Health system resource strain became an urgent concern early in the COVID-19 pandemic. Hard-hit areas exhausted their hospital beds, ventilators, personal protective equipment, staffing, and other life-saving essentials, while other regions scrambled to prepare for inevitable surges.
These resource concerns heightened the need for accurate, localized hospital capacity planning. With additional waves of infection in the summer months following the initial spring 2020 crisis, health systems must continue to forecast resource demands for the foreseeable future.
An accurate capacity planning tool uses population demographics, governmental policies, local culture, and the physical environment to predict healthcare resource needs and help health systems prepare for surges in patient demand.
 Download
Download

Health systems use capacity planning methods to balance the availability of beds, staff, and other resources with patient demand. Planning for annual surges in volume (e.g., flu season) is difficult, given uncertainty about timing and duration, but the unprecedented scale of the COVID-19 pandemic has far exceeded the worst surges. COVID-19 spread and severity have proven variable over time and place, leading to demand spikes and empty beds.
A variety of factors, including population demographics, governmental policies, local culture, and the physical environment, have shaped COVID-19 demand for healthcare resources. As regions around the world have been struggling to obtain sufficient beds, staff, and equipment during the pandemic, advanced analytics-driven capacity planning has emerged as a healthcare must-have.
Capacity forecasting provides critical insight into when a patient surge will occur and if/when demand will exhaust resources. This foresight allows planners to design and implement mitigation strategies that can prevent disastrous pandemic resource strain, like those in Italy and New York City in the spring of 2020 and Florida, Texas, and Arizona in the summer of 2020. Meanwhile, overestimating demand can be dangerous to the financial viability of these same care delivery organizations. Although national and regional outbreak forecasts exist, hospital leaders need projections that incorporate local dynamics, their expert knowledge, and risk tolerance.
In choosing a capacity planning model, organizations can’t afford to waste valuable discussion time debating model methodology, which is likely with black box or proprietary models. Using a transparent capacity planning tool from an established analytics partner, such as Health Catalyst, promises more efficient, accurate outcomes. Health Catalyst initially built its COVID-19 Capacity Planning Tool on the well-regarded, open-source COVID-19 Hospital Impact Model for Epidemics (CHIME) application from Penn Medicine.
Is your health system planning for a resurgence of COVID-19 cases?
Utilize our free online Capacity Planning Tool to forecast local demand on system capacity, supplies, staffing—and more.
START USING THE CAPACITY PLANNING TOOL
At the beginning of the pandemic, health systems forecasted the need for patient beds, staff, and supplies using the standard SIR model for infectious disease. Users could adjust the model at a single point in time to account for the impact of mitigation policies, such as social distancing. But the required assumptions for accurate adjustment were often unknowable or more dynamic. Even the most sophisticated models predicted patient volumes and deaths that disease spread rapidly proved wrong.
As more data became available from sources such as the New York Times and the U.S. Census, Health Catalyst added the ability to leverage empirical forecasting with well-documented methods from the fields of microbiology and epidemiology and implemented the open-source statistical computing package R. As a result, Health Catalyst makes increasing data and model sophistication available through a simple, transparent interface healthcare planners can easily leverage. These design decisions have led to increased credibility in the broader healthcare community and kept conversations focused on decisions and action.
COVID-19 spread rates have progressed differently over place and time. In the five sample regions in the animation below, black points indicate data used in generating the forecast, grey points indicate actual counts held out from the forecast, and the yellow rectangle shows the next 30 days. The colored lines show the forecast using the measures of spread (reproduction number versus doubling time) and forecast techniques (e.g., linear versus spline) that worked best for each region.
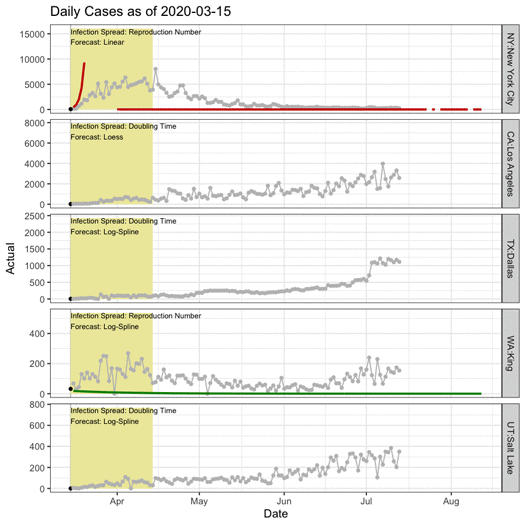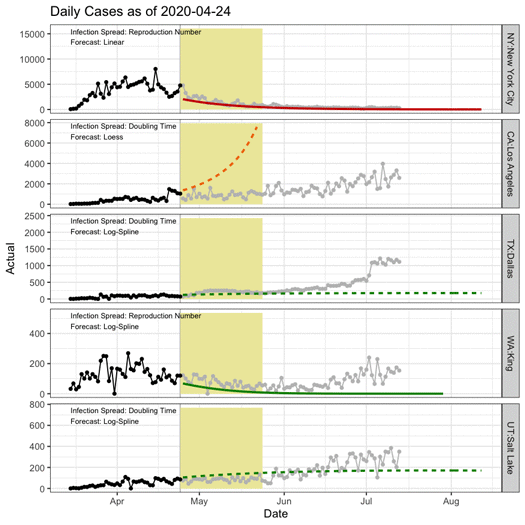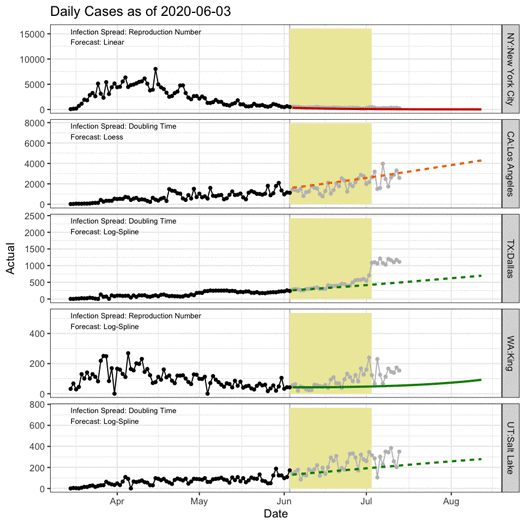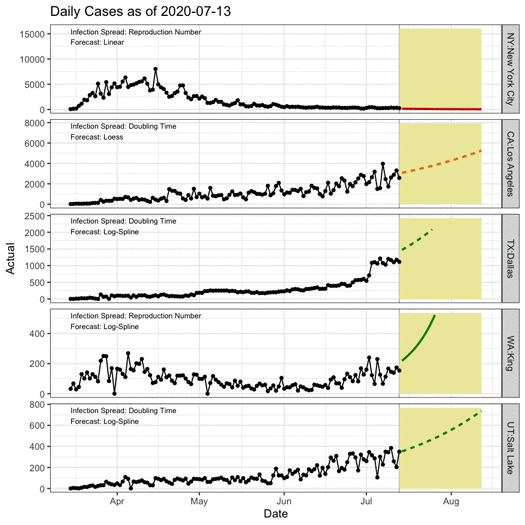
Rapidly changing conditions that place limits on social interaction, travel, and business operations can hamper the accuracy of outbreak forecasts. A capacity planning tool aims to buy leadership time to act. Organizations should adjust model inputs to reflect different pandemic scenarios, given the high level of uncertainty in how the population will react to the virus. For example, quick adoption of travel restrictions and social distancing policies initially slowed viral spread and evaded a dramatic patient surge in some areas. As restrictions have been differentially enforced or lifted, however, spread keeps changing.
An accurate capacity planning tool supports timely action with its ability to manage, use, and save scenarios. The ability to easily compare a variety of situations gives a better picture of uncertainty around resource availability and provides more support to mitigation efforts.
Capacity planning usually occurs at a regional level based on the hospital’s market share and utilization patterns. Given differences in population densities and changing social distancing restrictions between regions, suitable mitigation strategies will vary between hospitals.
Some organizations have been surprised to find they cannot reliably estimate market share and thus alter this parameter during scenario modeling. Cultural factors can shape market share, such as when a patient feels more comfortable presenting at an academic medical center over a community hospital (even if they lack objective evidence to support this preference).
As well, hospital utilization patterns have changed. Examples include pausing non-emergent services and shifting labor and delivery services to ambulatory surgical centers. Some hospitals are working with local and more distant skilled nursing facilities as a place for COVID-19 patients to convalesce once out of intensive care.
One unexpected silver lining of the COVID-19 crisis has been the willingness of healthcare executive culture to embrace data science to support its decisions. Many data science applications exist at the point of care or service to support individual providers and patients, but engaging health system leadership in data science has been more challenging. The deployment of advanced analytics for capacity planning is a rare opportunity to directly influence executives and strategic planners to likewise work in a data-driven way.
While governmental policies initially slowed the spread of COVID-19 to prevent dramatic patient surges in many areas, as regions have reopened during the summer months, infection rates have again risen. Hospital leadership will need to monitor forecasts for some time, particularly as fall and winter approach. An effective capacity planning tool must leverage robust data and advanced analytics in the face of shifting circumstances. Such a solution will provide valuable insights into several possible futures and gift healthcare leaders and managers with the time to anticipate the necessary resources to keep communities healthy.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download the presentation highlighting the key main points.