How Texas Children’s Turned Child Diabetes Management into a Community Cause

- 34.4 percent relative improvement in the percentage of patients with diabetes who received the influenza vaccine.
- 26.3 percent relative improvement in pediatric provider diabetes knowledge.
- 90 percent of patients now have individualized school packets developed and available in the EHR.
Patients with diabetes are at a high risk for infections and substantial complications, including the risk of death from infections. Further, social determinants in these patients’ communities have a tremendous influence on their health.
Texas Children’s Hospital, ranked as one of the top four Best Children’s Hospitals by U.S. News & World Report, recognized that there were gaps in diabetes care coordination in the community—where the majority of a child’s diabetes management takes place. The hospital initiated a coordinated community response, aided with an analytics platform, which is setting the standard for community management of pediatric diabetes.
CHILDREN WITH A DAUNTING CONDITION NEED CONCERTED SUPPORT
Texas Children’s Hospital is a leader in the research and treatment of children with diabetes, and evaluates more than 2,500 diabetes cases annually. As such, the children’s hospital is well aware that certain social determinants directly impact a person’s health.1 These range from resources available in the home and neighborhood, such as proximity to quality schools, libraries, and parks and playgrounds, to availability of clean air, water, and food. Indeed, zip code is a stronger predictor of health than a person’s genetics.2
Further, children whose parents did not graduate from high school have additional barriers to health, as lower education levels are directly correlated to lower income, a higher incidence of smoking, and a shorter life expectancy.
Texas Children’s knew that addressing such social and environmental determinants requires broad-based population health interventions. Preventative care is also particularly important for patients with diabetes, as they are at a higher risk of infections and related complications.3 This story describes how the children’s hospital invigorated a broad-reaching, effective community response to managing a serious disease that is on the rise in our nation’s children.
DIABETES: DIAGNOSED IN THE CLINIC BUT MANAGED IN THE COMMUNITY
By and large, management of a child’s diabetes takes place outside of the clinic—in the child’s home, school, and community. A diabetes diagnosis affects the entire family; in a school-age child, a diagnosis also affects the child’s friends and schooling. Unlike many other diseases, effective treatment of diabetes requires that both the patient and his or her family understand the disease process, how to effectively manage nutrition, physical activity, glucose monitoring, and psychosocial challenges.
Coordination between the pediatrician, endocrinologist, family, and school is critically important for patient safety. It can also assure that the child is able to achieve his or her highest goals and live a healthy, fulfilling life. For such collaboration to happen, everyone involved in the child’s care needs to be confident that they possess the foundational knowledge to capably manage the plan of care. They also need to keep one another informed of any changes.
A need for tighter collaboration. Texas Children’s identified gaps in coordination of care among the many people involved in the care of their pediatric patients with diabetes, as well as gaps in care related to preventative activities, like influenza vaccination to prevent the flu. At times, pediatricians, primary care providers, and endocrinologists were not on the same page regarding the patient’s plan of care. Variation in knowledge about diabetes identification and management was believed to be contributing to somewhat late recognition of diabetes, in turn delayed diagnosis and the start of care.
Just as seriously, school nurses were often unaware of the plan of care for the patient—even though the school plays an incredibly important role in the patient’s safety, especially with ensuring the patient maintains effective glycemic control while at school. The existing informational school packets were word documents, with multiple versions, and were not easily accessible, ultimately limiting their effectiveness.
Keeping the flu at bay. Texas Children’s also knew that the rate of influenza vaccinations in its patients was below national benchmarks. People with diabetes are at high risk of serious complications from the flu, including hospitalization and sometimes even death.4 Influenza vaccination to prevent the flu is incredibly important for patients with diabetes.
With these challenges facing some of its most vulnerable patients, Texas Children’s set out to formulate a strategy that would improve foundational knowledge and communication among all of those involved in the care of pediatric patients with diabetes, along with a strategy to improve the rate of influenza vaccinations.
SETTING A STANDARD FOR COMMUNITY DIABETES CARE
The Diabetes and Endocrinology department at Texas Children’s created an innovative diabetes outpatient program that provides coordinated, family-centered, multidisciplinary care to their patients and families.
To speed and expand on improvements, a physician-led multidisciplinary Diabetes Care Processes Team (CPT) was established. The Community CPT, one of five Diabetes CPT subteams, was developed to improve community collaboration and community interventions. It is a physician-led team comprised of parents, primary care providers, pediatricians and endocrinologists from Texas Children’s and the community, and social workers. The Community CPT had two immediate goals: improve flu shot compliance to at least 80 percent, and add improved school packets to the EHR of at least 80 percent of school-age children.
PROMOTING THE INFLUENZA VACCINATION TO PATIENTS WITH DIABETES
The Community CPT developed a strategy to improve the flu vaccination rate that required the entire interprofessional team to work together. First, the registered nurse (RN) or medical assistant (MA) offered the vaccine at the beginning of the visit rather than the end, with efforts taken to assure these medical professionals understood the importance of the vaccine for their patients with diabetes. Texas Children’s listened to the feedback from parents, who indicated that it would be helpful if they received a reminder to help ensure their child received the vaccine. Automated voice messages from the Chair of the Endocrinology department were sent to each parent as a reminder of the start of flu season and the vaccine’s availability. Reminders were also distributed via the EHR to all eligible patients. Finally, posters from the CDC that advised the influenza vaccine for patients with diabetes were prominently displayed in all the clinics.
THE ROLE OF ANALYTICS IN RAISING AWARENESS
Analytic tools are an essential aid for the Community CPT’s efforts to improve community diabetes care, including to identify opportunities for improvement. The team uses the Health Catalyst Analytics Platform built using the Late-Binding™ Data Warehouse architecture (EDW) and a pediatric diabetes application.
The EDW supplies near real-time data to monitor influenza vaccination rates, and midway through the flu season, the team uses the pediatric diabetes application to quickly assess the effectiveness of their strategy and review influenza vaccination rates. Those patients who have not yet received a vaccination are sent an additional reminder, informing them of the availability and importance of the vaccine.
IMPROVING DIABETES CARE COORDINATION IN THE COMMUNITY
The Community CPT is increasing their involvement in the community, taking advantage of local events as an opportunity to educate the public about diabetes. Increased education may contribute to earlier identification of children with Type 1 diabetes and allow for earlier treatment. Because pediatricians are often the first to identify that a child may have diabetes, a recent educational offering targeted pediatric providers in the community, focusing on diabetes, recognition, and effective medical management.
Creating health heat maps. Understanding that social determinants heavily influence health status, the Community CPT is beginning to use geographic data from the EDW, in addition to claims data, to identify areas of potential need. For example, zip code data is analyzed in relation to HbA1c, an indicator of blood glucose control. The team is able to use geographic data to identify which areas have a higher concentration of patients with elevated HbA1c. Disproportionate increases in HbA1c among a group in a particular geographic area suggests barriers to effective care or other needs unique to the geographic area, revealing a community that is in need of additional education and support.
Distributing individualized school packets. To improve community care for school-age children, the Community CPT targeted improvement of the school packets. These are now individualized for each child, and include important information about how to best manage the child’s diabetes, such as information about insulin dosing, sick day management, and contact information for Texas Children’s staff. Adding the endocrinologist’s name has improved the ability for the school nurse or pediatrician to know who is managing the child’s diabetes, should they need to contact this care provider.
Standardization of the school packets was a big endeavor, requiring input and contributions from many stakeholders. For example, certified diabetic educators reviewed the content included in the packets to ensure its accuracy and that the relevant education points were included. Staff in the clinic participated, assuring that school packets were developed for each school-age child with diabetes, and updated the packets to include the most recent plan of care for the patient.
IT support also assisted by making the school packets readily available in the EHR. This step ensured the packets available to all provider offices with access to the EHR, even those outside of Texas Children’s.
RESULTS
The Community CPT is positively affecting community health, with closer diabetes care coordination for pediatric patients with diabetes.
- 34.4 percent relative improvement in the percentage of patients with diabetes who receive the influenza vaccine, exceeding their 80 percent target (see Figure 1).
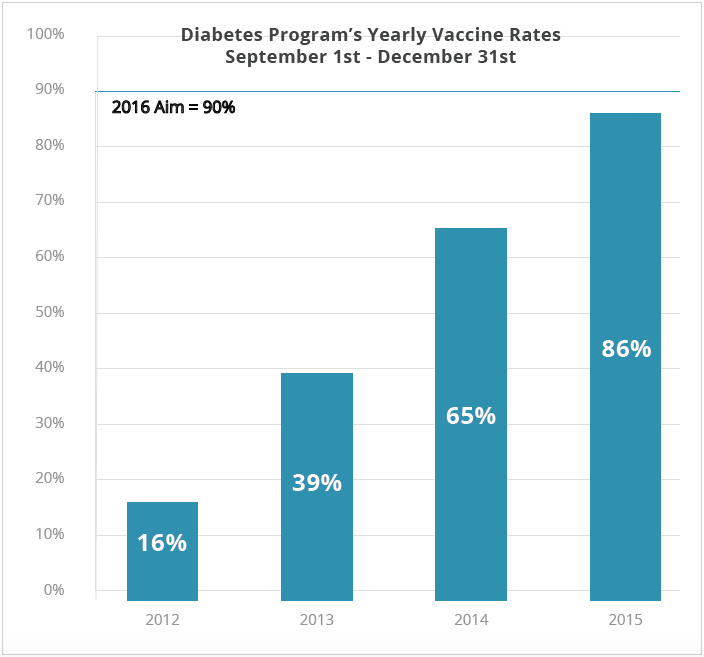
- 26.3 percent relative improvement in pediatric provider knowledge, measured by pre- and post- tests, following completion of the pediatric provider diabetes education sessions. More than 140 pediatric providers attended the education sessions.
- 90 percent of patients now have individualized school packets available in the EHR.
“Using our analytics tools, we pulled flu shot rates, and identified that as an area where we were falling behind. We now use our population health analytics application to follow our data in real-time and make course corrections to improve our flu shot compliance.”
– Bonnie McCann-Crosby, MD
Diabetes and Endocrinology
WHAT’S NEXT
The Community CPT plans to build upon their success in improving the influenza vaccination rate, aiming to achieve at least a 90 percent vaccination rate this flu season. Longer-term goals include increased use of geographic data as a part of ongoing community/population health assessments. Use of this data will allow Texas Children’s to target interventions for those communities at the greatest risk—and build on the hospital’s proactive approach to involving all who can make a positive difference.
REFERENCES
- Office of Disease Prevention and Health Promotion. (2016). Social determinants of health. HealthyPeople.gov.
- Heinman, H. J. & Artiga, S. (2015). Beyond health care: The role of social determinants in promoting health and health equity. The Henry J. Kaiser Family Foundation.
- Casqueiro, J., Casqueiro, J., & Alves, C. (2012). Infections in patients with diabetes mellitus: A review of pathogenesis. Indian Journal of Endrocrinology and Metabolism. S27-S36. doi:10.4103/2230-8210.94253
- Centers for Disease Control and Prevention. (2016). Flu and people with diabetes.
ABOUT HEALTH CATALYST
Health Catalyst is a mission-driven data warehousing and analytics company that helps healthcare organizations of all sizes perform the clinical, financial, and operational reporting and analysis needed for population health and accountable care. Our proven enterprise data warehouse (EDW) and analytics platform helps improve quality, add efficiency and lower costs in support of more than 50 million patients for organizations ranging from the largest US health system to forward-thinking physician practices.
For more information, visit healthcatalyst.com, and follow us on Twitter, LinkedIn, and Facebook.
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.