate from a limited set of data.
Capable data platforms must support a growing and dynamic list of data sources. The right population health solution creates a strong foundation in data and analytics, allowing organizations to meet their most pressing population health needs while laying the foundation for a scalable, adaptable future.
The Health Catalyst® Population Health Foundations Solution, for example, blends technology and services to support population health transformation and ongoing success. These tools and services help organizations leverage multiple data sources to understand their patient populations and create meaningful views of financial and clinical quality performance.
Key elements make the Health Catalyst Population Health Foundations solution effective in supporting the needs of risk-bearing entities:
With a projected 90 million Americans in an ACO by 2022, the transition from volume to value is becoming a greater reality for U.S. health systems. Organizations must now get serious about volume-to-value transformation, from acquiring and managing the needed comprehensive population health data to ensuring they have the analytics platforms and expert guidance to support their journey. An organization’s best bet is a population health solution that delivers the appropriate capabilities, technology, and understanding and is fully customizable to a health system’s individual needs.
Would you like to learn more about this topic? Here are some articles we suggest: