In today’s high-pressured world of healthcare, health systems don’t need report writers. They need highly valuable healthcare data analysts. A top healthcare data analyst becomes a partner for clinical and operational improvement by using a five-step method for solving complex problems.
This article walks through this step-by-step approach and demonstrates its application using the real-world example of building a diabetes registry. In addition to this specialized approach to solving problems, the article discusses the five essential skills for data analysts needed in the diabetes registry example:
• Data query
• Data movement
• Data modeling
• Data analysis
• Data visualization
 Download
Download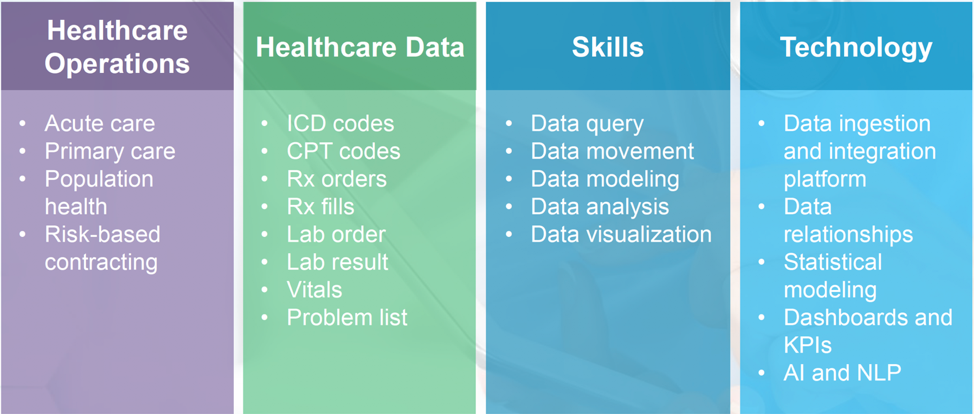

External factors are re-shaping the healthcare delivery landscape: mergers and acquisitions, at-risk contracting between payers and hospitals, a combination of reimbursement models, and a complex payer mix. This is the reality of healthcare today. There’s a real need for healthcare analysts to understand the pressures on the system so that their analyses can help leadership develop strategies that will improve care delivery and keep the clinic doors open and profitable.
For a top-performing healthcare data analyst, it’s insufficient to simply model and forecast increasing volumes and charges. She must do that and explore care models that deliberately drive profit away from hospitals into ambulatory settings while being mindful of the impacts (good or bad) regarding their at-risk contracts. She must also think about getting much further upstream in a care continuum to support population health initiatives.
Health systems don’t hire analysts to run reports or build dashboards. They don’t hire analysts to leverage the fancy technology they purchased. These duties may be assigned to an analyst, but that’s not where their value lies. They hire healthcare data analysts to solve problems–period. This article demonstrates the step-by-step problem-solving approach used by the best healthcare data analysts today and walks through a real-world example that shows how this ability provides tremendous value to healthcare organizations.
The best healthcare data analysts maximize their value to the organization by using their problem-solving skills to become a partner for clinical and operational improvement. They also use a common approach to solving problems. Their approach involves the following pattern of thinking:
Step 1. Healthcare Operations – First, the top healthcare data analyst asks lots of questions that seek understand, “What is the problem we’re trying to solve?” and “Why does it matter?” This deliberate questioning helps to tease out the best opportunities.
Step 2. Healthcare Data – Next, the analyst asks, “What information would be needed to help solve this problem?” Top analysts turn data into information so what they’re getting at is, “What data do I need to begin to address the issue and where do I find it?”
Step 3. Technical Skills – After finding the data, the healthcare data analyst then asks, “How does this data need to be organized, analyzed, and presented to address the problem?” And, “Who do I need to present this information to so they can make a decision based on the information I’ve shared?”
Step 4. Tools – The last step top analysts take is to reach for their tools. This process reframes the role of technology. When analysts see their role as problem solvers, they effectively become partners for clinical, financial and operational teams.
The pairing of technical aptitude with domain expertise becomes a sustainable model for analysts to become a tremendous asset to be leveraged. In the words of Jim Collins in Good To Great, “Technology cannot turn a good enterprise into a great one, nor by itself prevent disaster.” The same holds true for analysts. No technology will make someone a great healthcare data analyst.

While this model is simple to understand, it’s rather difficult to implement. One of the most challenging aspects of this model is the interchange between technical experts and domain experts. That interplay is fascinating to observe. The manner in which clinicians are trained to think about data is strikingly dissimilar to the way analysts think about data and when the two are in the same room together, there is a real risk that they will talk past one another. Great analysts have learned that for them to add value, it’s not about what they say, it’s about what their audience hears that matters.
Looking at a real-world use case of building a diabetes registry will help illustrate this. The design of the registry begins with the why: “Why do we need to build the diabetes registry?” Through questioning of the right stakeholders, the analyst learned that the organization has embarked on a population health initiative as part of a marketing campaign to raise community awareness and healthy living. The timing of this contract coincided with an increased physician network of primary care clinics.
The focus for the initial registry build is in support of population health and the target audience is primary care physicians with diabetes on their panels. With further questioning, the analyst learned that the primary care physicians are excited to have a more robust set of clinical definitions for who has diabetes. But, they’re also concerned about being held accountable for diabetics on their panels if the patient-provider attribution model is not clear. This told the analyst he needed to get physician buy-in.
He also learned that a small portion of physician compensation is tied to the effective management of the diabetic population, making the attribution model accuracy even more important. By listening carefully and asking lots of questions, he developed a rule-set for the diabetes population, driven by the PCPs (Figure 2).

Looking at this list of qualifiers, do any seem peculiar? Knowing that the business driver for this registry is a population health initiative with a focus on PCPs treating diabetics in the ambulatory setting, the inclusion of rules one and two is especially brilliant.
Here’s why: physician leadership points out that an inpatient or ED visit for diabetics could be viewed as a potential failure within the population health effort. The analyst took this to heart. By creating the rules through careful questioning, the analyst was able to establish a baseline that was illuminating for the population health clinical leadership. It showed a significant number of diabetics were slipping through the cracks, much more than this health system had anticipated.
Through a simple but elegant analysis of the rules, the analyst learned the following:
In this example, the healthcare data analyst was able to highlight genuine opportunity for improvement because he understood the problems the clinicians and leadership were trying to solve. This analysis ultimately informed the strategy for population health.
In this diabetes registry example, in order to accurately populate the clinically-defined rule set, the analyst needed to understand which data elements were both available for use and approved by key stakeholders. For these rules, the analyst used ICD codes, Rx orders and fills, lab orders and results, and the problem list within the EMR.
Of course, not all ICD codes were used nor needed: only those that were specific to diabetes and even more detailed in definition, only those that were a primary diagnosis for an inpatient or ED encounter. Similarly, only A1C lab orders and results came from the laboratory data system or EMR.
Healthcare analysts have been given an incredible gift through the use of coding systems. The embedded meaning associated with these codes can be exploited to produce powerful analysis. But these can only be leveraged if the analyst understands the healthcare data captured within coding systems. An expert analyst of this caliber must have a deep understanding of the inherent meaning in coded data, where it’s captured, and why it’s captured in clinical work flow.
The best analysts are in top technical form. In the diabetes registry example, let’s quickly walk through how these technical competencies shaped the building of the cohort.
Later a tool like Qlik or Tableau consumed the subsequent data models and highlighted the baked-in analysis, but this wasn’t necessary for the inclusion criteria.
These are the five technical skills absolutely necessary for analysts to seize the best opportunities within healthcare systems. To be an effective healthcare analyst will require technical aptitude, the data skills outlined above, coupled with knowledge of healthcare data and operations.
The more analysts understand the problems their health systems are trying to solve, the more value they will be able to provide with their insights. The lessons for healthcare data analysts and healthcare leaders are clear. Healthcare leadership must strive to elevate the role of the healthcare analyst to be a problem solver, not just a report writer. The best analysts harness technology without becoming overly reliant on it supplanting the five key data skills. They must understand the business needs to provide maximum value to the organization. And lastly, healthcare leaders need to invest in education for analysts to grow deeper into healthcare data and operations understanding.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download the presentation highlighting the key main points.
Click Here to Download the Slides
https://www.slideshare.net/slideshow/embed_code/key/Dg0yra6dhmlarX