While most consumer-oriented industries have turned to mobile-first, cloud-based platforms for consumer interaction, healthcare lags behind in digitization, particularly when it comes to self-service consumer engagement. As digital consumer interaction increasingly drives enterprise success, healthcare must join the modern digital playing field. To get there, organizations need to establish digital investment and enablement frameworks and can then follow five strategies for stable, scalable transformation:
1. Formally define “digital” for the organization.
2. Follow 10 guiding principles to support digital.
3. Divide technology into appropriate portfolios.
4. Develop an analogy to explain the integrated portfolio approach.
5. Strategically select vendor partners.
 Download
Download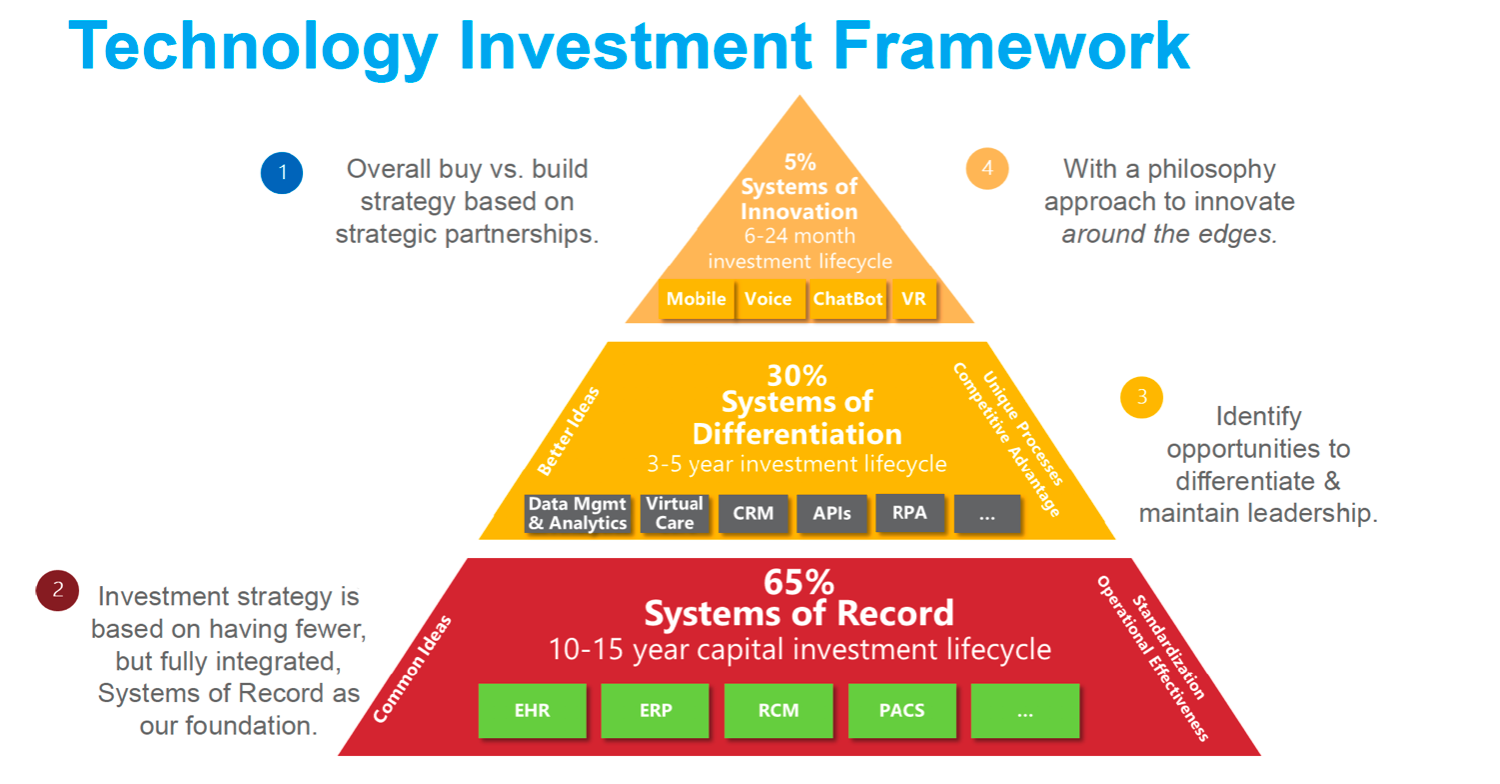

From planning travel to buying groceries, today’s consumers are making more transactions digitally. Yet, as consumer-oriented industries overall turn to mobile-first, cloud-based platforms as their primary, and sometimes only, means of consumer interaction and engagement, healthcare lags behind. Healthcare digitization remains EHR centric and relies on a vendor approach to apps, resulting in a fragmented experience, poor data integration, and non-intuitive tools that too often fail to drive informed decisions or customer value.
This digital lag puts healthcare at risk in an evolving consumer landscape in which digitization increasingly drives success and failure. Even brands with business models that predate digitization, such as Delta Air Lines, have had to disrupt themselves and transform to consumer self-service models to stay relevant as digitization steadily gains influence over consumer experience and loyalty. It’s now imperative that healthcare catches up with digital consumer-oriented trends and expectations.
To get on the modern digital playing field, healthcare organizations can follow a basic digital transformation roadmap and customize it to serve each health system’s unique and complex needs. With an effective digital framework, providers and the right vendor partners fully integrate data, technology, and reimagined workflows. Health systems address optimal user experience while providing virtual access to all relevant information in an interactive, self-service environment that’s always available, from any device.
For effective transformation, a healthcare digitization framework supports four central goals:
Meeting the goals of the digitization framework requires health systems to rethink how they invest in technology. Current healthcare technology spending models can allocate up to 90 percent of their non-labor costs to maintaining and supporting systems of record (e.g., EHRs, enterprise resource planning, revenue cycle management, and more); these models need to evolve to allow strategic growth in consumer-facing areas (e.g., mobile, voice, chatbot, and virtual reality).
An effective system of record investment, that supports consumer-centric digitization, should more optimally be managed around 65 percent (Figure 1). To support this 65 percent systems-of-record investment goal, organizations must adopt an overall buy-versus-build strategy based on strategic partnerships (putting responsibility on those partners to figure out system integration) and an investment strategy based on having fewer, but fully integrated, systems of record as the foundation.

Then, working up the framework, health systems identify opportunities to differentiate and maintain leadership, maintaining an approach to innovate “around the edges” rather than building or customizing the foundational systems. The technology investment framework in Figure 1 shows how organizations can save money at the lower level (systems of record) to allow for investment at the center and top of the pyramid—the systems of differentiation and innovation, which will generate opportunities and with which consumers will engage directly.
Furthermore, technology lifecycles align with the above investment framework as longer lifecycles at the bottom of the framework correspond with heavier, capital intensive investments; the middle of the framework focuses more around SaaS-enabled cloud solutions in a subscription-based model; while the top of the framework follows a very short lifecycle, allowing organizations to rapidly test which consumer-oriented tools and services are effective and continually update those tools to meet rapidly evolving innovation cycles.
Once health systems have redefined their technology investment framework, they need a roadmap for digital transformation. A digital enablement framework (Figure 2) layers systems of differentiation and innovation (application interface, digital process, API/event gateway, and data operating system layers) on top of other data sources, systems of record, and internet of things (sensors, monitors, consumer devices, etc.), which all rests on the IT infrastructure layer (cloud, networking, directories, data centers, etc.).
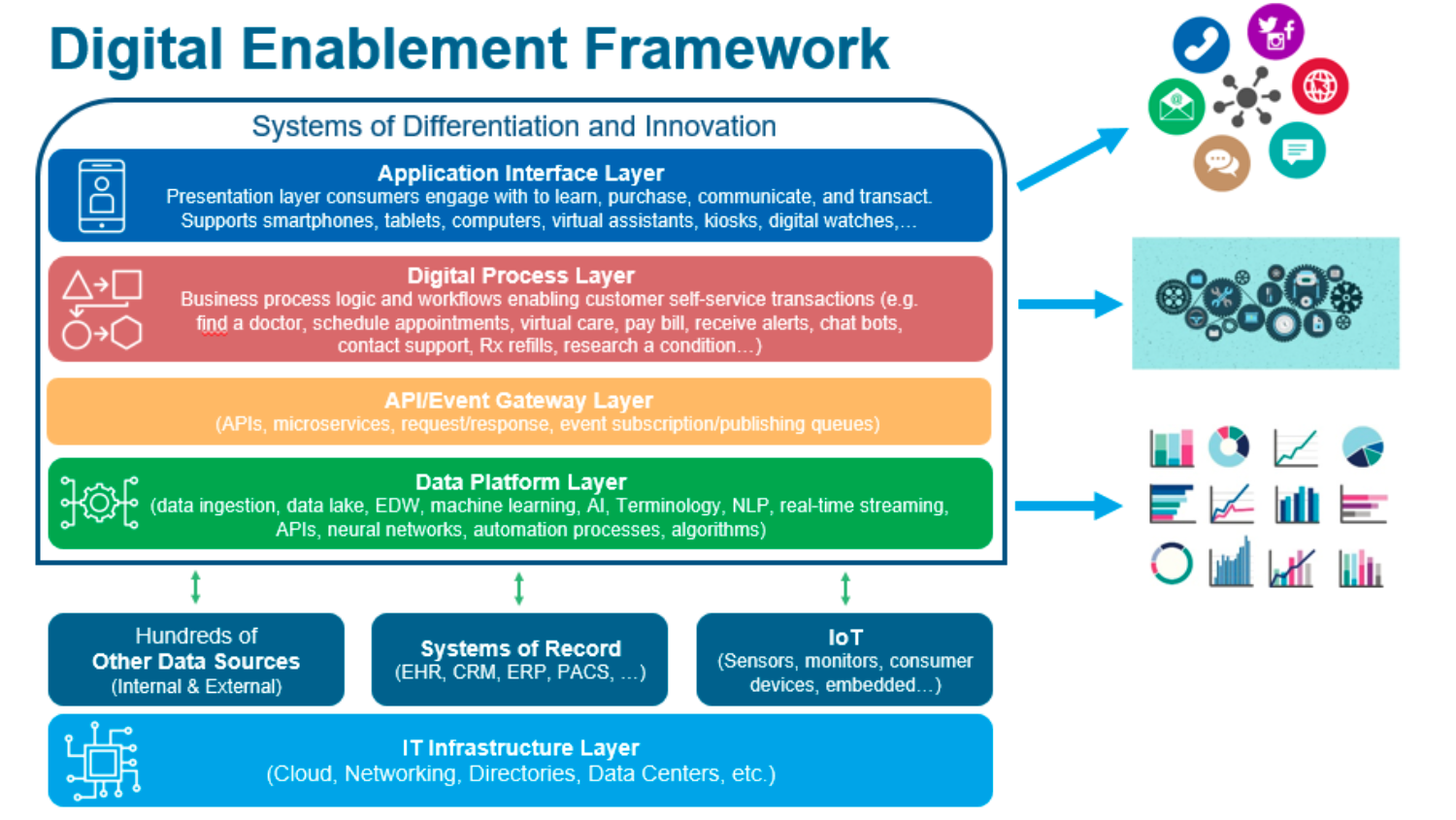
This framework allows organizations to make conscientious decisions about systems of differentiation and innovation at the top layers, as well at the data platform layer (e.g., the Health Catalyst® Data Operating System [DOS™]) to support digital process and application interface layers. This allows organizations to build fully integrated, consumer-centric digital interactions based on consumer perspectives, rather than just offering consumers a myriad of non-integrated, vendor-specific digital tools lacking cohesiveness.
Following the establishment of the digital investment and enablement frameworks, organizations can start their digital transformation. A holistic approach supports digitization from the ground up with four strategies that guide stable, scalable transformation:
An effective definition of digital includes the innovative meshing of new technologies, data intelligence, re-imagined workflows, and organizational leadership—all aligned to achieve a “sticky” and optimal experience that invites end users to virtually access all relevant information while offering a breadth of interactive self-service capabilities.
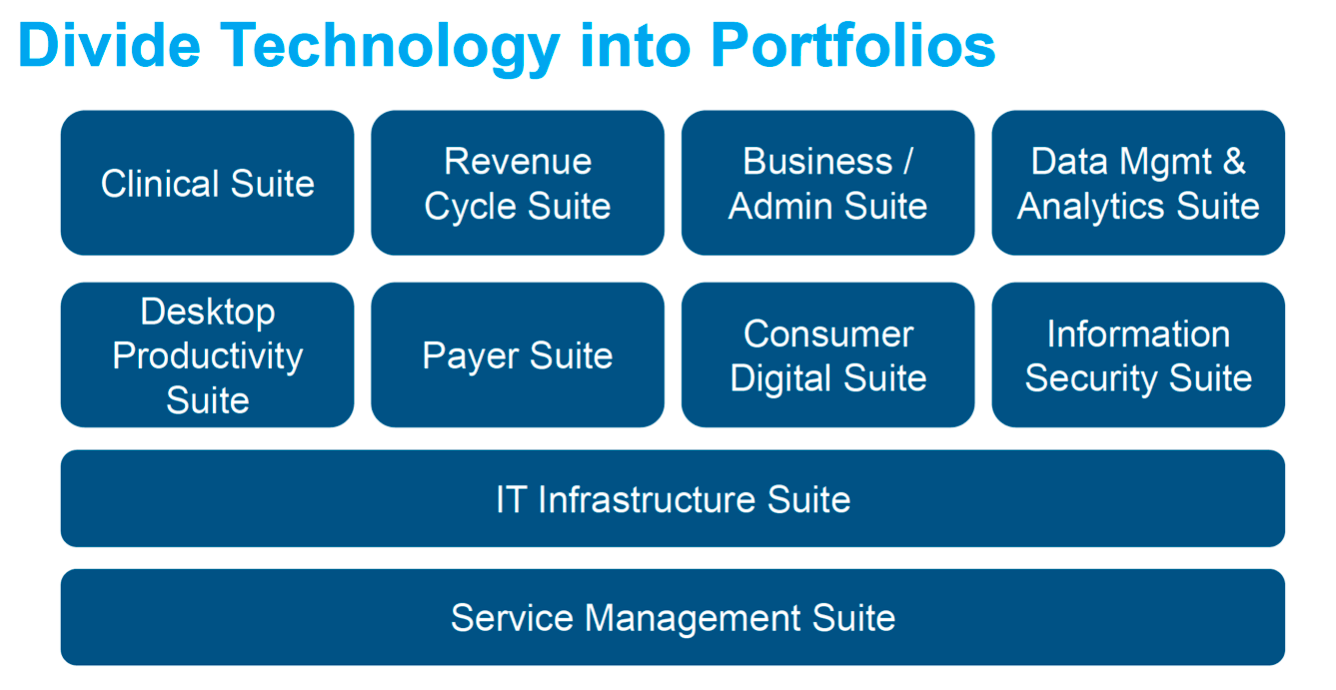
Health systems create 10 portfolio areas (Figure 3) for laser focus around strategy for each area, all governed to support end digitization goals. Build business-driven IT partnerships for each portfolio and each major IT investment with a clinical or business sponsor/champion, who is the face of the initiative, paired with IT champion who’s doing the bulk of work behind the scenes. The partnership allows for two “harmonized” voices on the leadership team and ensures IT and business goals are connected.
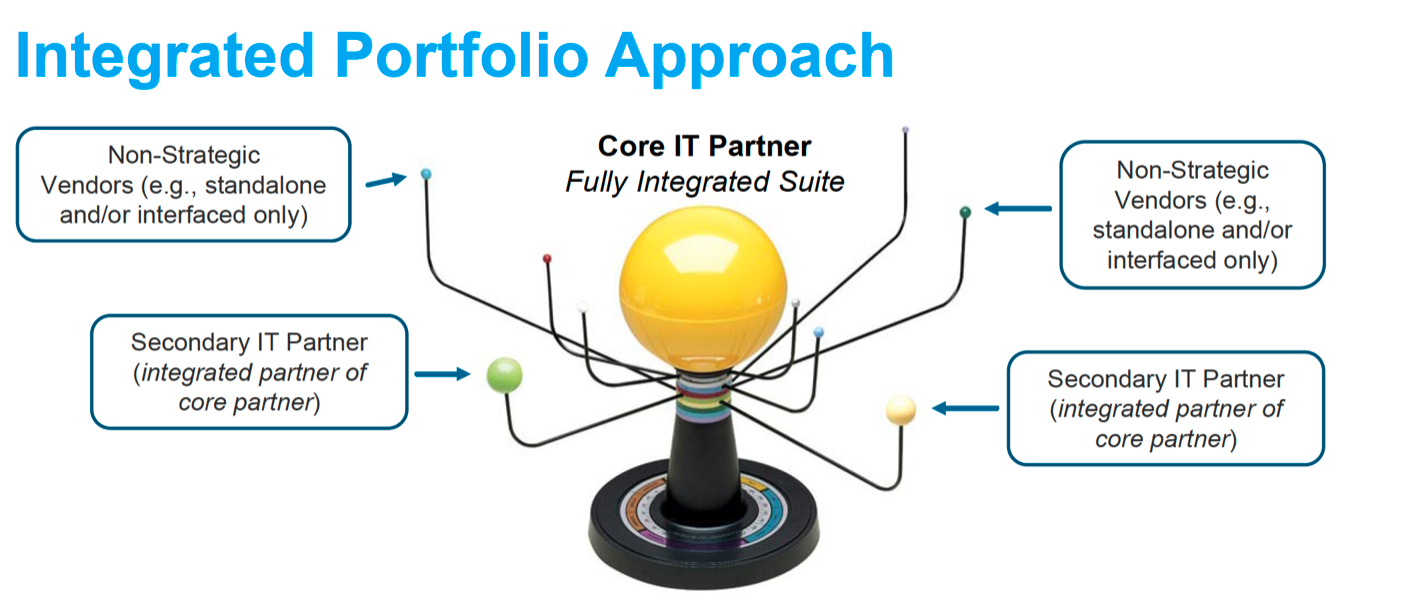
An analogy can make the integrated portfolio approach above more understandable to leadership. One possible approach, as shown in Figure 4, uses a solar system to represent the relationships between the primary vendor partner for a given portfolio (the sun), secondary vendors (e.g., fully integrated partners of the primary partner), and non-strategic vendors (e.g., interfaced vendors) in its orbit.
This “best of suite” approach by portfolio results in far fewer vendors with much higher levels of integration, which both supports reducing systems of record costs while providing significantly higher levels of integrated capabilities and access to data—key enablers of the digital framework.
A vendor-partner (versus a vendor-only relationship) maintains a mindset that they and the organization win or lose together. This relationship operates on trust and respect, keeps a long-term (versus sales) focus, enters into mutual risk sharing, supports the growth of both businesses, pursues co-development initiatives, and earns high levels of executive sponsorship.
Other service industries have set a standard for digitization that comprises key attributes, including mobile-first and cloud-based platforms, a cohesive and brand-driven (versus vendor-driven) user experience, and analytics-driven personalization of the digital experience while delivering substantial consumer value. As consumers increasingly interact according to these standards and base brand choice and loyalty on the quality of their digital interactions, healthcare must adopt the digital priorities and expectations that increasingly define consumer-oriented industries. Retail, travel, food service brands, and more have defined the modern digital playing field and given healthcare the roadmap it needs to join them.
Would you like to learn more about this topic? Here are some articles we suggest:
Would you like to use or share these concepts? Download the presentation highlighting the key main points.