Read how Allina Health is transforming healthcare by embracing a vision of the future where 100 percent of healthcare services add value, and everyone has access to quality, compassionate care. Utilizing data and analytics to drive its improvement efforts, the health system has continued to improve and sustain outcomes.
Wasteful spending in healthcare now exceeds $1 trillion annually, which is double the money required to fund Medicare each year. Allina Health, a non-profit healthcare system, embraced a vision of the future where 100 percent of healthcare services add value, and everyone has access to quality, compassionate care.
Allina Health president and chief executive officer Dr. Penny Wheeler recognized the critical importance of data and analytics to measure and track performance. To meet those needs, the organization leveraged its analytics platform, using the integrated clinical, financial, and operational data to enable, measure, and scale data-driven improvement initiatives. With input from users, the analytics platform delivers ready access to the data and information providers and operational leaders need to improve and sustain outcomes.
Penny Wheeler, MD, president and CEO of Allina Health, has had an opportunity to look at the healthcare system from many lenses and perspectives. As an OB/GYN physician, she learned firsthand the challenges that clinicians and patients face every day in a healthcare system that can be fragmented, complex, and reactive. As the chief clinical officer at Allina Health, she was deeply involved in quality improvement at Allina Health and in the community, serving on community boards and collaboratives that focused on improving access and affordability. As CEO, she led Allina Health to become one of the top healthcare organizations in the country.
At Allina Health, a non-profit healthcare system dedicated to the prevention and treatment of illness and providing whole-person care to individuals, families, and communities throughout Minnesota and western Wisconsin, Dr. Wheeler has demonstrated that reducing waste in healthcare is an achievable and necessary goal, making healthcare affordable by improving care for those served. She believes that reducing waste is the key to addressing the polarity of enabling widespread access to quality care, while also ensuring financial accountability and sustainability of the healthcare system.
Wasteful spending in healthcare now exceeds $1 trillion annually— double the money required to fund Medicare each year.1 Despite spending more on healthcare than other high-income countries, health outcomes in the U.S. are poorer than other countries, with the U.S. ranking last in healthcare system performance.2
Healthcare delivery is costly, fragmented, and complex. Patients struggle to navigate the healthcare system and how to pay for it. Sometimes, a patient must choose between putting food on the table or paying for needed medications, and as a result, experience additional suffering and stress.
Knowing that approximately 30 to 40 percent of healthcare is wasted, such as preventable complications, over-treatment, inefficiencies, and errors, Dr. Wheeler embraced a vision of the future where 100 percent of healthcare services add value, and everyone has access to quality, compassionate care.1 She believes that nothing less than a transformation of healthcare is needed to create a system that is compassionate, sustainable, integrated, and proactive. By making healthcare quality better, organizations can make it more affordable.
The required transformation is driven by quality improvement, a powerful driver of cost containment, leading to improved value and care. To support Allina Health’s journey to becoming an organization that successfully and continuously drives improvement, Dr. Wheeler and her team put key elements in place.
When an aligned and functional organizational structure is in place, and everyone is rowing in the same direction, productive collaboration and partnership occur between operational leaders, providers, employees, and the community. This synergy supports the work at Allina Health.
To enhance its healthcare system, Allina Health aligns the purpose, economic incentives, and clinical activity of its providers, both employed and affiliated, through the following ways:
This structure brings operational and clinical leaders together as partners on improving care and enables a clinically integrated network of employed and affiliated providers, allowing them to share in market rewards based on market-based risks.
Allina Health’s quality improvement work is supported by a structure of eight clinical service lines, which are structured based on patient care conditions and needs. The health system’s clinical service lines include:
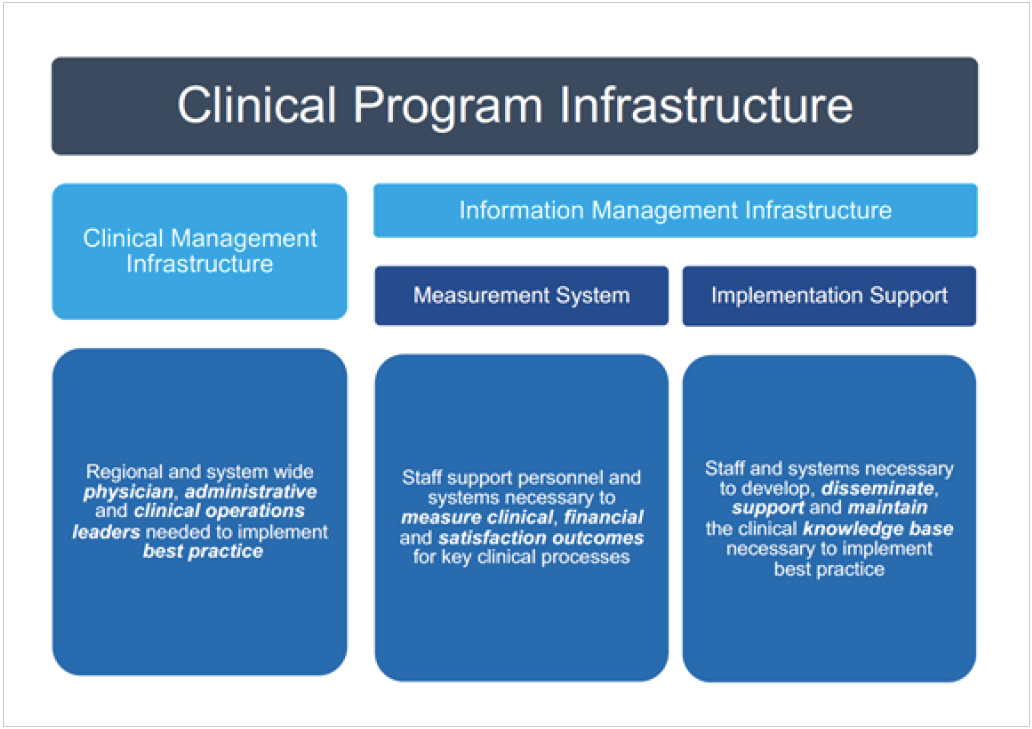
Its clinical program infrastructure is comprised of regional and systemwide physician, administrative, and clinical operation leaders that collaborate on implementing best practices, supported by the data, analytics, and visualizations needed to recognize, monitor, and measure performance—critical elements required for effective quality improvement (see Figure 1).
Dr. Wheeler recognized the critical importance of data and analytics to measure and track performance. To support its data-driven approach to improvement, the organization leveraged the Health Catalyst® Analytics Platform and broad suite of analytics applications, using the integrated clinical, financial, and operational data to enable, measure, and scale data-driven improvement initiatives.
The analytics platform gives providers and operational leaders ready access to the data and information needed to improve and sustain outcomes. These applications and visualizations are then created with input from users. For example, when the spine care analytics application was developed, the community came together and decided what was most important to them and determined how visualizations would look. The analytics application automatically updates with the most recent data, enabling providers to drive and sustain goals with minimal IT support. Rather than spending time obtaining data, analysts can now be deployed to other more value-added tasks.
Allina Health promotes widespread data access, exposure, and transparency, opening its analytics applications and unleashing the data, so the whole team has the data required to continually improve. Providers have embraced data transparency and recently voted to have comments from patients, both positive and negative, included in the analytics applications. Providers, operational leaders, and employees actively review data, learning from high performers, using the information to continuously improve the patient experience.
Healthcare lags behind other industries in looking at consumer insights, and although the concept of patient-centered care has been around for years, most healthcare organizations have not asked patients what is important to them, what is causing them stress, and what can be done.
To address this gap, Allina Health has a patient advisory group and includes patients in process improvement teams. Dr. Wheeler advocates for designing care processes with consumers at the table, believing that involving patients in improvement efforts has made a significant difference in Allina Health’s ability to improve care processes and produce meaningful outcomes.
Having the patient’s perspective at the table is important and impacts improvement teams, as is illustrated by the breast program committee. The improvement team suggested measuring and improving the time from when a woman is called to schedule a mammogram appointment to when the appointment is scheduled. Patients advised that it would be far more impactful and meaningful for Allina Health to shorten the time from when a problem was identified by the mammogram to the time of the first appointment with the provider, as this period between problem identification and a plan for treatment created stress and anxiety for patients.
Dr. Wheeler is proud of the many significant clinical improvements that Allina Health has achieved, and yet, she knows it is not enough. Although the organization has improved care, health is much more than clinical episodes. It includes the whole person and their life outside of the clinic or hospital. Dr. Wheeler believes that something profound happens when providers and employees get to know the patient as a fellow human being.
Allina Health elected to adopt a fresh approach, in addition to improving clinical care and reducing waste but, striving to provide “whole person care,” an approach that recognizes all the factors that impact health are connected—mind, body, spirit, and community. This method requires moving from just asking “what is the matter” to “what matters to you?”
Whole person care asks patients about issues that impact their health and then connects patients to resources in their communities to help meet their unique identified needs. Through whole person care, Allina Health can help ensure equitable healthcare for all.
As numbers alone do not convey the impact on patient lives, patient stories are shared with providers and employees, allowing them to see the bigger impact their efforts have had on the lives of those they serve. These anecdotes further engage the hearts and minds of the care team, increasing the commitment to improvement efforts.
Allina Health’s strategy to embed healthcare quality in the organization has resulted in significant improvements. Dr. Wheeler credits her teams, the patients, providers, and employees with the success of the projects, as they have worked to make quality more impactful, are dedicated to getting to what matters most and to what benefits the people of the community, and the organization. Notable improvements include:
“In healthcare today, 30 to 40 percent of what we pay for is waste. In the future, there won’t be more healthcare dollars available—money needs to be directed to activities that add value.”
– Penny Wheeler, MD, President and CEO, Allina Health
Allina Health will continue to embrace quality as a strategy to transform care, keep expanding whole person care, and implementing innovations that will better serve its patients and the community.




