Health systems have vast amounts of data, but frequently struggle to use that data to solve strategic problems in a timely fashion. A healthcare analytics team, made up of the right people with the right tools and skillsets, can help address these challenges. This article walks through the steps organizations need to take to put an effective analytics team in place.
These include the following:
• Recognizing the need for change.
• Demonstrating the value of an analytics team.
• Conducting a current state assessment.
• Identifying solutions.
• Implementing a phased approach.
• Building a roadmap.
• Making the pitch.
• Putting the roadmap into action.
The article also includes the foundation skills to look for when putting together the team and tips on how best to organize.



This report is based on a 2018 Healthcare Analytics Summit presentation given by David M. Wild, MD, Vice President of Lean Promotion, and Chris Harper, MBAi, MPM, Director, Business Architecture & Analytics, at The University of Kansas Health Center, entitled, “How We Developed an Advanced Analytics Team to Solve Our Strategic Problems.”
Health systems have a wealth of data available, but often struggle with leveraging that data to solve strategic problems. A healthcare analytics team—made up of the right people with the right skills—can go a long way toward addressing organizational challenges and improving patient care. These analysts use advanced analytics to produce actionable insights, creating positive impacts throughout the organization.
This article will walk through the steps needed to put an effective applied analytics team in place.
Healthcare organizations often struggle with the time-value curve of data. The time it takes between a clinical event and being able to collect and use data to make and measure an improvement is far too long. Health systems can shorten the time-value curve of analytics with an applied healthcare analytics team. These trained analysts, working with the right tools, can get to actionable data faster, providing value in improved outcomes, operational efficiency, and the bottom line.
Organizations also face a data quotient problem. There is a vast amount of data available today, yet the data assets, data usage information, and people with data skills are often scattered throughout an organization and aren’t aligned strategically.
While healthcare organizations can often collect needed data without having a dedicated analytics team, the process is slow, inefficient, and difficult to manage. A dedicated team, with the support of key stakeholders, can focus on gathering accurate data more quickly and turning that data into insights that drive results.
Labor in any organization is a finite resource, and because data analytics can be time intensive, there is a limit to the data employees and consultants can process and report. In many healthcare organizations, much of data analysts’ time is spent managing reports, leaving little time for analysis and consulting. As required reporting volume grows, time for analysis shrinks, further compounding the problem. To identify solutions, organizations must understand the needs and limitations of processes in use. A current state assessment can reveal this information.
Conducting a current state assessment is vital for health systems challenged by collecting and using data effectively. An assessment highlights gaps in data analysis and provides insights into duplicative or inefficient processes. It might include looking at who collects and reports data, what tools they are using, and where the data comes from.
The next step is to identify solutions to challenges uncovered during the current state assessment. For example, if the organizational goal is to become more efficient and effective at gathering and reporting data, leaders must find a way to change the productivity curve. How can they decrease the time it takes to report data while increasing the time available to analyze the data for actionable insights?
To answer this question, leaders should map out requirements for a viable solution. This might look like the following list of requirements:
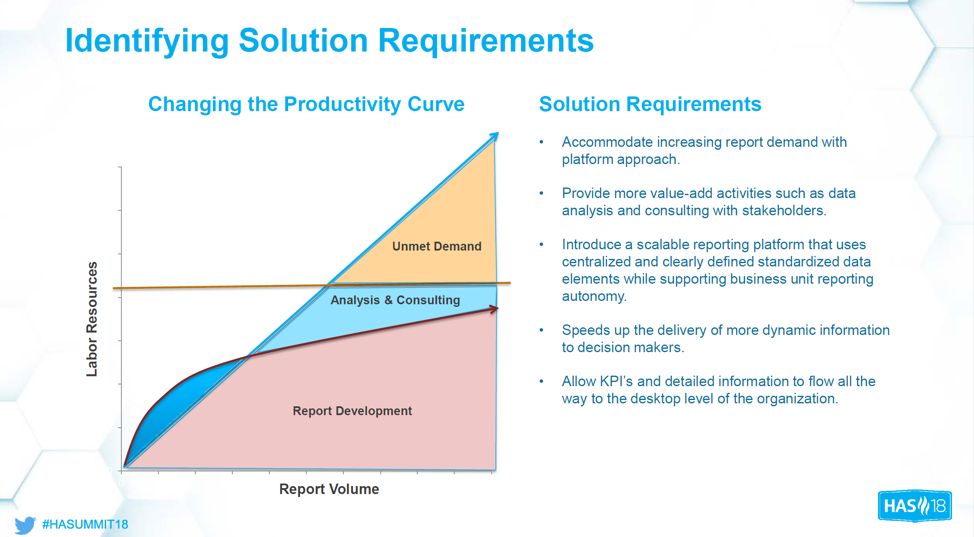
Figure 1 shows that report development takes up most of an analyst’s time, which leaves little time for analysis and consulting. Because labor is limited, as report volume increases, the unmet demand for analysts’ time increases. Automating reports changes the productivity curve. If analysts could significantly reduce time spent developing reports, they could add more value to the organization doing what they’re trained to do—analyze data and provide insights from that analysis.
Once the organization’s challenges and potential solutions are mapped out, it’s time to get buy-in about how to get from the current state to a future, desired state. To do this, organizations must look at both people and tools and invest in team members to prepare them for the task.
A frequent debate when building a healthcare analytics team is whether or not to have a centralized approach. Instead, it may better serve the organization to decide the best approach from a cultural standpoint and think more about the technical architecture of the team. This might include looking at what skills will be needed on the team and then deciding how to organize those people. A skills assessment provides data about whether current staff have or can quickly be trained in the skills necessary to produce actionable knowledge. Not every team member must possess each skill, but there are several skills the team, as a whole, must have to be successful.
Below is a sample list of foundational skills to include in a skills assessment:
An analytics team must have many of these foundational skills and know how to apply them in order to provide efficient and effective data analysis. Once the team is up and running, the organization might later decide to add additional specialty skills to the team, either through training, hiring, or contracting.
Having effective tools is also imperative. Not all data analysis software is created equal, so it’s important to have the right technology. Technology needs vary from organization to organization, but ideally organizations invest in a comprehensive solution with a variety of tools that will help speed the variety of tasks analysts spend the bulk of their time doing. An organization might spend a billion dollars on technology and building out a pristine data analytic platform, but this does nothing if the organization doesn’t have the right people to drive insights, and ultimately improvements. Neither people nor tools alone will do the job. Technology is vital to improving efficiency and accuracy of data reporting, and so is having the right people on board.
Developing an effective healthcare analytics team takes forethought and planning. Many organizations use a phased approach when building a team of analysts who are ready and able to solve the most pressing strategic problems. This might include the following three phases:

A roadmap is a guiding document that clearly lays out where an organization is and where it’s going, along with the concrete steps to get there. Part of building a roadmap involves introspection and organizational analysis. To do this, organizations need to take a three-step approach:
Getting leadership buy-in to invest in an applied healthcare analytics team requires a clear, concise message. Data is an asset. That’s a given in any healthcare organization. Most health system leaders will agree that analyzing data is critical—and that data analysis is a supporting function of strategy. So, the key to getting leadership on board to invest in an analytics team may require illustrating how to turn data analysis into a function of competitive advantage rather than just a supporting service.
This is challenging, however, if leadership regularly makes decisions based on the available data or even gut intuition. To meet that challenge, the project leader should make this pitch: The benefit of a data analytics team is that analysts will take data and, as quickly as possible, develop information from that data. They will then share what they’ve learned with operational leads who can translate that information into actionable insights. It’s these insights that have an immediate, measurable impact. The pitch should also highlight the competitive advantage of a dedicated healthcare analytics team. If the analytics team can do this work better and faster than the competition, what was once believed to be a support service can become a competitive advantage.
Once there is leadership buy-in, the next step is to put the roadmap into action. There are three general steps to building an analytics team:
Organizations that take time to ensure the team is asking the right questions to solve the right problems tend to have better results. Zeroing in on what those questions are takes a clear understanding of operations and outcomes. Knowing the biggest challenges and identifying solutions moves the roadmap from theory into action.
Limited resources can make building an analytics team challenging, but it can be done. Using available resources rather than having to get additional budget approval can make the process of building the team more efficient. And, any team or process that adds value without increasing expenditures is more likely to get buy in.
Finding space for the analytics team to operate can also be challenging. If office space isn’t available, look for alternative locations to set up computer stations.
When these goals have been accomplished, the healthcare analytics team can start doing what they were created to do—analyzing data to create actionable insights that can lead to improved processes, care, and outcomes.
Data is power, and to unleash that power, healthcare organizations need trained analysts, the right tools for the job, and to carefully consider the necessary steps to success. The first step is to think it through. Real, measurable change can happen when all foundational work has been done. The next step is to develop a plan that uses an organization’s unique culture and situation as a guide. Every organization is different, so there is no one “right” way to build and utilize an analytics team. Once stakeholders agree which strategic problems to tackle first and understand how an applied analytics team will drive change, the team can get to work. Finally, it’s important to remember the why.
Thoughtfully building a roadmap and following it gives the applied analytics team—and the data—the ability to shine. A qualified, dedicated team of analysts can provide actionable knowledge to inform quality initiatives that will positively affect patient care and the patient experience.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download this presentation highlighting the key main points.
Click Here to Download the Slides
https://www.slideshare.net/slideshow/embed_code/key/g5cCRi38ddi5nX