Health systems alike struggle to effectively manage hospital patient flow. With machine learning and predictive models, health systems can improve patient flow for different departments throughout the system like the emergency department. Health systems should focus on three key areas to foster successful data science that will lead to improved hospital patient flow:
Key 1. Build a data science team.
Key 2. Create a ML pipeline to aggregate all data sources.
Key 3. Form a comprehensive leadership team to govern data.
Improving hospital patient flow through predictive models results in reduced patient wait times, reduced staff overtime, improved patient outcomes, and improved patient and clinician satisfaction.
 Download
Download

This report is based on a 2019 Healthcare Analytics Summit presentation given by Michael Thompson, MS Predictive Analytics, Executive Director of the Enterprise Data Intelligence at Cedars-Sinai Medical Center, entitled, “New Ways to Improve Hospital Flow with Predictive Analytics.”
One of the never-ending challenges healthcare systems face is managing hospital patient flow—the movement of patients through the hospital from entry to discharge. If not managed effectively, patient flow can have negative ripple effects throughout the health system:
Efficient hospital patient flow allows newly admitted patients to get to the right place as soon as they enter the hospital, current patients to seamlessly transition to the right unit, and patients who are ready for discharge to leave the hospital with as little delay as possible. When hospitals manage hospital patient flow effectively, the health system and the patients win—hospitals don’t keep patients longer than necessary and patients spend the minimum amount of time at the hospital, making room for new patients who need care.
One way for health systems to improve hospital patient flow is through machine learning (ML). Because hospital patient flow is so complex and full of moving parts, ML offers predictive models to assist decision makers with hospital patient flow information based on near real-time data.
For example, an academic medical center created an ML pipeline that leveraged all its data—patient data, EHR data, clinical and claims data—to predict length of stay, emergency department (ED) arrival, ED admissions, aggregate discharges, and total bed census. The predictive models proved effective as the medical center reduced patient wait times and staff overtime and improved patient outcomes as well as patient and clinician satisfaction.
ML can be an effective tool to improve hospital patient flow and alleviate capacity strain burdens. The goal of ML is not only to create predictive models, but to ultimately improve, and in some cases fix, the challenges that arise from poor hospital patient flow:
Introducing data science requires strong leadership support at the highest level. Introducing the value of data science to executive leaders and taking a centralized approach to all data analytics within the health system fosters an environment for data science to succeed. With C-suite support and one data science team, data scientists are ready to work with other departments and turn data into intelligence that drives better decision making.
To leverage all the data available to a health system, the data science team should create an end-to-end ML pipeline (Figure 1) aggregating the data. The pipeline should include all data sources, storage, transformation and modeling, and visualization components. It is vital that the ML pipeline include every data source because if the data isn’t accurate or doesn’t provide a complete picture, the predictive models won’t identify the right areas for opportunity, resulting in wasted effort.

To make the ML pipeline more friendly and less intimidating to other team members, data science leaders should consider calling the data pipeline by a human name like “Alex” instead of “machine learning”. Using a common name helps team members focus on the insight from the predictive models and not that the insight was derived from a machine.
Another important piece for ML success is to include leaders from other departments. This has two benefits: 1. It ensures multiple viewpoints when discussing the data science strategy within the health system, and 2. It helps garner support for data science from a variety of departments throughout the organization. For example, a comprehensive leadership team could include leaders from departments like operations, nursing, patient satisfaction, case management, and providers/clinicians so that the data science team can develop champions for data science across other departments. Creating data science champions who are not members of the data science team makes data science implementation more likely to succeed and helps team members trust it more when they see their leaders—whom they already trust—trust and support it.
Another important step in achieving long-lasting institutional support for ML is the importance of back-testing models—meeting with team members to show them how well the model performed compared to what actually happened. Back-testing models increases transparency and sets realistic team member expectations about predictive models —that they aren’t perfect.
Reviewing the accuracy of the model with teams may also foster brainstorming discussions that lead to ideas for new models or other explanations about why the models were inaccurate. These alternative explanations can offer insight to what should be included in the next iteration of the model, further increasing accuracy.
Another valuable practice when discussing ML models with team members is to use a variety of models and compare which models are the most accurate. Comparisons help team members understand that different models have varying degrees of accuracy and that no models are ever 100 percent accurate.
Asking team members to share their thoughts about the machine learning findings (usually displayed in a graph) gives team members a chance to interact with the models. Rather than listening to the data analyst report on the findings, they have an opportunity to interact with the data and participate in the process that is data science.
In the process of refining the model, leaders and team members become invested in the model, offer suggestions for improvement (like adding new data variables), and eventually own the model. This is one strategy for increasing participation and support for data science that leads to data democratization.
It can be tempting for data science teams to disseminate information from the predictive models on a daily basis. The problem with daily information is that executive leaders develop data fatigue—seeing the same email with slightly different numbers every day makes it hard to focus on what the numbers mean and eventually tend to ignore the emails.
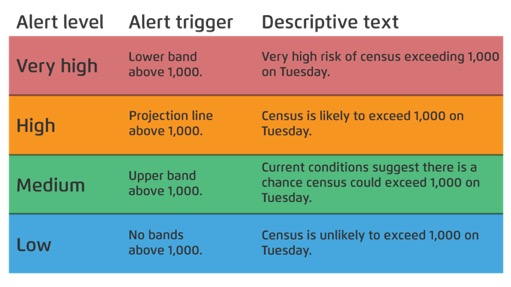
In order to prevent data fatigue, but still effectively communicate the predictive model findings to executive leadership, the data science team can send information in the form of alerts (Figure 2). For example, the alerts are triggered whenever the alert level for one of the next three days is either high or very high—a condition set by a health system’s leadership team so they are notified only when they feel it is necessary.
Hospital patient flow challenges are not a single department problem but a problem the entire health system should strive to overcome. To effectively improve hospital patient flow, it is imperative for operational and clinical leaders to be involved from the start in order to recognize the value of data science.
The data science team has a responsibility to democratize data—ensure its availability to decision makers at every level. However, access to data doesn’t mean that the interpretation of data will be uniform. The data science team should equip leaders with easy-to-understand models at first and work closely with them until they feel comfortable, slowly building their analytics acumen.
An agile approach to data science allows leaders to experience the data, not just review it. Agility within ML is crucial because with each model iteration, participation from a clinician or an administrative leader increases their understanding and, as a result, the accuracy of the predictive model. At this point, leaders throughout the organization are referencing data and then leveraging it to make decisions.
ML models can improve hospital patient flow, but only do so effectively when leadership adds valuable perspectives through suggesting new variables to consider in the predictive models. When ML and committed team members come together, ML is more accurate because it is sensitive to a health system’s needs, schedules, insurance plans, and most importantly, its patients.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download the presentation highlighting the key main points.
Click Here to Download the Slides
https://www.slideshare.net/slideshow/embed_code/key/uJghiYCtfn1eXx