As healthcare systems are pressured to cut costs and still provide high-quality care, they will need to look across the care continuum for answers, reduce variation in care, and look to emerging technologies. This article walks through how to evaluate the safety and effectiveness and of emerging healthcare technology and prioritize high-impact improvement projects using a robust data analytics platform. Topics covered include:
• The importance of identifying variation in innovation.
• Ways to improve outcomes and decrease costs.
• The value of an analytics platform.
• The reliable information that produce sparks for innovation.
• Identifying and evaluating emerging healthcare technology.
• Knowing what data to use.
• The difference between efficacy and effectiveness in evaluation of emerging healthcare technology.
 Download
Download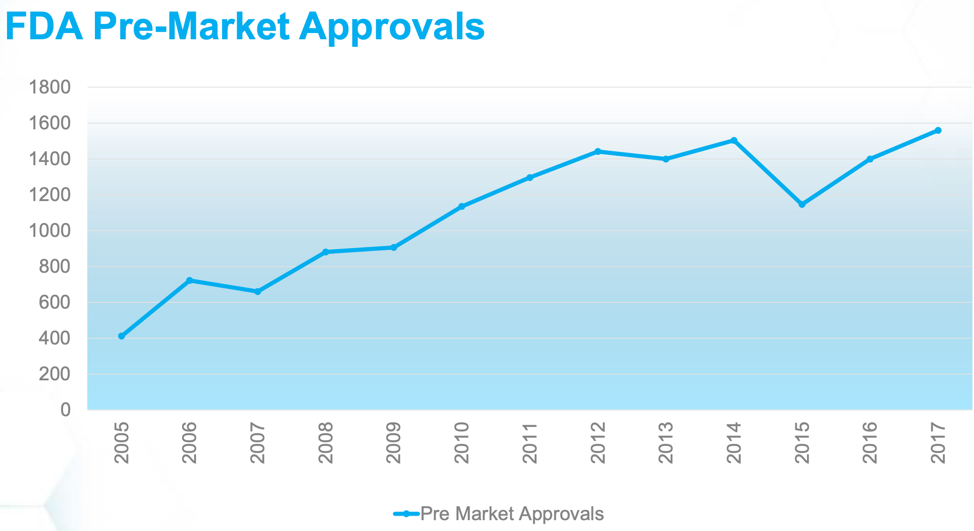

This report is based on a 2018 Healthcare Analytics Summit presentation entitled, “Innovative Analytics: Using Analytics to Evaluate Emerging Technologies.”
U.S. healthcare spending alone is larger than the gross domestic product of most nations. Total health spending in the U.S. was $3.5 trillion in 2017 and is projected to grow by an average of 5.5 percent annually from 2017 to 2026. If all U.S. healthcare spending was separated into its own sovereign nation, it would constitute the fifth largest economy in the world. Much of those healthcare dollars is spent on the costs of cardiovascular disease, which surpassed both Alzheimer’s disease and diabetes with a cost of $318 billion in 2015. That number is projected to more than double to $749 billion in 2035. Additionally, consumers and providers are not experiencing a great return on investment in healthcare dollars. In fact, life expectancy in the U.S. does not compare favorably to other countries which spend less per capita on healthcare.
These skyrocketing costs have a big impact on consumers, with premiums increasing by 74 percent from 2007 to 2017. During that same period, employer contributions increased by an average of 48 percent. The impacts are also being felt by hospitals and providers. In 2016, 30 percent of all Medicare fee-for-service patients were part of alternative payment models; that number rose to 50 percent in 2018. As healthcare systems are squeezed in all directions, they need to determine how to cut costs and still provide high-quality care. To do so, they will need to look across the care continuum for answers, eliminate silos, reduce variation in care, and look to emerging technologies.
There are two types of variation in healthcare: necessary and unnecessary. Necessary variation is deviation from standardized care based on individual patient characteristics resulting in improved outcomes. Unnecessary variation does not result in a benefit to the patient and instead increases cost. Variation in practice patterns has been studied in multiple conditions and the conclusion is that higher cost regions are not associated with improved quality or outcomes. While health systems have to look at variation in care in order to reduce unwanted variation, they can look within their own four walls to gain insights from data in order to reduce costs and improve care.
Health systems have struggled to answer the question of how to improve outcomes and decrease costs. New solutions are needed to answer an old problem. Healthcare systems can focus on these four pillars of healthcare improvement:
As emerging healthcare technology comes into greater focus, it’s important for healthcare systems to evaluate the safety and effectiveness in order to effectively harness new technology for better care and reduced costs.
Optimizing Care Across the Cardiovascular Continuum
Additionally, in looking for the highest impact projects to tackle, health systems can look to optimize care across the cardiovascular continuum:
To do all of these things effectively, healthcare systems need a robust analytics platform. In order to gain deep insights about the organization, its patients, and areas to maximize improvement, healthcare systems need a powerful analytics platform that brings data from many sources into a single source of truth. This allows an improvement team to evaluate the care that’s being provided, the impact on outcomes, and the impact on the cost of care. Once all the data is gathered, the next step is to decide what information to focus on.
Once health systems have all the data they need brought together in an analytics platform, they need to decide what information to focus on. Assembling an improvement team is necessary to evaluate and assess ideas for improvement work. There are many great sources of information that spark ideas and excitement once improvement teams begin their work. These could include:
Sparks for improvement ideas can also come from looking at processes, such as ideation sessions with subject matter experts, process mapping, or operational analysis. The more improvement teams begin to identify gaps in care, unintended variation, and other high-impact improvements that can be made, the more clinicians, frontline leaders, and staff begin to engage in the process and put forth new and higher quality ideas. As the permeation of quality increases, so do the quality and quantity of new sparks.
In particular, health systems should identify ideas related to emerging healthcare technology. So, how or where can a health system identify these sparks? While ideas are everywhere, some great places to identify potential ideas related to new technology might include supply chain or operations, cost analyses, or physician and staff questions.
Improvement teams need to begin by asking, “What data should be used?” The roadmap of an improvement journey begins there and then might take the following path by answering each of the questions or following the steps below:
At this point in the data journey, the improvement team may take these results back to the subject matter experts and find out if the results make sense, if there are obvious gaps, etc. The goal is to then have data that is valuable in terms of analytical output and valuable to providers in informing clinical decision-making.
Technological improvements in healthcare have saved many lives and improved the quality of life for even more. Technology changed experiences for patients and families and impacted medical processes and the practices of healthcare professionals. However, there are so many new medical devices and other technologies entering the healthcare space that health systems and providers need to exercise caution and thoroughly evaluate the safety and effectiveness of new technologies before implementation. It’s important to strike the right balance between efficacy and effectiveness in the evaluation of emerging healthcare technology. The graph below shows the drastic increase in FDA Pre-Market Approvals of medical devices and reinforces the need for evaluation.

It can be difficult to strike this balance as many medical professionals are looking for the next shiny, new thing. Health systems have to be able to differentiate between case studies in specific segmented populations versus the real-world implementation of new technologies. In practice, most patient populations are heterogenous and differ greatly from the homogeneous patient population where testing of new technology occurs. The overarching problem in moving from efficacy to effectiveness is understanding what new therapies or devices will truly support the mission of providing better quality care, better outcomes and lower costs. Oftentimes, new technologies, when placed into real-world settings, will end up being very costly and may not provide any additional benefits for patients.
Improvement teams can learn the following valuable lessons for evaluating emerging healthcare technology:
While healthcare technology continues to advance rapidly, sound assessment with non-homogenous patient populations lags significantly behind. Ultimately, health systems need to be able to make their own decisions regarding implementation of emerging healthcare technology and other high-impact projects. Doing so requires a robust analytics platform.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download the presentation highlighting the key main points.
Click Here to Download the Slides
https://www.slideshare.net/slideshow/embed_code/key/3mmxUN0TzrRJyF