A More Accurate Sepsis Identification Method: Leveraging Physiological Data
Health experts estimate that sepsis, a life-threatening condition that occurs when harmful microorganisms enter the blood or other body tissues, affects 1.7 million people a year in the United States, leading to hundreds of thousands of preventable deaths.
Any health system must meet the challenge of finding and implementing a sepsis identification process, and most organizations can improve the way they handle sepsis care. Rather than the current practice using administrative codes as the only means to determine how care is delivered to patients with sepsis, clinical leaders can consider more effective sepsis identification methods, such as leveraging physiological data.
Traditional Sepsis Identification Methods Leave Opportunity for Improvement
Traditionally, to identify a patient with sepsis, a clinician completes a discharge summary of a patient’s visit. Along with written orders, a patient’s health history, progress notes, and a physical exam, someone in the coding/billing department uses the information from the healthcare provider’s documentation to determine if the patient is septic and at what level of severity. The coding/billing department also determines the cause of sepsis (e.g., pneumonia, pyelonephritis, cellulitis, etc.).
The problem with this administrative, coding-based process is that the coder may assign sepsis as a diagnosis when it isn’t sepsis (it just looks like it should be sepsis), or vice versa. Research also suggests that administrative coders are more likely to diagnose sepsis due to higher levels of sepsis awareness, personal biases, and financial incentives (sepsis has a higher reimbursement rate than other conditions, such as pneumonia) (Figure 1).
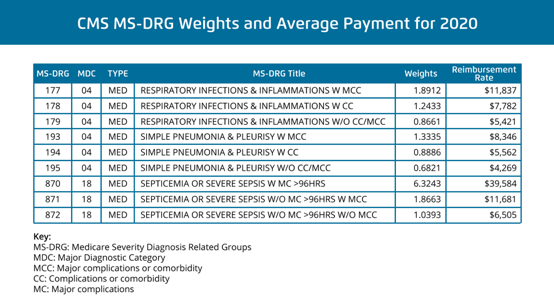
Issues with inaccurate sepsis diagnoses include skewing the number of patients in a health system who, in fact, have sepsis, leading to unreliable sepsis outcomes data. Inaccurate diagnoses also delay the right care for patients who have a condition other than sepsis, leading to worse outcomes.
A New Sepsis Identification Method: Physiological Data
Another approach to identifying patients with sepsis is relying on their physiological data instead of billing codes from clinical documentation. Health systems would use physiological data—such as a patient’s vital signs, signs of organ failure, blood culture orders, and antibiotics prescribed—to determine if the patient is truly septic. While coders regularly diagnose sepsis correctly, the administrative coding method is still not as accurate as relying on a patient’s actual physiological parameters.
In essence, using physiological data, health teams can see a group of patients in two cohorts:
- In a diagnostic cohort, users see what the care team—including the coder/biller—interpret.
- In a physiologic cohort, users see only what the patient’s physiological data tells them, removing any biases or anecdotal information that could be misleading or incorrect.
The Right Tools Lay the Foundation for Successful Sepsis Management
Better sepsis management starts with an understanding of the role physiological data plays in sepsis identification. However, health systems can only go so far without the right tools. Data management tools, like a robust data warehouse and analytics platform, play an essential role in early sepsis identification. Without the ability to access physiological data and customize the sepsis criteria based on a hospital’s unique needs, health systems reach an impasse.
The Centers for Disease Control and Prevention(CDC) created a toolkit that health organizations can use to create a cohort based on physiological data. The toolkit includes in-depth instructions about highest-priority factors to identify and track, helping care teams know which patients to define as septic.
Health systems can also leverage the Health Catalyst® Sepsis Analytic Accelerator to guide sepsis development and improvements around any of five specific areas:
- Early recognition in the emergency department.
- Bundle compliance.
- In-house sepsis recognition: The Health Catalyst Patient Safety Monitor™ Application.
- Compliance to Society for Critical Care Medicine and Surviving Sepsis Campaign care guidelines.
- Readmissions.
After health systems have identified and implemented sepsis improvement interventions, leaders can leverage advanced benchmarking tools, such as the Health Catalyst Touchstone™ application, to compare sepsis improvement results with other systems to serve as a benchmark throughout the improvement process.
Using tools like the CDC’s toolkit together with the Sepsis Analytic Accelerator and Touchstone will help health systems guide their sepsis management efforts and offer course correction before any intervention is too far off track. With the right tools, improvement teams can regularly track sepsis rates and understand if their interventions are making a difference.
A Clinical and Scientific Lens Leads to Accurate Sepsis Data
Filtering cohorts based on physiological parameters has benefits in addition to increased accuracy. It is a more clinical and scientific, and therefore objective, approach to patient identification, eliminating anecdotal information from a doctor’s notes—such as “patient seemed fatigued and short of breath”—and instead looking at a patient’s oxygen levels. Physiological filtering also removes the incentive to bill for sepsis, as it is a higher paying reimbursement.
As health systems begin to look at patient data related to a physiological sepsis cohort, in particular the process metrics for treating sepsis (e.g., three-hour bundle metrics), leaders will likely see that patients in the physiologic cohort respond significantly better to the interventions because those patients are actually septic, compared to part of a cohort inaccurately coded as septic. Patients who are not actually septic won’t respond as favorably to specific sepsis interventions, leading to inaccurate data and wasted resources. The data from the physiological cohort not only helps providers administer the right interventions to treat the right patients, but offers additional opportunities to improve care because the right patients are being diagnosed with sepsis earlier, leaving more time for providers to intervene.
With a new cohort based on the body’s unbiased, objective physiological information, health teams will learn that the actual sepsis population is most likely lower than the numbers in the coded population. Increased accuracy in sepsis rates should potentially demonstrate a decrease in other data sets, like sepsis mortality rates.
An Effective Sepsis Identification Method Is Key to Effective Interventions
The traditional coding-based sepsis identification method can be variable and often inaccurate. In a healthcare landscape in which reimbursements are tied to value and margins are tight, health systems must identify the right cohorts to categorize septic patients, allowing providers to intervene as early as possible and deliver the right care to each patient without delay.
As health systems build cohorts for patients with sepsis based on physiological data—rather than relying on a coder to decipher a doctor’s notes—clinicians can provide the correct targeted interventions to patients who are indeed septic. Once an effective sepsis identification method is in place, health systems are free to focus on intervention and helping patients with sepsis get on the road to recovery.
Additional Reading
Would you like to learn more about this topic? Here are some articles we suggest:
- Using Improvement Science in Healthcare to Create True Change
- How to Design an Effective Clinical Measurement System (And Avoid Common Pitfalls)
- Healthcare Quality Improvement: A Foundational Business Strategy
- The Top Six Examples of Quality Improvement in Healthcare
- Population Health Management: A Path to Value
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.

