DSRIP in 2018: Continuing Efforts for Medicaid Reform
As part of the evolving Medicaid programs, Delivery System Reform Incentive Payment (DSRIP) programs have been implemented in thirteen states with the goal of transforming Medicaid in those states. DSRIP programs are not grants but, rather, performance-based incentive programs. They emphasize three concurrent goals for each state:
- Reducing the total medical spend.
- Improving patient outcomes.
- Establishing a direct link between provider performance and payment.
In 2010 California was the first state to implement the DSRIP program. Since then, more states—Alabama, Arizona, Kansas, Massachusetts, New Hampshire, New Jersey, New Mexico, New York, Oregon, Rhode Island, Texas, and Washington—have implemented DSRIP. Each of these states obtained a Section 1115 waiver from the Centers for Medicare and Medicaid Services (CMS). The Section 115 waiver, which is typically in effect for five years, gives states the authority to transform their Medicaid programs and align them with value-based reimbursement. Participating states must agree to budget neutrality, transparency, statewide quality metrics, and frequent reporting of outcomes. Each state’s program is unique in its structure and goal.
Participating DSRIP States and Structures
In general, the DSRIP programs focus on four main areas:
- Infrastructure development.
- System redesign.
- Clinical outcomes improvements.
- Population focused improvements.
Below are the DSRIP states and a few notes on structure:
| State/Program Name | Timeframe | State and Federal funding (Billions) | Provider Structure | Alternative Payment Model |
|---|---|---|---|---|
| Early Programs (approved prior to 2014) | ||||
| California/DSRIP California/PRIME (Public Hospital Redesign and Incentives in Medi-Cal) | 2010-2015 2016-2020 | $6.6B $7.5B | District/municipal public hospitals (39) and designated public hospitals (21) | Goal for 60% of current beneficiaries by end of 2020 |
| Texas/DSRIP | 2011-2016 with extension to 2017 2017-2021 | $15.2B $10.8B | 20 regional health partners with 297 providers | Not in current plan |
| Massachusetts/Delivery System Transformation Initiative (DTSI) Massachusetts/DSRIP | 2011-2017 2017-2022 | $13.1B $1.8B | ACO and community partners (34) | Yes |
| New Mexico/Hospital Quality Improvement Incentive Program (HQII) | 2015-2018 | $29M | MCO and 29 hospitals | N/A |
| New Jersey/DSRIP | 2014-2017 | $573M | 49 Participating hospitals | N/A |
| Kansas/DSRIP KanCare | 2014-2017 | $60M | 3 MCOs and 2 hospitals | N/A |
| Recent Programs (approved after 2014) | ||||
| New York-DSRIP | 2014-2019 | $12.8B | 25 PPS that work with hospitals and nonhospital | Goal to move 80-90% to value-based |
| Oregon- Hospital Transformation Performance Program (HTPP) | 2012-2018 | $600M | 28 urban hospitals | None |
| New Hampshire-DSRIP | 2016-2020 | $150M | IDN for behavioral health | Roadmap for 50% |
| Alabama-Integrated Provider System (IPS) | 2017-2022 | $300M | RCO that contract with hospitals and other providers | None |
| Rhode Island-DSRIP | 2016-2020 | $200M | Hospitals and nursing homes | Moving to Medicaid Accountable Entities (AE) |
| Washington-DSRIP | 2017-2021 | $1.1B | Accountable community of health (ACH) that includes providers and community organizations | Move 90% |
| Arizona-Targeted Investments Program | 2016-2021 | $300M | Hospitals and providers | None |
The DSRIP programs that started before 2014 focused on payment enhancement and preservation for safety net providers. The newer (post 2014) DSRIP programs show a greater emphasis on Medicaid payment and delivery system reforms, as well as increased emphasis on mental health programs.
The DSRIP policymakers recognized upfront the need to start with process and move to population improvements over time. This allows for short-term and long-term goals; many program goals were milestones in the journey.
The three state programs below differ in content but share a focus on improving health for the state’s population:
| California | Texas | New York |
|---|---|---|
| • Focusing on prevention. • Improving care for the high-risk, high-cost population. • Reducing overuse and misuse of services. | • Investing in infrastructure (technology, tools, and people). • Promoting program innovation (e.g., testing and replicating care models). • Focusing on quality improvement in at least one outcome (clinical events, experience, cost, or health status). • Focusing on population-focused improvements, including reporting on 83 measures (e.g., admission, readmission, complications, satisfaction, emergency, and medication management). | • Focusing on project requirements and milestones. • Implementing system transformation projects (e.g., care coordination and integrated delivery systems). • Focusing on clinical improvement (e.g., asthma, prenatal care, and cardiovascular, behavioral health). • Implementing population-side chronic disease prevention, prevention of HIV and STDs. |
To support the above areas, providers will need to collect data and report results. All participating states must report standardized measures. Health systems provide general reports to the state semi-annually.
For example, the state of New York requires six types of reports:
- Quarterly progress.
- Semi-annual report on achievements.
- Standards to collect data as often as is practical to move to real time.
- Some metrics reported annually.
- Evaluation by independent contractor.
- Operational performance, which looks at consumer level reports and high-level geographic elements.
The following results from 2011 and 2012 (Figures 1 and 2), publicly available on the New York State Department of Health website, show metrics for hospitalizations and diabetes care:
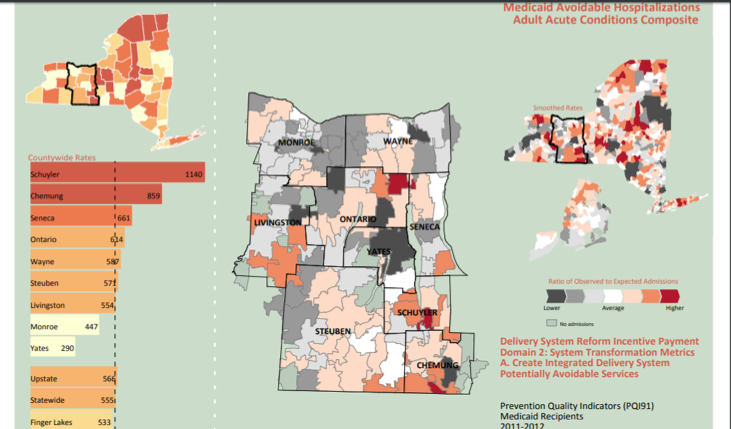
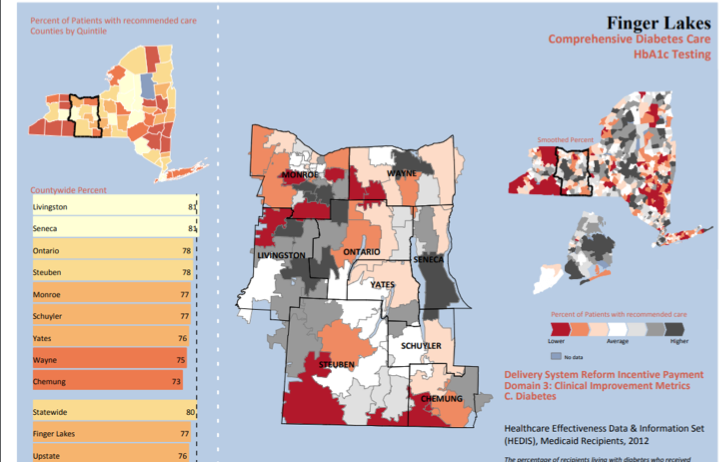
More Momentum Towards Reform in 2018
According to a March 2018 Medicaid and CHIP Payment and Access Commission (MACPAC) issue brief, key policy changes for the more recent waivers increase the emphasis on reform:
- Increased focus on reform goals for the delivery system, less focus on payment preservation.
- Increased emphasis on provider partnerships.
- The addition of statewide performance milestones.
- Increased use of Designated State Health Programs (DSHP) to finance DSRIP investments.
- More standardized monitoring and evaluation requirements.
- Requirements to develop plans for sustaining DSRIP activities through value-based purchasing strategies in managed care.
States Meet the Significant Challenges of DSRIP
States and health systems have had some concerns with DSRIP, as they need to align DSRIP with other Medicaid and value-based programs. Metrics and implementation plans cannot conflict with other initiatives. DSRIP participants, however, are meeting the program’s challenges. Programs in New York state, for example, are meeting high standards:
New York DSRIP Aims for 80 Percent Value-Based Payment
The New York DSRIP program started with the bold goal “to reduce avoidable hospital use by 25 percent through transforming the New York healthcare system into a financially viable, high performing system.” The New York program began in April 2014 and will continue through March 2020. The state required providers and community-based organizations to form Performing Provider Systems (PPS); New York currently has 25 PPSs. By the end of the waiver period, 80 percent of payments to providers must use value-based methodologies.
Finger Lakes Performing Provider System Has Achieved Maximum Incentive
A 2016 article from the Healthcare Finance Management Association describes the experiences of Finger Lakes Performing Provider System (FLPPS), a nonprofit with more than 3,000 providers from 600 organizations. FLPPS members united to provide care to 400,000 Medicaid and uninsured individuals, with several key goals:
- Improve the integrated delivery model for the Finger Lakes region, which includes a population of 100,000 uninsured individuals.
- Smooth the transition from fee-for-service to value-based care by using funds to reward outcomes.
- Build strong collaboration among the providers.
- Begin the journey to population health strategy and management.
DSRIP payments to providers are tied to achieving process metrics; in 2015 around 150 organizations received $23 million in incentive payments. To date FLPPS has achieved 100 percent of the possible award dollars. The organization is working on the next phase of delivery reform to mature the performance goals for each member of the delivery system.
Positive Results, but Impact Is Hard to Measure
Providers have met the milestones and targets but have struggled to isolate the impact of the DSRIP projects against other policy changes. Three states (California, Texas, and Massachusetts) have completed final evaluations for the first time period. To date little evidence exists that DSRIP waivers have significantly improved quality and health outcomes or reduced spending on healthcare services. Several states have shown lower ED visits but are unable to tie this outcome directly to DSRIP.
Despite lack of evidence, DSRIP also has had obvious some overall positive results:
- States, via various organizations, have forged an infrastructure for population health.
- States are collecting data and will be able to increase tracking for services provided to the Medicaid population.
- The diffusion of value-based payment programs will increase if states meet DSRIP goals in the future.
DSRIP’s Potential Impact on Delivery System Reform
DSRIP could be an important program in the pursuit of delivery system reform. Many models may need continued monitoring and measurement. But which models will be successful, and which ones can be replicated to improve our health care system? CMS has initiated this waiver process but has not issued any specific guidance about future requirements. Recent waiver approvals, however, include more accountability and broader list of provider participants. As renewal dates approach, measurement of population and provider results will be important. Comparing the effort to maintain and participate in the program with final outcomes will help participants replicate and scale the population-based movement at the state level.
Seven Must-Haves to Meet DSRIP Requirements
Participating DSRIP states are best positioned to meet DSRIP requirements when they have seven elements in place:
- A next-generation data platform to integrate data from many sources (e.g., the Health Catalyst® Data Operating System [DOS™]).
- The ability to build measures (e.g., avoidable hospitalizations, frequency of necessary screening tests, and results of diabetes care testing).
- DSRIP education for providers.
- An organizational-level commitment to population health.
- Technology to share data and monitor performance.
- An organizational-level evaluation of the potential benefits of participation and the cost of the effort.
- Long-term thought about all organizational strategies (specifically, as care is redesigned for the Medicaid population under DSRIP projects, how does that impact other care process improvements in organizations?).
DSRIP Boosts States Towards Value-Based Care
States that participate in DSRIP and meets its goals gain momentum toward value-base care, as well as rewards for high clinical performance. Without such incentives, states risk remaining in an older fee-for-service system and won’t be prepared as healthcare continually shifts towards a value-based system. By putting in place the seven must-haves for DSRIP above, states are positioned the transform their Medicaid programs and thrive in a value-based environment.
Additional Reading
Would you like to learn more about this topic? Here are some articles we suggest:
This website stores data such as cookies to enable essential site functionality, as well as marketing, personalization, and analytics. By remaining on this website you indicate your consent. For more information please visit our Privacy Policy.

