Measuring and Reporting The Joint Commission’s Perinatal Core Measures using Clinical Analytics

“Now we have data about our pregnancy cohort that we can discuss, that we can disseminate, and that we can use as a baseline. This is a huge achievement for us. The process of gathering this data showed us the areas where we can optimize our EHR to lead to more discrete data capture. Improving our data capture processes at the point of care will significantly improve the accuracy of our reporting and reduce the time we spend performing manual chart extractions.”
– Susanna Swart, RN, Nursing Supervisor
- Established a Women and Newborns population health analytics platform
- Identified data quality issues and developed accurate baseline metrics
- Increased clinical productivity
Antenatal steroid administration is one of five perinatal core measures that The Joint Commission (TJC) is implementing nationwide.1 Beginning in 2014, all hospitals with 1,100 or more live births per year must report their performance against these measures to TJC for accreditation.
Research shows that administering a full course of antenatal corticosteroids to women at risk of a preterm birth reduces morbidity and mortality rates among newborns. Specifically, these corticosteroids reduce the risk of complications of prematurity such as respiratory distress syndrome, intraventricular hemorrhage and perinatal death.
Texas Children’s Hospital, one of the most highly regarded children’s hospitals in the nation, was determined to ensure that its perinatal care processes met the latest evidence-based care standards. Texas Children’s leaders began this effort by systematically incorporating and measuring the use of corticosteroid therapy protocol for at-risk obstetric patients.
“In the past, the manual reports that we relied on to track our performance on this measure were six to nine months old — and, it turns out, very inaccurate. Using this new analytics platform, we learned that our corticosteroid administration rate was, in fact, far higher than we had thought. We can now track our performance in near real time and use this same platform to tackle other perinatal care measures.”
Frances Kelly, MSN, RNC-OB,NEA-BC, CPHQ, PhD(c)
Director of Quality and Safety for Texas Children’s Pavilion for Women
ESTABLISHING AN ANALYTICS FOUNDATION FOR IMPROVED PERINATAL CARE
Texas Children’s has long been committed to the triple aim of improving outcomes and the patient experience, while reducing costs. The hospital invested in a technology-driven approach to improving its care processes, implementing an enterprise-wide electronic health record (EHR). Then, realizing that the EHR alone couldn’t meet their needs, they engaged Health Catalyst, a healthcare enterprise data warehouse (EDW) and analytics vendor, to implement an analytic, deployment, and content – three system framework – for optimized care delivery.
This framework introduced an EDW to improve clinical analytics throughout the organization. Health Catalyst’s EDW platform organized the system’s data into a single source of truth that serves as a foundation for continuous clinical quality improvement initiatives throughout Texas Children’s.
When Texas Children’s determined to address TJC’s perinatal core measures, applying Health Catalyst’s framework for clinical improvement to this area was the logical approach. The framework incorporates more than just analytics technology. It also involves creating permanent, integrated workgroup teams that identify areas for care improvement, and support the development and measurement of evidence-based care practices.
Texas Children’s had assembled a workgroup to oversee improvement strategies for its Women’s Services and Newborn departments – and to address the perinatal core measures. This group included a quality chief for obstetrics and gynecology, physicians and professors in obstetrics and maternal fetal medicine, and directors of quality and system’s integration from the hospital’s quality department and Evidence Based Outcomes Center.
Using a modified Delphi technique, this workgroup selected antenatal steroids as the TJC measure on which to initially focus performance improvement work. The hospital’s initial EHR data indicated that, among the obstetric patients who delivered between 24 and 32 weeks of gestation, the rate of administering a full course of antenatal steroids was very low – around 30 percent. This team believed that this measure would lend itself to interventions that could be rapidly deployed and measured.
The workgroup was aware upfront of the challenges they faced with this clinical improvement project. One of the biggest challenges was incomplete data. Clinicians could not simply rely on the inpatient EHR, because many patients were transferred to Texas Children’s Pavilion for Women from other facilities or outpatient settings, where a steroid course may have been initiated or fully administered. In many of these cases, the medications were not recorded as discrete data within the inpatient EHR, precluding automated data capture.
Rather, it could be documented in multiple locations within the patient chart, including as a narrative in history and physicals and clinical progress notes. This limitation required Texas Children’s nurses to perform manual chart abstraction to locate the necessary data. An additional challenge was the lack of a systematic process for documenting which charts they had reviewed, or the results of that review. A tracking method was needed to ensure that charts were reviewed once, and the results recorded to maximize efficiencies and provide a complete and accurate history of antenatal steroid therapy.
IMPLEMENTING AN ANALYTICS PLATFORM FOR PERINATAL CARE
Critical to the success of establishing the analytics platform for antenatal steroids was the formation of a team to guide its development and implementation. The interprofessional team dedicated to the antenatal steroid project – a team that reported up to the original workgroup – consisted of a nurse in the women’s clinical program, an assistant director of nursing, the quality and safety director of the Pavilion for Women, a data architect and a representative from finance.
The following are the team’s principal accomplishments to date:
Established a Women and Newborns population health analytics platform
Working together and interacting with the data from the EDW, the team followed an Agile development process that delivered rapid time to value. They implemented the Health Catalyst Population Analytics Advanced Application – Antenatal Steroid module to run on the existing EDW platform. In just eight weeks, they had defined and identified their cohort of patients, designed the dashboards and visualizations and had the platform ready to drive clinical improvement at the point of care. The interactive, Agile development process cemented the team’s confidence in the data coming from the analytics application.
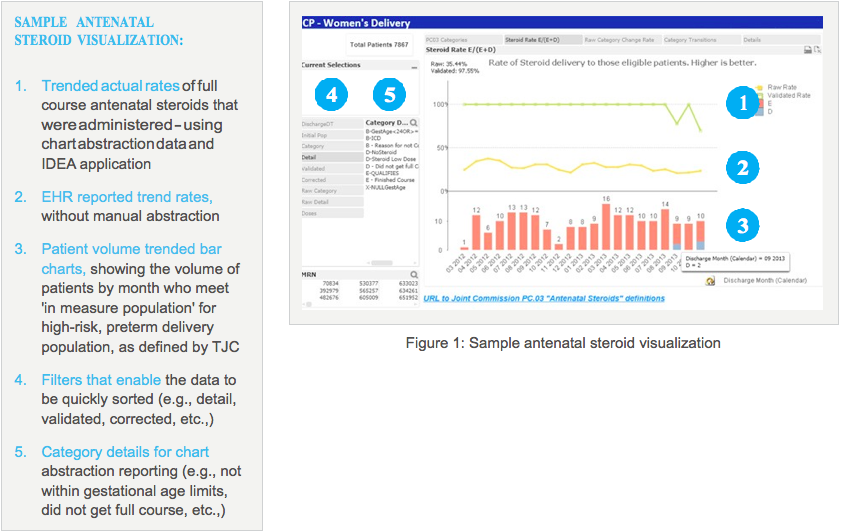
The analytics module, shown in Figure 1, enabled the team to consume at a glance the information they needed to track performance on the antenatal steroids measure.
With this platform in place, Texas Children’s has achieved level four of the Healthcare Analytics Adoption Model (analytics that enable regulatory reporting) and level six (analytics for population health management). Most importantly, this analytics platform can now be leveraged for improvement projects in other Women and Newborns care process families.
Identified data quality issues and developed accurate baseline metrics
The population health analytics platform helped TCH understand its perinatal core measure performance much more accurately. Whereas the EHR indicated that the rate of administering a full course of antenatal steroids was approximately 30%, the EDW platform and clinical analytics revealed that the true rate was actually close to 98%, as shown in Figure 1. The team is now able to accurately refect and measure the trended data – and focus their resources on other clinical quality improvement initiatives. Additionally, they can now leverage the platform to expand their clinical quality improvement programs to encompass the remaining four TJC perinatal core measures, as well as hospital acquired conditions such as surgical site infections following a cesarean section.
Increased clinical productivity
Nurse chart abstractors previously lacked a systematic process for documenting what charts they had reviewed and recording the results. Health Catalyst deployed the IDEA application, which enables the chart abstractor to document that the chart was reviewed and where antenatal steroids were administered.
Nurses now spend less time examining the charts because they have an application where they can quickly document their findings and mark a chart as reviewed. The workgroup is collaborating with the informatics team to create a discrete data field for this purpose within the EHR. Implementing this change should further reduce nurse abstraction time.
The perinatal care team can also use the analytics application visualizations to quickly and easily share their results with clinical and executive teams. This level of self-serve analytics enables the team to filter and view the data easily themselves without asking for multiple reports from data analysts.
References
- The four other perinatal core measures include early elective delivery, nulliparous term singleton vertex (NTSV) cesarean section, healthcare-associated bloodstream infections in newborns and exclusive breast milk feeding.
ABOUT HEALTH CATALYST
Based in Salt Lake City, Health Catalyst delivers a proven, Late-Binding™ Data Warehouse platform and analytic applications that actually work in today’s transforming healthcare environment. Health Catalyst data warehouse platforms aggregate and harness more than 3 trillion data points utilized in population health and ACO projects in support of over 22 million unique patients. Health Catalyst platform clients operate 96 hospitals and 1,095 clinics that account for over $77 billion in care delivered annually. Health Catalyst maintains a current KLAS customer satisfaction score of 90/100, received the highest vendor rating in Chilmark’s 2013 Clinical Analytics Market Trends Report, and was selected as a 2013 Gartner Cool Vendor. Health Catalyst was also recognized in 2013 as one of the best places to work by both Modern Healthcare magazine and Utah Business magazine.
Health Catalyst’s platform and applications are being utilized at leading health systems including Allina Health, Memorial Hospital at Gulfport, MultiCare Health System, North Memorial Health Care, Providence Health & Services, Stanford Hospital & Clinics, and Texas Children’s Hospital. Health Catalyst investors include CHV Capital, HB Ventures, Kaiser Permanente Ventures, Norwest Venture Partners, Partners HealthCare, Sequoia Capital, and Sorenson Capital. Visit healthcatalyst.com, and follow us on Twitter, LinkedIn and Facebook
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.