Sepsis: The Impact of Timely, Trustworthy Data and a Systemwide Approach to Care Improvement

- Deployed systemwide visibility into sepsis care performance
- Improved compliance
- Improved acknowledgement of the first alert that a patient might be at risk for sepsis by 19 percent across the system
- Reduced manual data collection by 97 percent
EXECUTIVE SUMMARY
For patients with the severest form of sepsis, the chance of survival decreases by 7.6 percent for every hour that antimicrobial treatment is delayed. Coordinated team work and the speed with which recognition, diagnosis, and treatment of sepsis occur are critical. Health systems across the country have discovered that by successfully engaging clinicians in driving and maintaining best practice interventions they are able to save lives and improve patient outcomes.1
At Piedmont Healthcare, the work of educating clinicians on the importance of following sepsis care best practices had been done. The missing pieces were a well-resourced, systemwide improvement team focused on improving sepsis, and a concise way to view and give timely feedback on performance based on accurate, trusted data. To fill in these missing pieces, Piedmont created a cross-representative sepsis improvement team and enabled tracking for compliance to best practices with an analytics application from Health Catalyst.
Within just three months of deploying the Sepsis Improvement Application, Piedmont has accomplished significant improvements in efficiency—and completely won trust in the data. Piedmont has already identified early indications of patient outcome improvements. Initial achievements of its sepsis improvement team include the following:
- Deployed systemwide visibility into sepsis care performance and best practices compliance
- Improved acknowledgement of first alert by 19 percent across the system
- Reduced manual data collection by 97 percent
THE THREAT OF SEPSIS
Sepsis is a common and often deadly response to an infection. It is vitally important that care teams quickly recognize and treat the condition; indeed, the chances of surviving severe sepsis decrease by 7.6 percent for every hour that antimicrobial treatment is delayed.2 Substantially reducing sepsis’ mortality rates is one of the chief areas of focus for leading health systems today. These organizations recognize that successfully engaging clinicians to follow best practice interventions is an essential component of success.
One such healthcare organization is Piedmont Healthcare (Piedmont), a system of six hospitals with over 125 physician and specialist offices across greater Atlanta and North Georgia. To improve sepsis outcomes, Piedmont implemented the Surviving Sepsis Campaign care bundles 3, specifically, the 3-hour bundle, 6-hour bundle, and early alerts. This case study describes how being able to provide accurate and timely data to clinicians can re-energize a stalled improvement effort and set the stage for meaningful and sustainable clinical practice change.
DATA DISTRUST AND MANUAL PROCESSES
Although efforts to improve sepsis care at Piedmont had been underway for some time, substantive changes in clinical practice were difficult to maintain. Piedmont had no consistent way to view performance on sepsis bundle compliance by facility and provider, or to tie adherence to best practices directly to the impact on length of stay (LOS), mortality, and clinical outcomes.
To audit sepsis performance metrics, Piedmont relied on heavily manual processes—which was especially difficult for the health system’s smaller hospitals with fewer resources. Simply identifying sepsis patients required sifting through three different reports, and then an additional hour was spent on chart audits for each of the identified patients. All told, the work involved in collecting and presenting the findings from sepsis data required the equivalent of one FTE, spread across three people.
Yet for all the time and effort spent, clinicians were deeply skeptical of the accuracy of the data—which by the time it was presented to the clinicians, was very retrospective. Not surprisingly, they were especially doubtful when the data indicated poor compliance with sepsis care best practices. With levels of compliance to best practice bundles being so difficult to monitor and sustain, sepsis improvement had stagnated.
A “BIG PICTURE” VIEW INTO SEPSIS IMPROVEMENT
Piedmont clinicians had been well educated about the importance of following best practices for sepsis care, but that alone wasn’t enough to sustain an ongoing change in practice. Piedmont needed a systemwide sepsis improvement team with a strong physician champion, and it needed a clear and simple way to view clinical and financial performance data and bundle compliance based on timely, trustworthy data. To that end, Piedmont implemented the solutions below.
Systemwide sepsis improvement team for sustained change
In order to deploy a standardized approach to sepsis care improvement, Piedmont made sure its sepsis improvement team included strong representatives from each hospital across the system. These team members included an engaged physician champion, expert clinical leadership, a proficient program manager, and active leadership support, which Piedmont knew was critical to sustaining improvement.
Data validation process for clinician buy-in
Piedmont determined that an analytics application was essential for tracking sepsis clinical outcomes and compliance with best practices and guidelines. In order to deploy an application that would be trusted by physicians, nurses, and financial staff alike, the improvement team first undertook a meticulous data validation process. An ad hoc group of team members from finance and coding met together with clinicians from the ED, ICU, and acute floors to review and validate data. Clinician acceptance of the data was achieved once they saw full agreement between the data from the application and data that they had personally obtained from manual chart audits.
This validation effort, done effectively and efficiently, was completed in weeks. Piedmont was pleasantly surprised by the level of engagement it generated. It became clear that asking clinicians what data they wanted to view and how they preferred to view it was the engagement these clinicians needed in order to trust and “own” the data—and make changes in their sepsis care practices.
Sepsis Improvement Application to bring accountability
Having gained clinician engagement and trust in the data through the validation process, Piedmont was able to bring its Sepsis Improvement Application from Health Catalyst into effective use very quickly.
Research shows that near real-time feedback impacts people when they still remember their actions, and without the ability to show clinicians how they were doing in real-time, data was easy to dismiss 4 The application’s interactive visualization features now allow the sepsis improvement team to quickly and precisely show executives, managers, and front line staff exactly how well the health system and/or individuals are adhering to the best practice 3-hour bundle, responding to early sepsis alerts, and how this performance directly impacts LOS, mortality, cost, and patient outcomes (see Figure 1).
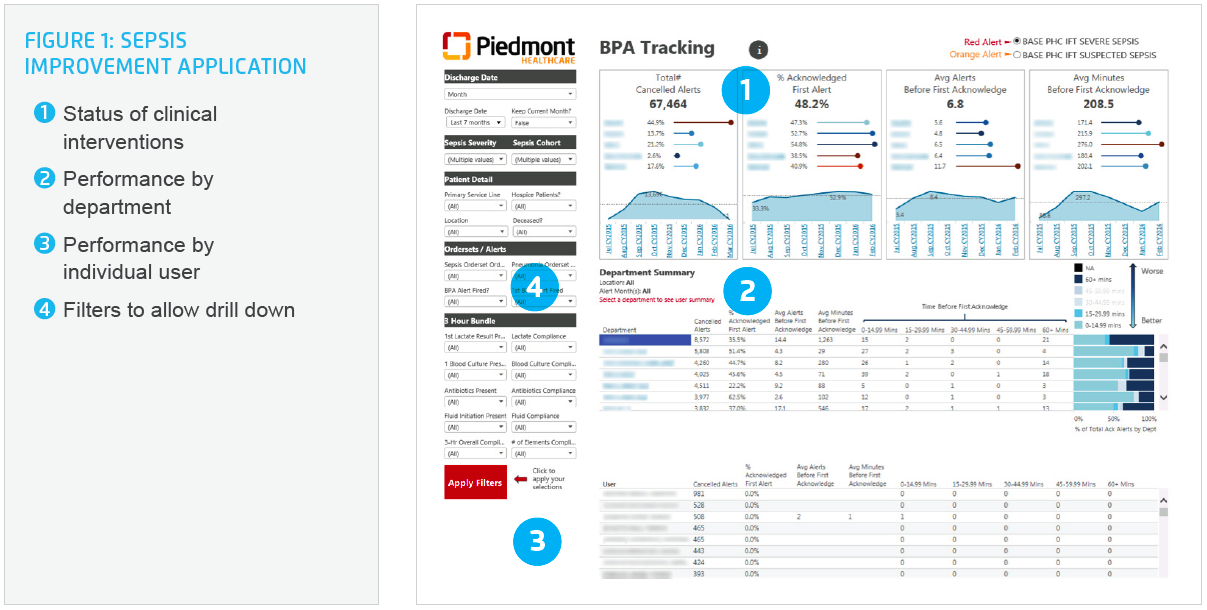
Additionally, tying clinical and financial data in one analytics application enables the clinicians to see the broad picture of how sepsis effects LOS, mortality, outcomes, and costs—and how following sepsis care best practices has a direct impact on these factors.
Informed by accurate, near real-time individual feedback, clinicians are motivated to make adjustments to their practice. Seeing the difference in patient outcomes, based on the number of elements of the 3-hour bundle the patient received, moves the discussion at the improvement team and leadership team levels beyond arguments about best practice to collaboration about how to improve.
Meanwhile, putting near real-time information into the hands of the unit managers enables them to easily monitor compliance on their unit with interventions. For example, the unit manager on the Intermediate Cardiac Unit focused on responses to early sepsis alerts which use an algorithm to let clinicians know when a patient might be at risk for sepsis so that they can intervene earlier with lifesaving measures. Cancelled alert rates have dropped by 42 percent now that the unit manager is able identify issues and intervene with education when necessary.
Automated sepsis care compliance monitoring
The new analytics application has eliminated the need to do manual chart audits to report sepsis performance, a process that had taken three people many hours each month. Now it takes place in less than five minutes via online interactive data mining. Information is widely available to clinicians, managers, and executives in a way that allows them to drill down to determine the source of variation and tie it to clinical outcomes. Seeing the manpower previously expended on manual chart audits diverted to actual process improvement is a motivating force for clinicians at Piedmont.
RESULTS
Within just three months of deploying the Sepsis Improvement Application, Piedmont has accomplished significant improvements in efficiency—and completely won trust in the data. Piedmont has already identified early indications of patient outcome improvements. Major achievements of its sepsis improvement team include the following:
- Deployed systemwide visibility into sepsis care performance with an analytics application that creates clean and concise views based on trusted data and a culture of transparency
- Improved compliance with best practice and reinvigorated an improvement initiative through data visibility and feedback on performance on best practice bundles and alerts
- Improved acknowledgement of the first alert that a patient might be at risk for sepsis by 19 percent across the system— and even more dramatic improvement has been realized in some units, such as the 42 percent reduction in cancelled alert rate seen in the Intermediate Cardiac Care Unit
- Reduced manual data collection by 97 percent:
- Eliminated the need for 480 chart reviews per year in one facility alone
- Wait time for reports eliminated due to access to near realtime data in analytics application
- Replaced manual chart audits with less than five minutes of online interactive data mining on selected patients
- An estimated one FTE spread among three people across the system was refocused from data gathering to data analysis and quality improvement
- All manual sepsis reports eliminated
“The biggest impact we’ve had with the Health Catalyst partnership on the sepsis care initiative is quickly cutting through the EMR data piles and compiling information in usable, understandable dashboard displays that everyone can get their mind around regarding where we are and where we should be.”
– Dr. Chad Case
Medical Director of Critical Care
WHAT’S NEXT?
By end of the fiscal year, all clinical managers will be up and running on the analytics platform to drive sepsis process improvement at the unit level. This will enable the immediate feedback on performance to the individual clinicians, units and hospitals that has been found to be so effective in other organizations. But access and visibility are already having an impact—and Piedmont is confident it has now set the stage for substantive and sustained reductions in LOS, mortality, and improved patient outcomes as education about the use of the application rolls out across all units and all hospitals in the system.
Piedmont discovered the power of putting relevant, accurate, and timely data into the hands of those who can do something with it. The result is nothing less than a cultural shift to continuous improvement and accountability.
REFERENCES
- Schorr, C. (2009). Performance improvement in the management of sepsis. PubMed, 25(4), 857-67. doi: 10.1016/j.ccc.2009.06.0052.
- Wergin, J. (2015). Sepsis: Combating the Hidden Colossus. ECRI Institute, Healthcare Risk, Quality & Safety Guidance.
- Surviving Sepsis Campaign. (2015, April). Surviving Sepsis Campaign Bundles.
- Johns Hopkins Medicine. (2015, April 17). ‘Real-time’ feedback, ‘pay for performance’ improve physician practice, hospital safety. ScienceDaily. (2016, March 14)
ABOUT HEALTH CATALYST
Health Catalyst is a mission-driven data warehousing and analytics company that helps healthcare organizations of all sizes perform the clinical, financial, and operational reporting and analysis needed for population health and accountable care. Our proven enterprise data warehouse (EDW) and analytics platform helps improve quality, add efficiency and lower costs in support of more than 50 million patients for organizations ranging from the largest US health system to forward-thinking physician practices.
For more information, visit healthcatalyst.com, and follow us on Twitter, LinkedIn, and Facebook.
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.