Using Data-Driven Insights to Improve Practice Management

- All leaders have on-demand access to performance data at multiple levels from the organization-wide down to the patient and provider level.
- Senior leaders are making data-driven decisions for strategic responses across John Muir Health to shifts in market, growth opportunities, and emerging markets.
- The regional management teams are using the application to inform:
- Daily operations.
- Encounter processing.
- Patient access.
- Budget variances.
By leveraging these new capabilities, John Muir Health has achieved:
- Transparency of the data and accountability of the regional management teams for key performance indicators.
- 14 percent improvement in completed physician encounters, resulting in faster revenue capture, when compared with the previous year.
- Eliminating the encounter-associated report backlog.
Effective practice management includes tracking and reporting patient outcomes, and effectively managing revenue cycle, as well as keeping an eye out for market changes and growth opportunities. Well-managed practices effectively balance supply and demand on a daily, weekly, and long-term basis, actively managing encounter volume, panel size and scope, timeliness of available appointments, and payer mix.
John Muir Health faced challenges in obtaining data that would provide leaders with strategic decision support information that fostered effective practice management. John Muir Health had attempted to use its EHR to obtain this information, but discovered it was unable to meet the complex demand. As a result, the organization relied on burdensome manual work processes, resulting in delays and a backlog of data requests, and limited ability to make well-informed, data-driven decisions.
After leveraging the information within its data warehouse and analytics platform to create a network leadership encounter application, John Muir Health acquired the following capabilities:
EVOLVING PHYSICIAN PRACTICE LANDSCAPE
The physician practice landscape is changing, with large numbers of physicians now employed by healthcare organizations. One factor contributing to the decrease in independent physician practices, and increases in the number of physicians employed by healthcare organizations, is the burden associated with managing a practice.1,2 In addition to tracking and reporting patient outcomes, and ensuring appropriate revenue cycle management, effective practice management requires organizations to effectively balance supply and demand on a daily, weekly, and long-term basis, actively managing encounter volume, panel size and scope, timeliness of available appointments, and payer mix.3
A leader in healthcare in the San Francisco Bay Area, John Muir Health is a not-for-profit integrated system of hospitals, outpatient centers and independent and foundation doctors that offer a full range of medical services. Within John Muir Health’s Physician Network, there are more than 300 foundation primary care and specialty physicians, physician assistants, and nurse practitioners. These physicians include pediatricians, family medicine practitioners, internal medicine physicians, cardiologists, and other specialists who provide services to John Muir Health patients.
THE CHALLENGE OF MANAGING WITH INCOMPLETE PRACTICE INFORMATION
John Muir Health is dedicated to the three-part aim of improving population and patient health, elevating the patient experience, and providing affordable care. It has demonstrated success in achieving goals to lower costs, enhance quality and service, and increase access.
Despite this dedication and demonstrated success, John Muir Health faced challenges in obtaining practice data that would support leaders, from the frontline staff to the c-suite, in effective practice management. Lack of an organization-wide view of data made it difficult to evaluate the impact of practice interventions on systemwide performance.
DEFINING THE SPECIFIC NEEDS AND USE CASES
Recognizing the opportunity to greatly improve practice management by providing better information to senior and operational leaders, John Muir Health engaged key stakeholders to analyze the situation further to identify and prioritize which data would provide the best strategic and actionable information. Their analysis uncovered the following insights.
Senior leadership’s need for integrated data
Incomplete data limited the Physician Network’s senior leadership team’s ability to make data-driven decisions. Across the entire organization, the total volume of encounters was not well understood or defined. This made it difficult to effectively explore growth opportunities such as opening additional clinics or services, reallocating physicians’ time, or evaluating opportunities in emerging markets. Decisions made without an organizational view could easily result in a change that helped an individual practice or region, but had a negative impact on the organization overall. Without integrated data, it was difficult for John Muir Health to develop a strategic plan that would support growth and maximize patient access, without unnecessary duplication of services.
Regional management team’s need for operational data
Regional Management teams did not have the information they needed to explain and understand budget variances, which hampered their ability to make insightful changes to daily operations that would effectively control costs, meet targeted revenue, and provide appropriate care for patients. To accomplish this goal, they determined that the solution must include performance metrics that provided the level of detail necessary to evaluate individual practice performance, including information on the drivers of performance and patient outcomes.
Practice managers were largely unable to efficiently manage encounter processing. Identifying how long an encounter had been open and if it needed follow up was a challenge. Encounters must be closed before billing can be completed, making an effective encounter closing process critical to revenue cycle and essential to avoid delays in coding, billing, and revenue capture. Also lacking was information regarding the distribution of new patients, a particularly important data point for ACO, and payer data by appointment.
ANALYTICS KEY TO PRACTICE MANAGEMENT IMPROVEMENT
John Muir Health had attempted to use the EHR to provide the data leaders required, but discovered the EHR was unable to meet the complexity of the demand. This led to a dependency upon burdensome manual work processes to get to the data, resulting in delays and a backlog of data requests. A flexible analytics solution was required that would provide access to the information leaders desired, enabling practice management improvement.
To execute its desired analytics strategy and provide the information it needed, John Muir Health selected and utilized the Health Catalyst® Analytics Platform, including the Late-Binding™ Data Warehouse and broad suite of analytics applications, and Health Catalyst’s Professional Services.
Bringing together disparate information
The analytics platform aggregates data from a wide variety of sources, including financial, supply chain, patient satisfaction, and other operational source systems’ data. John Muir Health relies upon this solution as its primary source for internal data. In addition to leveraging the suite of analytics applications, John Muir Health partnered with Health Catalyst Professional Services for training on visualization tools to accelerate the ability of its data analysts to independently develop applications, cultivating the capacity for the analysts to meet identified, and prioritized, organizational and business needs.
Using the analytics platform and the Subject Area Mart (SAM) Designer, John Muir Health developed a network leadership encounter dashboard to provide operational leaders access to information critical to practice management. The SAM Designer simplifies the process of pulling data out of source systems, which used to be a time-intensive, manual task that required substantial specialized IT knowledge. Now, the SAM Designer pulls relevant data into a data mart and filters out anything not needed. Analysts then run calculations on that data and create visualizations that reflect the results.
Dashboards for simple visualization
The network leadership team encounter dashboard (see Figure 1) includes critical information, easily visualizing this data, which can be filtered by criteria including location, department, manager, city, site, visit type, financial class, specialty, and provider. The analytic application supports drilling into the detail, all the way to the individual provider and patient level detail. Available data includes:
- Encounter statistics—information can be trended over time, compared to the last four years’ performance, and filtered to include all, new, or established patients.
- Payer mix—appointments and utilization can be viewed by financial class and payer.
- Open and closed encounter status—the number of days an encounter has been open is easy to see. The data is grouped by days, supporting the quick identification of outstanding encounters.
- Third next available appointment—it is now easy to visualize the average wait time for the third next available appointment, and the data can be filtered by specialty, site, department, and provider.
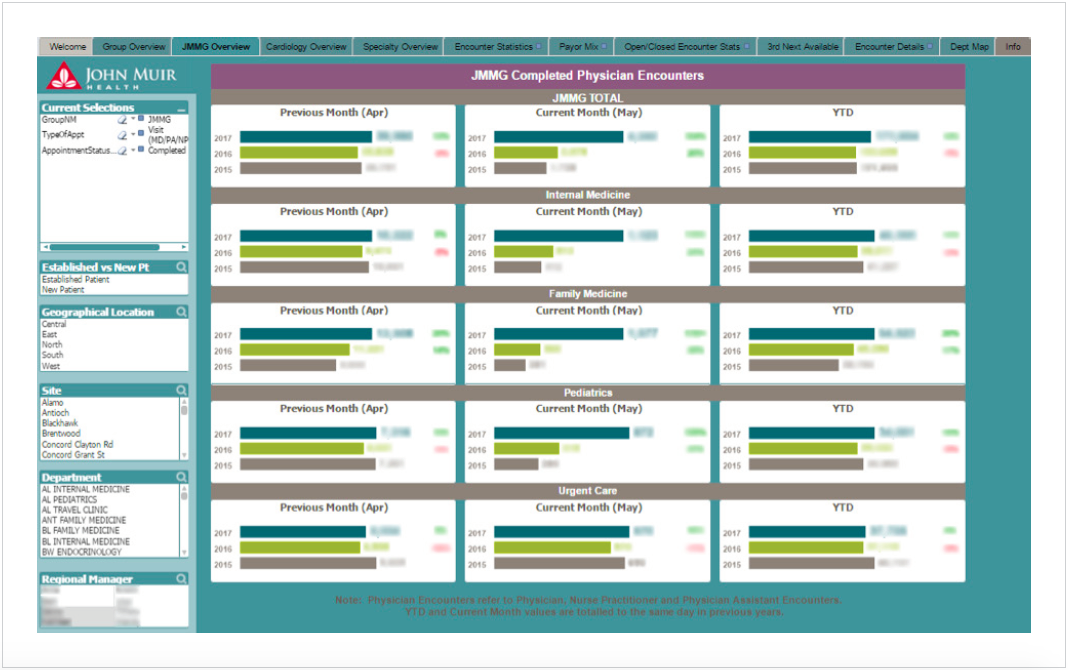
The analytics solution provided all of the information stakeholders had identified and prioritized as essential, and more. For the first time, operational leaders can take a data-driven approach to making strategic decisions, effectively balancing supply and demand, managing encounter volume and closure, ensuring timely revenue capture, timeliness of available appointments, and payer mix.
RESULTS
The network leadership encounter dashboard is used each day by the President and Chief Administrative Officer of the Physician Network and his direct reports, ensuring improved daily management of operations.
After leveraging the information within its data warehouse and analytics platform to create a network leadership encounter application, John Muir Health acquired the following capabilities:
- All leaders have on-demand access to performance data at multiple levels from the organization-wide down to the patient and provider level.
- Standardized data and definitions, and one source of truth.
- Senior leaders are making data-driven decisions for strategic responses across John Muir Health to shifts in market, growth opportunities, and emerging markets.
- The regional management teams are using the application to inform:
- Daily operations.
- Encounter processing.
- Patient access.
- Budget variances.
- By leveraging these new capabilities, John Muir Health has achieved:
- Transparency of the data and accountability of the regional management teams for key performance indicators.
- 14 percent improvement in completed physician encounters, resulting in faster revenue capture, when compared with the previous year.
- The visualizations in the application supported identification of outliers whose encounters were not closed in a timely manner. Leaders were able to follow up, providing additional support to ensure complete clinical documentation so the encounter could be closed.
- Reporting efficiencies through the analytic application.
- Previously, access to the data sources was limited to just a few people. Now, 77 different people use the application, providing immediate access to key performance data.
- Elimination of encounter-related report requests backlog and a substantial decrease in the number of ad hoc reports asked for each month due to improved data and access. Rather than spending all their time creating multiple versions of similar reports, analysts are able to use their time for more value-added work.
“Being able to access data in an efficient manner has allowed me and other leaders to make proactive changes rather than be reactive to situations. This has shifted our traditional, intuitive management style into a data-driven management style, and is making a difference in aligning staff, physicians, and others in decision making. I am very proud of the Physician Network’s adoption of this tool and feel that our team has become more sophisticated in our approach to managing this very important component of our health system.”
– Lee Huskins
President and CAO
John Muir Physician Network
WHAT’S NEXT
The leadership team plans to continue to use the analytic application to inform John Muir Health’s strategy, and make strategic and operational decisions. By following up on additional opportunities the application surfaces, John Muir Health will continue to improve the value and effectiveness of operations.
REFERENCES
- Singleton, T., & Miller, P. (2015). The physician employment trend: What you need to know. Family Practice Management, 22(4), 11-15.
- Page, L. (2016). Employed vs. self-employed physicians: Who’s happier? These are the tradeoffs. Medscape.
- Manage Variation in Demand. (n.d.) Institute for Healthcare Improvement.
ABOUT HEALTH CATALYST
Health Catalyst is a next-generation data, analytics, and decision support company committed to being a catalyst for massive, sustained improvements in healthcare outcomes. We are the leaders in a new era of advanced predictive analytics for population health and value-based care. With a suite of machine learning-driven solutions, decades of outcomes-improvement expertise, and an unparalleled ability to integrate data from across the healthcare ecosystem. Our proven data warehousing and analytics platform helps improve quality, add efficiency and lower costs in support of more than 85 million patients and growing, ranging from the largest US health system to forward-thinking physician practices. Our technology and professional services can help you keep patients engaged and healthy in their homes and workplaces, and we can help you optimize care delivery to those patients when it becomes necessary. We are grateful to be recognized by Fortune, Gallup, Glassdoor, Modern Healthcare and a host of others as a Best Place to Work in technology and healthcare.
Visit www.healthcatalyst.com, and follow us on Twitter, LinkedIn, and Facebook.
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.