Trauma Program Analytics Improves Emergency Department Throughput

- 21 percent relative reduction in ED LOS for patients ages zero to 17.
- 19.2 percent relative reduction in ED LOS for patients ages 18 to 64.
- 11.9 percent relative reduction in ED LOS for patients over age 65.
To leverage data from its trauma registry database to improve patient outcomes, Mission Health utilized its data platform and analytics, providing real-time access to data and a more comprehensive understanding of each trauma case. With an analytics-driven approach, Mission reduced emergency department (ED) length of stay (LOS) for patients with Level II trauma activation across its populations.
TRAUMA TEAM ARRIVAL TIME IS KEY TO LOWER MORBIDITY AND MORTALITY
As the leading cause of death for individuals up to the age of 45 and the fourth leading cause overall for all ages, trauma significantly impacts patient populations. Patients with serious traumatic injuries, however, who receive timely care at a designated trauma center have lower morbidity and mortality.1,2
One of the nation’s leading providers of healthcare services, HCA Healthcare is made up of locally managed facilities that include 185 hospitals and 119 freestanding surgery centers located in 21 U.S. states and in the United Kingdom. Mission Health, an operating division of HCA, based in Asheville, North Carolina, is the state’s sixth-largest health system and includes six hospitals, numerous outpatient and surgery centers, post-acute care provider CarePartners, and the long-term acute care provider Asheville Specialty Hospital. It also has the region’s only dedicated Level II trauma center, Mission Hospital, which provides care to over 3,500 trauma registry patients annually.
IMPROVEMENT REQUIRES TIMELY, MEANINGFUL DATA
Mission’s trauma program had access to a voluminous amount of data—over 500 data points on every patient for more than 3,500 trauma admissions annually. However, despite access to a trauma registry database with an overwhelming amount of information, the health system was unable to obtain timely, meaningful data it could use to drive improvements. Previously, Mission had collected data from the EMR by completing manual chart reviews or via an IT request for a report. Writing the report often took weeks, plus additional time to validate data. The trauma team often had to wait months for the data it requested. With the delay, the trauma team ended up using retrospective data for improvement, rather than realtime data, limiting the effectiveness of improvement efforts.
To improve patient outcomes, Mission needed an analytics solution to visualize the data in a way that would effectively and efficiently help the health system better understand its performance and enable ongoing process improvement.
IMMEDIATE ACCESS TO REAL-TIME TRAUMA DATA IDENTIFIES IMPROVEMENT OPPORTUNITIES
To better visualize its data, Mission leveraged the Health Catalyst® Data Operating System (DOS™) and a robust suite of analytics applications, including a Trauma Advanced Analytics Accelerator. The Trauma Advanced Analytics Accelerator provides immediate, easy access to data real time, including data that had not been captured previously. The trauma program, and providers involved in the care of trauma patients, can access detailed trauma program data, including trauma type, arrival location, trauma team time to arrival, process measures like use of the standard order set, aggregate and patient level process, and outcome measures by injury type (see Figure 1). With improved access to robust data and analytics, the trauma program can focus on using the aggregated and detailed data to improve work processes and patient care.
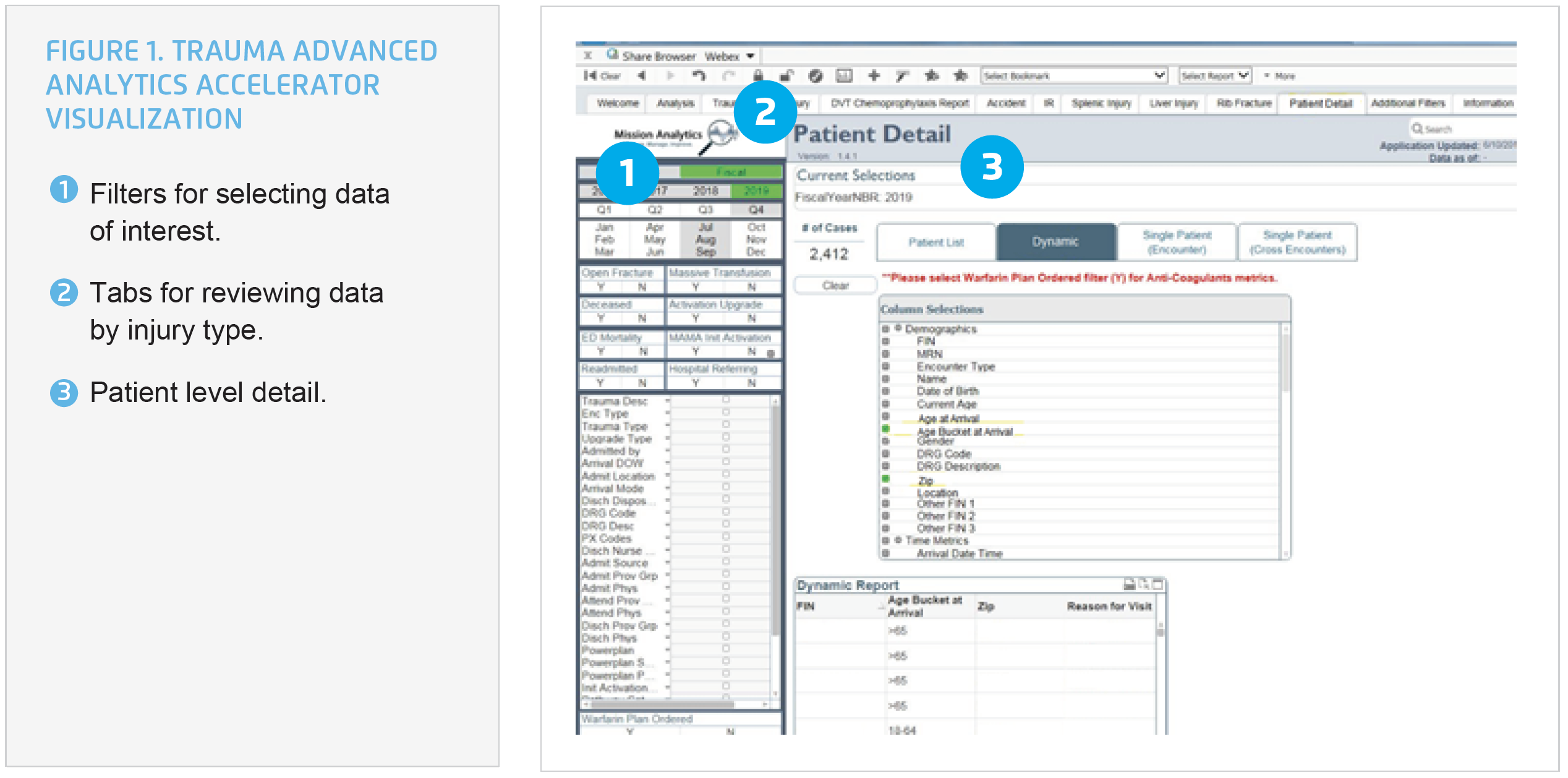
Using data from the analytics accelerator, the trauma program began investigating its trauma alert Level II activations—known as a modified trauma—which indicate a suspected potential injury based on the mechanism of injury. The team discovered that more than 50 percent of trauma activations are for geriatric patients.
The trauma team further investigated the data and evaluated response time by both injury type and by age groups to discover that not all geriatric trauma patients arrived as trauma activations, inadvertently delaying the allocation of the resources required for timely, effective trauma care. Timely identification of geriatric trauma patients, accurate recognition of their injuries, and early, aggressive treatment for their injuries are essential for improving geriatric patient outcomes. While younger patients can tolerate an injury (e.g., a rib fracture) for a longer period of time, geriatric patients cannot and decompensate much more quickly than their younger counterparts.
The team evaluated the time of trauma team arrival for geriatric patients and identified the opportunity to improve the timeliness of care, changing processes and the expected response time to ensure geriatric patients receive care in a timelier manner. It then evaluated and improved its Level II trauma activation processes, re-affirming with the trauma team the expected response time and workflows. To improve the timeliness of care, the team also altered the ED workflow, initiating care within the ED that was previously not initiated until the patient was admitted to the inpatient unit.
Using the analytics application data, the trauma program can monitor trauma level activations, and the timeliness of trauma team arrival, providing feedback to the teams about their performance. When the team does not meet the expected arrival time, the trauma program can quickly identify why, remove barriers, and ensure timely trauma team arrival moving forward. The trauma team can visualize the impact of time to arrival on patient outcomes, including ED LOS.
RESULTS
Access to timely data has allowed Mission’s trauma program to improve the timeliness of the trauma team arrival for Level II trauma patients. Results include:
- Trauma team arrival for patients triaged as Level II trauma activation:
- 34.2 percent relative reduction in arrival time for patients ages zero to 17.
- 30 percent relative reduction in arrival time for patients ages 18 to 64.
- 33.7 percent relative reduction in arrival time for patients over age 65.
- LOS for patients with Level II trauma activation:
- 21 percent relative reduction in ED LOS for patients ages zero to 17.
- 19.2 percent relative reduction in ED LOS for patients ages 18 to 64.
- 11.9 percent relative reduction in ED LOS for patients over age 65.
- $17K in cost avoidance, the result of reducing ED LOS for Level II trauma activation.
“We have the opportunity to do things that we could only dream about 12 months ago”
– William Shillinglaw, DO, Medical Director Trauma/Critical Care Services, Mission Hospitals
WHAT’S NEXT
As a data-driven organization, Mission plans to continue to expand and grow the use of analytics across the organization.
REFERENCES
- The American Association for the Surgery of Trauma (n.d.). Trauma facts.
- Raja, A., & Zane, R. D. (2019). Initial management of trauma in adults. UpToDate.
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.