Sustaining healthcare improvements is challenging, with less than 40 percent lasting long-term. MultiCare improved outcomes for patients undergoing elective colon surgery, including reducing 30-day readmissions, length of stay, and surgical site infections through ongoing engagement and performance monitoring. Utilizing data insights and provider feedback, the organization maintained improvements and uncovered new improvement opportunities.
For healthcare organizations, sustaining improvements that have been adopted in more than one part of an organization remains a serious challenge. After improvement initiatives have been successfully implemented, it is estimated that less than 40 percent of gains are sustained in the long term. Because improvement initiatives are necessary to maintain a high standard of care, sustaining them so that further improvements can be made remains a top priority for health systems.
MultiCare Health System, a not-for-profit healthcare system serving Washington state, successfully implemented improvement efforts for patients undergoing elective colon surgery, which resulted in significant reductions in 30-day readmission, LOS, and surgical site infections (SSIs). However, without ensuring ongoing engagement, accountability, and visibility into performance, MultiCare was concerned improvements could slip away. By supporting continued monitoring powered by insights gained from relevant data, and by closely listening to provider feedback, MultiCare was able to sustain previous improvements while identifying new opportunities.
It is estimated that fewer than 40 percent of healthcare improvement initiatives successfully result in sustained implementation that is spread to more than one area of an organization.1 Having achieved high levels of clinical quality and safety, organizations with reputations for excellence are increasingly focused on sustaining improvements after adoption, ensuring care and support processes continue to perform at the new levels of quality and safety.2
Nationally, readmission within 90 days after colorectal surgery occurs in about one in four patients and is associated with a cost of approximately $9,000 per readmission, accounting for $300 million in total readmission costs annually.3 The incidence of SSIs is also high in this patient population, with approximately 20 percent of patients undergoing colorectal surgery developing an SSI.4
MultiCare is a not-for-profit healthcare organization with more than 18,000 team members, including providers, employees, and volunteers. As the largest community-based, locally governed health system in the state of Washington, its mission is partnering with the community for healing and a healthy future. While the healthcare system had achieved success with its initial colon surgery improvement efforts, MultiCare leadership knew that sustaining colon surgery improvements was necessary for further improvements to be discovered.
By previously engaging a multidisciplinary Surgery Collaborative in the development and implementation of an enhanced recovery after surgery protocol, MultiCare significantly improved the outcomes for patients undergoing elective colorectal surgery, achieving a 19 percent relative reduction in readmission rates, 22 percent relative reduction in LOS, and an 85 percent relative reduction in the incidence of SSI.
While the Surgery Collaborative achieved the desired results, MultiCare was aware that without ongoing engagement, accountability, and visibility into performance, its results could slip away over time. Without a purposeful sustainability plan in place, it risked the possibility of losing ground on the previous improvements. To maintain and further improve patient outcomes, MultiCare recognized it needed to prioritize the development of a robust sustainability plan.
To sustain the improved outcomes for patients undergoing elective colorectal surgery, MultiCare has invested in ongoing support of the Surgery Collaborative, which is a key driver for high surgical team performance. The Surgery Collaborative is organized to anticipate and detect defects in the standard processes that yield the desired results, ensuring that best practices are further refined and improved as new evidence becomes available.
A key part of the Surgery Collaborative’s work is continual monitoring of patient outcomes, enabled by the Health Catalyst® Analytics Platform and broad suite of analytics applications. Performance data from the analytics platform is easily accessible via a desktop application for providers and leaders, offering a visualization of performance for elective colon surgery. The analytics application includes visualization of both outcomes and process measures, all of which can be viewed at the system, facility, unit, and/or individual provider level (see Figure 1).
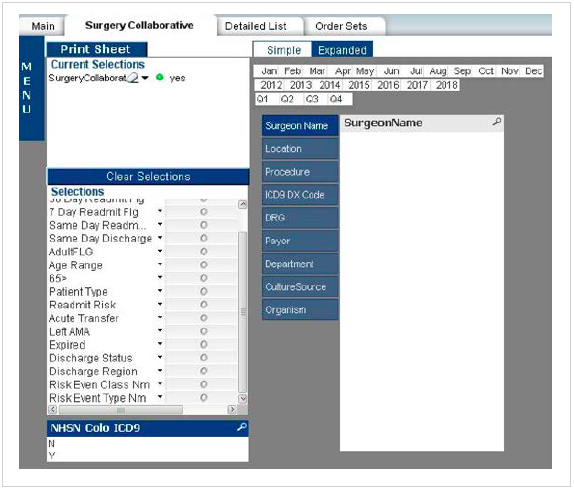
A weekly review of process measures, such as order set utilization, is conducted with the goal of detecting and promptly responding to any deterioration in the standard process. This review supports early communication with the providers and frontline staff, prompt feedback, and timely adjustment of the medical treatment plan as appropriate.
As part of its ongoing work, the Surgery Collaborative uses the analytics platform to conduct a deep dive review of elective colorectal surgery outcomes measures each quarter. The team closely reviews SSI rates, LOS, and 30-day readmission rates, using the analytics application to review patient level detail when appropriate (see Figure 2).

The Surgery Collaborative carefully analyzes surgical outcomes, looking to identify any potential system issues, breakdowns in processes, or deviations from the established standard of care. For example, the Surgery Collaborative identified there were gaps in the onboarding of new providers that resulted in decreased utilization of elective colorectal surgery order set and protocol, which in turn increased provider variability and decreased the consistency of care.
These gaps could potentially put sustaining the improved patient outcomes at risk. Informed by this new data, the Surgery Collaborative was able to prioritize use of resources to improve the new provider onboarding process, orienting them to the MultiCare standard for elective colorectal surgery.
In such instances when deviation from standard order sets and protocols remain despite communication from process leaders, physician champions provide peer-to-peer education on the standard of care, addressing gaps in order set utilization and protocol compliance, while encouraging use of the evidence-based care standards that have demonstrated improved patient outcomes. The physician champions also solicit feedback about any barriers to using order sets and protocols, all in an effort to fix potential problems as quickly as possible.
Understanding the importance of sharing success within the organization, the Surgery Collaborative leaders and nursing leadership provide frontline staff ongoing feedback about performance, sharing information about the positive impact of the standardized care on patient outcomes, providing coaching to ensure consistent performance, while also obtaining feedback from the staff about future opportunities to improve. On a quarterly basis, Surgery Collaborative meetings are held to determine how to refine the protocol in order to further improve outcomes for complex patients with comorbidities, such as those who have diabetes and are planning to have elective colon surgery.
In just one year, by applying principles for sustaining comprehensive, evidence-based practices across the care continuum, MultiCare’s Surgery Collaborative was able to not only sustain—but also to further improve upon—its previous improvements, achieving an additional:
MultiCare was able to sustain a:
Among patients who had the complete enhanced recovery after surgery protocol implemented for elective colon surgery, there were no surgical site infections in the past year. Additionally, MultiCare has sustained a high order set adoption of greater than 85 percent across the system, which has contributed to sustained performance.
“Our continued focus on keeping providers engaged in the process and communicating patient outcome information, has helped us to sustain and improve our gains.”
– Jennifer Yahne, Director, Surgery, Urology, and Gastroenterology, Service Line, MultiCare Health System
MultiCare is committed to further improve surgical outcomes by spreading these proven strategies to other surgical populations. It has already developed and implemented a standard protocol and order set for ileostomy. Next, MultiCare plans to focus its improvement efforts on outcomes for patients having small bowel surgery.




